Third Trimester
Overview
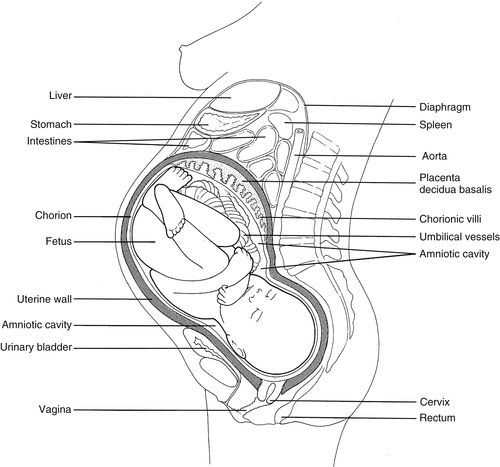
Maternal Anatomy and Physiology
• As discussed in Chapter 11, the female pelvis organs include the genital tract (uterus, vagina, and uterine tubes), bilateral ovaries, urinary bladder, a portion of the ureters, and the rectosigmoid colon. The osseous or bony pelvis forms the outer boundaries of the female pelvic cavity, whereas the skeletal muscles which line the pelvic cavity form the inner boundaries. Refer to Chapter 11 for anatomical specifics and sonographic appearance.
• Chapter 11 also discussed how the menstrual cycle prepares the uterus for implantation by a fertilized ovum. If fertilization does not occur, hormone levels decrease and the nonimplanted endometrial lining of the uterus is shed during menses. If fertilization does occur, it usually takes place within 1 day of ovulation, day 15 of the menstrual cycle, at the ampulla portion of the uterine tube. Fertilization is complete when the ova and sperm fuse to form a zygote or cell mass. The cell mass repeatedly divides into the morula, a cluster of 16 or more cells that leave the uterine tube and enter the uterine cavity on the day 18 or 19 of the cycle. The morula is then transformed into a blastocyst. The outer layer of the blastocyst, the trophoblast will develop into the chorionic membrane, the fetal component to the placenta (temporary organ joining mother and fetus; oxygen and nutrients are transferred from mother to fetus; waste products are transferred fetus to mother). The inner layer of the blastocyst, the embryoblast (or embryonic disk) develops into the primary and secondary yolk sacs (nutrient-filled sacs adjacent to the developing embryo), amnion (innermost layer of developing embryo), embryo (early stages of fetal growth, from conception to the week 8 of pregnancy), and umbilical cord (flexible cord comprised of 2 arteries and 1 vein that arises from the umbilicus and connects the fetus with the placenta). On day 20 or 21 of the cycle, the 1 mm blastocyst starts to implant the decidualized or gravid (pregnant) uterine endometrium. By the day 28 the blastocyst becomes completely imbedded into uterine myometrial tissue and implantation is complete.
First Trimester
Using a 28-day menstrual cycle, most radiologists and obstetricians define the first trimester as the 12 weeks beginning with the first day of the last normal menstrual period. Further, they describe the time span in terms of gestational age (GA) or menstrual age (MA), which are used interchangeably.
Anatomy and Sonographic Appearance During Early First Trimester
Gestational Sac
• The blastocyst is too small to be visualized sonographically, but other intrauterine changes can be detected to confirm a pregnancy during the early first trimester. The following transvaginal image shows an early pregnancy. It is described by sonologists as the gestational sac, a term used to represent the small, round or oval, fluid-filled, anechoic chorionic cavity completely enclosed by bright, echogenic walls that represent developing chorionic villi (fetal portions of the placenta that are fingerlike projections of the trophoblast layer that extend into the endometrium) and the adjacent endometrium.
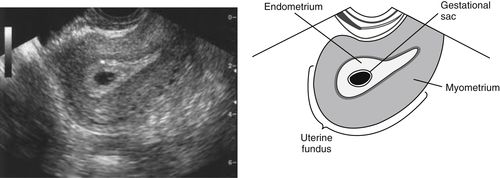
• The first key sonographic finding in an early intrauterine pregnancy is referred to as the “intradecidual sign,” which is the location of the early gestational sac right next to the centrally located endometrial cavity at the level of the fundus or body of the uterus. Transvaginal sonography is usually the best choice for visualizing the intradecidual sign, as illustrated below. Note that there should be no displacement or change in size of the endometrial cavity at this early stage.
