Part 10 Fluorine-18 Fluorodeoxyglucose Positron-Emission Tomography
Case 114

Clinical History
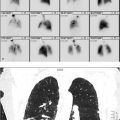
47-year-old female with marginal zone lymphoma of the left parotid gland (▶Fig. 114.1).
Key Finding
Focal fluorine-18 fluorodeoxyglucose (F-18 FDG) uptake in the parotid gland
Top 2 Differential Diagnoses
Primary parotid neoplasm. Physiologic activity on F-18 FDG positron emission tomography/computed tomography (PET/CT) can complicate interpretation of the head and neck. Physiologic uptake is commonly seen within the brain, extraocular muscles, soft and hard palate mucosa, Waldeyer’s ring, neck, pharyngeal and laryngeal muscles, and thyroid. Uptake can also be seen in brown adipose tissue. Physiologic parotid uptake is variable, as F-18 FDG is taken up by the salivary glands and secreted in saliva, but it is typically diffuse and symmetric. Several benign entities can result in increased, asymmetric, salivary gland uptake, including sarcoidosis, infection, and radiation-induced sialadenitis. Any focal increased FDG avidity within the parotid requires scrutiny of the associated anatomic imaging, and often further evaluation with magnetic resonance imaging (MRI) and/or biopsy. Several benign and malignant primary parotid neoplasms can show focal increased FDG avidity, including Warthin’s tumor, pleomorphic adenoma, primary parotid lymphoma, mucoepidermoid, salivary duct, and adenoid cystic carcinomas. High-grade malignant parotid lesions tend to have higher uptake, but no statistically significant standardized uptake value (SUV) cutoff has been defined to differentiate. Some low-grade lesions, such as adenoid cystic carcinomas and low-grade mucoepidermoid carcinomas, may result in false-negative F-18 FDG PET/CT.
Metastatic disease. Focal F-18 FDG uptake in the parotid gland may represent either a parotid parenchymal or intraparotid lymph node metastasis. While head and neck squamous cell carcinomas and melanoma are the most likely malignancies to metastasize to the parotid gland, parotid metastases have been also seen with lung, breast, renal, prostate, and gastrointestinal malignancies.
Diagnosis
Marginal zone lymphoma of the parotid gland.
✓ Pearls
Focal parotid gland uptake on F-18 FDG PET/CT can be seen with benign and malignant lesions.
High-grade primary parotid neoplasms typically show higher uptake values, but uptake is not diagnostic.
Parotid mets can be from multiple malignancies, most commonly head and neck cancers and melanoma.
Further evaluation of focal parotid uptake on PET is usually with MRI.
Suggested Readings
Nakamoto Y, Tatsumi M, Hammoud D, Cohade C, Osman MM, Wahl RL. Normal FDG distribution patterns in the head and neck: PET/CT evaluation. Radiology. 2005; 234(3):879–885 Purohit BS, Ailianou A, Dulguerov N, Becker CD, Ratib O, Becker M. FDG-PET/CT pitfalls in oncological head and neck imaging