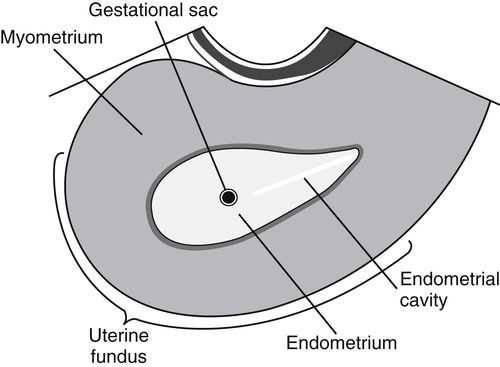
• Although transabdominal transducers are not generally the choice for resolving the intradecidual sign, they can visualize the intrauterine gestational sac as early as 3 to 5 weeks GA when sac diameter is 2 to 4 mm or serum human chorionic gonadotropin (hCG) (hormone secreted by developing placenta to communicate to the rest of the body that a gestation is present within the uterus) levels exceed 1025 mIU/mL. As the gestational sac enlarges, the walls get thicker and markedly hyperechoic relative to the imbedded myometrium.
Determining Gestational Age During the First Half of the First Trimester
Mean Sac Diameter
In the first half of the first trimester, gestational sac size is used to date a pregnancy. The method most institutions use to calculate the gestational/menstrual age is the mean sac diameter (MSD) method. As seen in the next image, caliper placement is illustrated between calipers 1 and 2. The three orthogonal dimensions of the chorionic cavity are added together and divided by 3. Alternatively, the length and anteroposterior dimensions can be measured on a long axis section of the gestational sac and width of the sac can be measured on the widest axial section. Notice how the bright rim of choriodecidual reaction is not included in the measurement. GA (in weeks) is determined by adding 3 to the MSD (in mm).
Length+Depth+Width=Total/3=MSD+3=GA(inweeks)
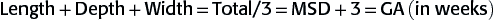
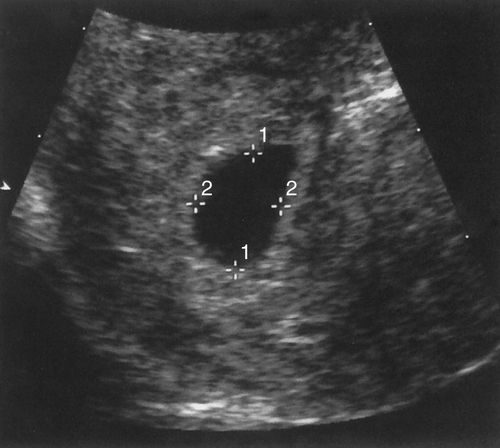
Sonographic Appearance and Development During the First Half of the First Trimester
Double Sac Sign
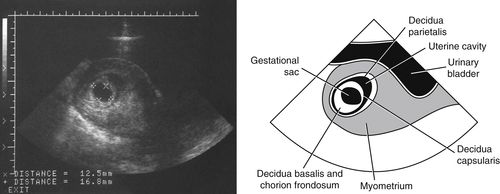
• This next transabdominal, sagittal scanning plane image shows that with further growth the gestational sac takes on the distinctive sonographic appearance known as the “double sac sign.” The 2 bright concentric lines separated by anechoic fluid in the uterine cavity are the decidua capsularis and decidua parietalis (layers of the gravid endometrium). Identification of the double sac sign is confirmation of the presence of an intrauterine pregnancy before a yolk sac is visualized and it rules out a pseudosac associated with ectopic pregnancies (pregnancies that occur outside the uterus, more often than not in a uterine tube).
Yolk Sac
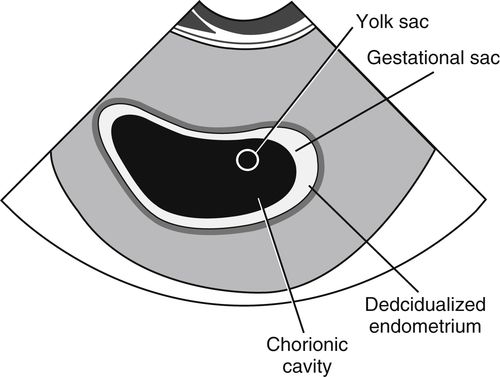
• By the end of 4 weeks GA, the primary yolk sac has regressed and is replaced by the secondary yolk sac, which is the first anatomic structure visualized within the gestational sac. The secondary yolk sac provides nutrients to the developing embryo and is the initial site of blood cell development. As illustrated below, the sonographic appearance of the yolk sac is small and round with bright, well-defined walls and an anechoic, fluid-filled center. Identification of the yolk sac is variable; however, it can be detected as early as 5 weeks GA with transvaginal transducers and should be visible by 7 weeks GA using a transabdominal approach. A faint flickering motion seen adjacent to the yolk sac represents the neurologically active heart tissue. From 5 to 10 weeks GA the yolk sac progressively increases to a maximum diameter of 5 to 6 mm. By the end of the first trimester, the yolk sac shrinks and is no longer appreciated sonographically.
Double Bleb Sign
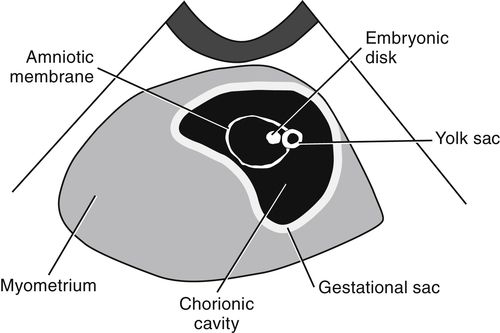
• When a subtle area is visualized on the periphery of the yolk sac, the embryonic disk has distinguished itself from the embryoblast layer. The embryonic disk lies between the yolk sac and developing amniotic membrane. On occasion, these three structures are visualized together. During the later portion of 5 weeks GA, their sonographic appearance, as illustrated below, has been described as a “double bleb” or “double bleb sign” because the embryonic disk is seen lying between the thick yolk sac and thin amniotic membrane. With developmental changes, the double bleb is not detectable after 7 weeks GA.
Determining Gestational Age During the Second Half of the First Trimester
Crown Rump Length
• Embryonic development is rapid during 6 to 10 weeks GA. As development continues into the second half of the first trimester, the MSD is replaced by the crown rump length (CRL) measurement that is thought to be the most accurate assessment of GA during pregnancy. At 6 weeks + days GA it is not possible to distinguish the crown and rump thus the embryonic disk length is taken for the CRL measurement.
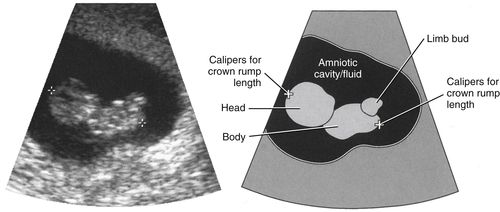
Between 6+ weeks and 8 weeks GA, the embryo’s head becomes prominently flexed making the longest axis for measurement from the neck to the rump. As seen in the image and illustration on the facing page, from 8+ weeks to 12 weeks GA the embryo’s head extends, making a true crown rump long axis for measurement.
Sonographic Appearance and Development During the Second Half of the First Trimester
Amniotic Sac
• By 6.5 weeks the amniotic membrane and its fluid filled sac or cavity have enlarged enough to surround the embryo. The thin, reflective amniotic membrane encloses the developing echogenic embryo and “bathes” it in the anechoic amniotic fluid within the amniotic sac. As the trimester progresses, not only do the CRL and amniotic sac diameter increase 1 mm per day, but their measurements are equal. Between 12 weeks and 16 weeks GA, the chorionic cavity will be obliterated when the amniotic cavity has enlarged enough for the fusion of the amniotic and chorionic membranes. At this time, it may or may not be possible to distinguish an actual embryo crown (or cephalic pole) from a rump (or caudal pole) but the yolk sac should be seen lying outside the amniotic cavity. The yolk sac and embryo retreat from each other but remain connected by the yolk stalk or vitelline duct that eventually becomes part of the umbilical cord, the 3-vessel connection between the embryo/fetus and mother. Also seen during this time is the tail-like appendage that is often identified at the site of the rump.
Embryonic Heart
• As previously mentioned, the embryonic heart may be detected as early as 5 weeks GA as a flickering motion. As the first trimester progresses the embryonic heart will appear small and pulsatile. The anechoic chambers, echogenic walls, and contour may be discernable by GA weeks 11 or 12.
Skeletal System
• The axial and appendicular skeletons form between the sixth and eighth gestational weeks. The bright reflection of the fetal skeleton indicates the degree of mineralization that has taken place within the developing bones. Ultrasound is able to distinguish how ossified portions of the fetal skeleton appear highly echogenic compared with the midgray appearance of adjacent cartilaginous structures.
Umbilical Cord
• During GA week 8 the embryo assumes a “C” shape, fetal limb buds start to be visible, placental development begins, and the umbilical cord can be visualized. The cord will appear thick and about as long as the embryo. In short axis it presents as 1 large, round, anechoic vein with bright walls, flanked by 2 small, round anechoic arteries with bright, walls. A gelatinous tissue, Wharton’s jelly, surrounds the 3 vessels within the cord and prevents it from becoming crushed. The umbilical cord will continue to grow at a rate similar to the embryo.
Tenth Week
The following image demonstrates that by GA week 10 (30 mm CRL, between measurement calipers), limbs are detectable, and normal gut herniation into the base of the umbilical cord is evident. Normal gut herniation should not be seen after GA week 12.
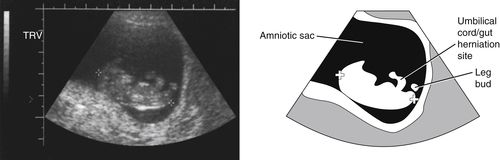
End of the First Trimester
• During GA weeks 11 and 12, individual fingers and toes can be identified as well as anechoic fluid in the stomach and urinary bladder, and the midgray, homogeneous liver. By the end of the first trimester, the oral cavity including hard and soft palates and the tongue are consistently identified. The mid- and distal portions of the esophagus may occasionally be seen as 5 parallel lines anterior to the thoracic aorta. The distal esophagus is nearly impossible to see. The embryonic head and body become proportional and the embryo has developed into a fetus that assumes a distinct humanlike appearance.
Second and Third Trimesters
Using a 28-day menstrual cycle, most radiologists and obstetricians define the second and third trimesters as GA weeks 13 to 42.
Sonographic Appearance and Development During the Second and Third Trimesters
By GA week 13, the majority of organs formed during the first trimester are located in their final anatomic positions. During the second and third trimesters, these organs and their associated organ systems become fully developed as other body structures continue to grow and mature. To grow properly and develop normally, the fetus depends on the placenta and umbilical cord for nutrients, oxygen, and removal of metabolic waste products.
Placenta
• The early placenta appears medium gray with homogeneous echo texture. It darkens slightly during the second and third trimesters and as the gestation advances, the homogeneous appearance of the placenta may be interrupted by bright, echogenic calcium deposits and/or small anechoic lacunae (maternal venous lakes) and/or retroplacental and intraplacental arteries that appear anechoic with bright walls. Anechoic tubular structures on the uterine surface of the placenta representing maternal marginal veins may also be visualized.
Placental Grading
• Many institutions utilize placental grading, a system that classifies placenta maturation according to its sonographic appearance (see Figure 13-1). Basically a grade 0 placenta appears normal throughout pregnancy. The chorionic plate (sac border) remains smooth; the basal layer (uterine border) is free of calcification, and the parenchyma or bulk of the placenta remains medium gray and homogeneous except for anechoic lacunae. With grade I, the chorionic plate shows some subtle indentations, the basal layer becomes hypoechoic or anechoic relative to adjacent structures, and the parenchyma exhibits a few scattered, bright punctate densities (calcifications). These findings are considered normal any time after 34 weeks of development. A grade II placenta presents with medium-sized indentations of the chorionic plate, a few small, linear, bright densities are identified at the basal layer, and the parenchyma contains bright, scattered, “commalike” densities. These findings are considered normal any time after 36 weeks of development. With grade III, the chorionic plate shows indentations extending as far as the basal layer, dividing the placenta into segments. The basal layer exhibits very long, linear, bright, densities that may, in advanced stages appear as a bright, unbroken line. The placental parenchyma may contain highly echogenic and anechoic areas. The bright echoes represent large calcifications that may cast acoustic shadows. These findings are considered normal any time after 38 weeks of development.
Placenta Previa
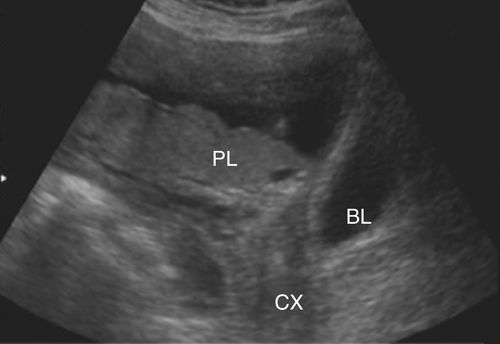
The location of the placenta is variable within the uterus and may change as the uterus expands to accommodate the growing fetus. Sonographic evaluation of the placenta includes its position relative to the cervical internal os to rule out placenta previa, a condition where the os is obstructed by overlying placenta. Depending on the degree of blockage, it is described as marginal, partial, or complete previa. When there is partial or complete placenta previa the patient may require a cesarean delivery rather than a vaginal delivery that would be dangerous for the fetus and mother. A placenta previa can be ruled out if the placental edge is 2 cm from the internal os. The following image shows an example of partial placenta previa (PL, Placenta; CX, cervix; BL, bladder).
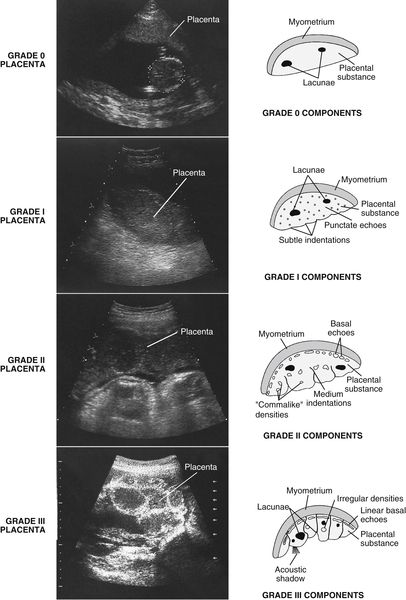
Classifications of the “aging” placenta. Notice the increase in calcifications (bright-appearing densities) and changes in contour from grades 0 to III. Grade 0: Represents the normal placenta. The placental substance appears homogeneous with medium- to low-level echoes that may be interrupted by anechoic lacunae. Grade I: The chorionic plate begins to show some signs of subtle indentations, a few scattered densities are present, and the basal layer appears anechoic. Grade II: Medium-sized indentations are evident in the chorionic plate, “commalike” densities are prevalent throughout the placental substance, and a few small linear densities appear in the basal plate. Grade III: The chorionic plate contains indentations extending to the basal layer, dividing the placenta into segments. The placental substance appears complex, with both anechoic areas and bright focal areas representing large calcifications that may cast shadows. Long, linear densities are evident in the basal plate. In advanced stages they may appear as an unbroken line.
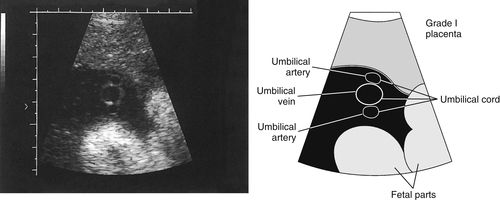
Umbilical Cord
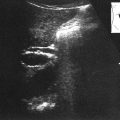
• The umbilical cord is the vascular connection between the fetus and the placenta where fetal circulation begins. The normal umbilical cord is composed of a single vein flanked by 2 arteries. The vessel lumens appear anechoic; the surrounding walls appear bright. The umbilical cord develops multiple spiral turns as it increases in length; therefore, the 3 vessels are usually easier to distinguish in short axis sections as seen in these images
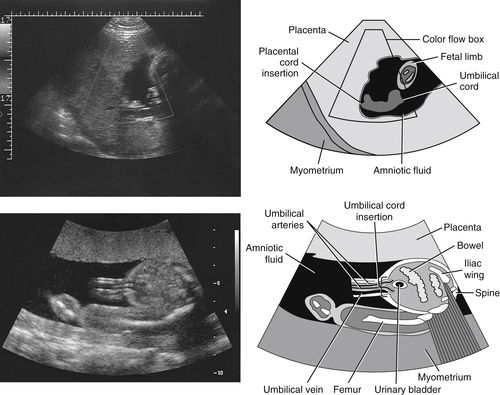
Umbilical Cord Insertion
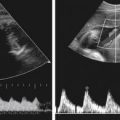
• The next 2 images show the umbilical cord insertion into the placenta and into the fetus. After the first trimester, the fetal surface vessels are routinely visualized. As demonstrated in the top image, they can be traced to the site where the vessels merge and penetrate the placental parenchyma. The bottom image shows that the umbilical cord can be identified where it enters or inserts into the fetus at the umbilicus. The umbilical vein runs cephalically to join fetal portal circulation. The arteries take a caudal course, running on each side of the urinary bladder to meet the iliac arteries.
Sonographic Appearance of Fetal Anatomy
• Midgray structures: Organ parenchyma and muscles fall into a wide range of midgray shades that provide delineation between the different structures.
• Reflective structures: Bone (ossified), choroid plexus, and the meninges appear highly echogenic with varying degrees of intensity.
• Anechoic structures: Echo-free, fluid-filled anatomy that includes the urinary bladder, stomach, gallbladder, blood vessels, brain ventricles, and heart chambers.
Skeletal System
Axial Skeleton
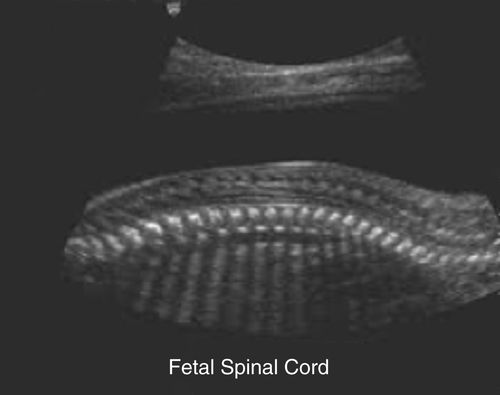
• During the second and third trimesters most of the bones of the axial skeleton are routinely visualized. The calvaria of the skull appear highly echogenic and prominent. The contour of the normal fetal head should appear smooth and elliptical in shape. Other identifiable bones include the rib cage in the thorax, mandible, nasal ridge, orbits, and fetal spine. The vertebrae have a highly reflective appearance, making them easy to recognize. The image below shows a longitudinal section of the fetal spine that can be described as 2 rows of closely spaced reflectors on each side of the medium- to low-gray appearance of the spinal cord. The 2 rows are roughly parallel, but wider in the cervical and lumbar regions and narrower in the sacral region. The gaps between the vertebral bodies are composed of nonossified margins of adjoining vertebral bodies and the intervertebral disks. In short axis sections, the vertebral anterior ossification center is seen equidistant from the 2 posterior ossification centers.
Appendicular Skeleton
• During the early to midpart of the second trimester most of the bones of the appendicular skeleton are routinely visualized. This
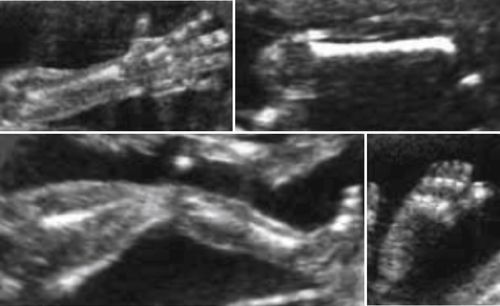
includes upper and lower extremities as demonstrated in the previous image. In short axis sections, they appear as bright echogenic foci surrounded by low-gray, homogeneous soft tissue. The longitudinal sections of the bones appear linear, bright, and reflective. The femurs especially, cast a very prominent shadow. The cartilaginous ends of the bones appear homogeneous and low-gray.
Cardiovascular System
Heart
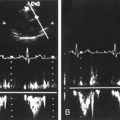
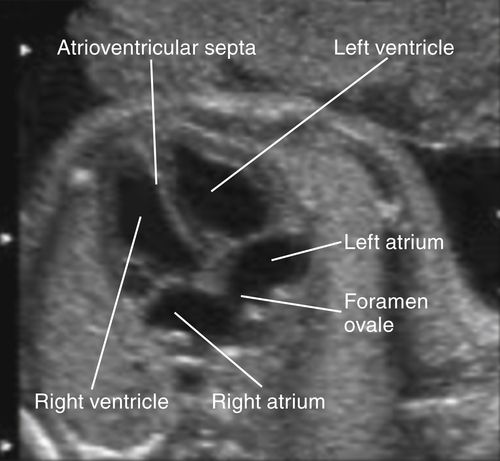
• By 15 weeks GA the 4 chambers of the fetal heart can be visualized. The walls of the heart appear midgray and hyperechoic relative to the anechoic blood in the chambers. The 4 chambers should appear relatively symmetric as demonstrated in the image below. They are divided by the echogenic atrioventricular septa, which will appear “broken” at the foramen ovale (a normal opening between the atria allowing blood to move right to left in the fetal heart). The heart is normally visualized on the left side of the thorax.
Blood Vessels
• Blood vessels in the fetus appear as they do after birth, bright walls and anechoic blood in the lumens. The superior vena cava, thoracic aorta, and pulmonary artery can be visualized in the upper mediastinum during the second trimester. With advanced GA, the brachiocephalic artery, common carotids, left subclavian, and the jugular veins are frequently visualized. The abdominal aorta and inferior vena cava are easy to identify in the posterior portion of the abdomen. The iliac arteries and veins are also often observed. Color Doppler sonography is helpful for resolving small vessel branches such as the celiac axis, superior mesenteric artery, renal arteries, and renal veins.
Respiratory System
Upper Respiratory Tract
• Sonography is able to visualize upper respiratory tract structures such as the nose, nasal cavity and septum, and the palate. The pharynx, hypopharynx, piriform sinuses, and the epiglottis (with advanced fetal age) are easily identified due to anechoic amniotic fluid in portions of the upper tract. The fluid filled trachea can usually be traced from its distal end to the level of the aortic arch. When the hypopharynx contains amniotic fluid the larynx can be identified.
Lungs
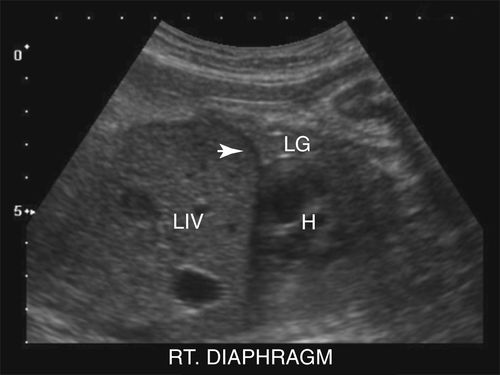
• During the first trimester, the lungs are identified more by the structures adjacent to them such as the heart, ribs, diaphragm, and liver. The image below demonstrates that during the second trimester, however, the lungs (LG rt lung) become more apparent and appear isosonic/isoechoic to the midgray, homogeneous appearance of the fetal liver (LIV). The muscular diaphragm (arrow) separates the thorax from the abdomen and appears hypoechoic relative to the liver and lungs. As GA advances, the lungs become more echogenic.
Gastrointestinal System
Stomach and Gallbladder
• The fetal stomach and gallbladder are readily identified sonographically as they are the only subdiaphragmatic gastrointestinal system structures normally filled with fluid. As seen in the next image, the fluid-filled stomach appears anechoic and is easy to identify on the left side of the fetal abdomen. Size of the stomach varies depending on the amount of amniotic fluid swallowed by the fetus. The bile-filled gallbladder appears anechoic and on the right side of the fetal abdomen. The gallbladder may not be visualized after 32 weeks GA. Some experts believe that the gallbladder contracts, releasing bile, due to initiation of gallbladder function.
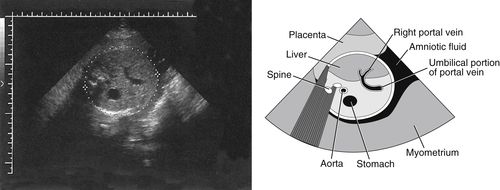
Liver
• The liver is the largest parenchymal organ of the gastrointestinal system and of the body. It is routinely visualized during the second trimester. It appears midgray and homogeneous and fully occupies the right side and much of the rest of the fetal abdomen. The anechoic umbilical vein is routinely identified coursing through a portion of liver parenchyma to reach its point of bifurcation.
Pancreas
• The pancreas is another major parenchymal organ of the gastrointestinal system; it is rarely seen. It may be visualized between the anechoic fluid-filled stomach (posterior wall) and anechoic splenic vein. It appears hyperechoic relative to the fetal liver.
Spleen
• The spleen is not a gastrointestinal organ but is included as part of this discussion because it is associated with the liver by virtue of portal-splenic circulation. Like the fetal liver, the spleen is routinely identified from the second trimester onward. The spleen occupies the left upper quadrant of the fetal abdomen and appears isosonic to the fetal liver.
Small and Large Bowel
• Small bowel loops and large bowel loops can be well distinguished sonographically in the second and third trimesters. The muscle layers of the bowel appear hypoechoic relative to the highly echogenic appearance of the serosa and subserosal linings. By the end of the third trimester it is normal to visualize a small amount of anechoic fluid and bright areas of meconium (fetal waste) within the small bowel.
Genitourinary System
Kidneys
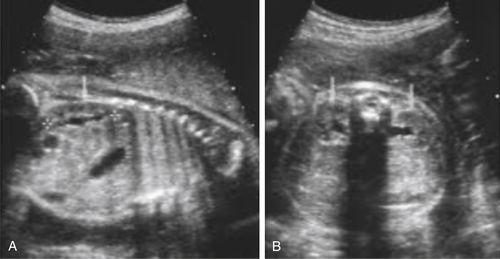
• The fetal kidneys have been identified sonographically as early as 15 weeks GA. At this stage of renal development the sonographic appearance of the kidneys can be difficult to differentiate from adjacent structures. However, after 20 weeks GA, the highly echogenic retroperitoneal fat comes to surround the kidneys, making them easier to identify. Normal fetal renal cortex appears mid- to low-gray or slightly hypoechoic relative to adjacent structures. Unlike adult kidneys, there is very little fat in the fetal renal sinus making it virtually indistinguishable from the cortex. This leads to visualization of urine-filled intrarenal structures (renal pelvis and infundibula) that are not normally appreciated sonographically in adult kidneys. With advanced GA, the renal sinus can become slightly hyperechoic relative to the cortex making the kidneys easier to sonographically distinguish. The distinctive elliptical shape and bright renal capsule assist sonographic identification of the longitudinal sections of the fetal kidneys as seen in image A (arrow and between calipers). Image B shows that the short axis or axial sections of the fetal kidneys can be identified in their normal paraspinal location (arrows).
Adrenal Glands
• The fetal adrenal glands are not part of the genitourinary system yet their close proximity to the kidneys makes them a significant sonographic marker. The adrenals appear to cap the upper renal poles. The triangular shaped adrenals present sonographically as low-gray organs that are hypoechoic relative to the liver and renal cortex on the right and the spleen and renal cortex on the left.
Ureters
• Normally, fetal ureters are not visualized sonographically.
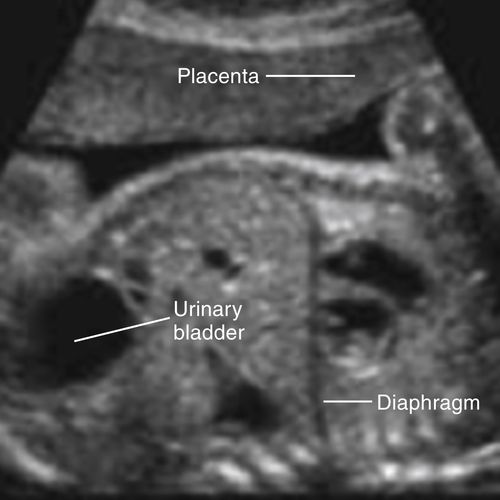
Urinary Bladder
• The urine-filled fetal bladder is easily recognized in the fetal pelvis because of its characteristic anechoic appearance and midline position. Another distinction is the thin, bright bladder wall that virtually disappears when the bladder is fully distended. Changes in the volume of the urinary bladder not only confirm normal fetal renal function but also, with time, differentiate the bladder from pathologic structures in the fetal pelvis, such as true cysts that have the same sonographic appearance.
Urethra
• On occasion, the urethra is identified in male fetuses. If the penis is erect, the urethra appears as a bright, reflective line running along the length; otherwise it cannot be identified.
Genitalia
• Fetal gender can be established from the early second trimester by identifying either the male scrotum or the female labia. The penis and scrotum appear homogeneous and mid to low gray. It is not uncommon to identify the testes within the scrotum in the early to mid third trimester. Occasionally, small, bilateral, anechoic testicular hydroceles (fluid collection) will be visualized. The labia have 2 parts that are sonographically distinguishable, the major labia and minor labia. The major labia flank the minor. Both appear homogeneous and midgray but the major labia is hyperechoic relative to the minor. The vaginal cleft lies at the midline between the minor labia; it appears linear and bright. The labia can be identified sonographically as early as 17 or 18 weeks GA.
Intracranial Anatomy
Lateral Ventricles
• By 11 weeks GA, the most prominent intracranial structures visualized are the highly echogenic choroid plexus, easily identified within the body of the lateral ventricles. There is a striking contrast between the appearance of the bright choroid plexus and the anechoic appearance of the ventricular chambers filled with cerebrospinal fluid. The walls of the ventricles appear vivid and bright. At this stage, only the ventricular bodies and frontal horns are developed well enough to visualize; the occipital and temporal horns are still rudiments. The outer walls of the lateral ventricles appear as bright linear structures lying the same distance from the interhemispheric fissure. The medial walls of the lateral ventricles are not quite as vivid in appearance as the outer ventricular walls. The appearance of the lateral ventricles changes as development continues. The occipital and temporal horns become visible by 18 to 20 weeks GA and as brain tissue volume increases with normal development, ventricular shape is altered and overall ventricular size decreases. The atria are the sites where the temporal and occipital horns join the body of the lateral ventricles. Ventricular width is normal up to 10 mm. Cerebrospinal fluid flows from the lateral ventricles to the third and fourth ventricles; into the subarachnoid space; then to the dural sinuses where it is absorbed into the venous bloodstream.
Third Ventricle
• The third ventricle lies at the midline of the brain and appears as a highly reflective line parallel to the interhemispheric fissure. Occasionally the third ventricle’s cavity fills with cerebrospinal fluid giving it the appearance of an anechoic, midline slit.
Fourth Ventricle
• The fourth ventricle also lies at the midline of the brain, posterior to the third ventricle.
Interhemispheric Fissure and Falx
• The interhemispheric fissure visually separates the cerebral hemispheres. The fissure appears as a single, linear, bright structure at the midline of the brain. The falx cerebri, a fold of dura mater, lies within the interhemispheric fissure, and because they are not sonographically distinguishable from one another, the terms are used interchangeably.
Cerebrum
• The cerebrum is the largest component of the brain. It is almost completely divided anteroposteriorly into two lateral, symmetrical hemispheres by the callosal fissure. It is composed of 5 lobes: parietal, temporal, occipital, frontal, and insula (or isle of Reil), the only lobe not named for an overlying bone. The normal cerebrum appears homogeneous and mid- to low-gray.
Cerebellum
• The cerebellum sits below the cerebrum and superoposterior to most of the brain stem. Like the cerebrum, it is composed of 2 lateral, symmetrical hemispheres. The vermis, a small central lobe relays information between the 2 hemispheres. The normal cerebellum appears mid- to low-gray with low-level echoes that tend to be hypoechoic relative to the cerebrum. In the posterior portion of the brain, the small, round, cerebellar hemispheres are seen on either side of the homogeneous, midgray vermis, which is located at the midline of the brain.
Tentorium Cerebelli
• The tent-shaped tentorium cerebelli separates the cerebellum from the more superior structures.
Brain Stem
• The medulla, pons, midbrain, thalamus, and hypothalamus compose the brain stem, which forms the base of the brain that is continuous with the spinal cord. The components of the brain stem present sonographically as midgray homogeneous structures that vary in their echo level intensity depending on the stage of development. The spinal cord is detectable by 15 or 16 weeks GA. Spinal cord neural tissue appears low-gray with low-level echoes. It is easily identified lying between the highly reflective, bony vertebrae.
Thalamus
• The thalamus can be identified in the center of an axial section of the temporal lobe of the brain. It is composed of 2 ovoid-shaped halves that are primarily composed of brain gray matter. Each half lies on either side of and forms a portion of the lateral walls of the third ventricle. Thalami appear midgray with medium-level echoes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree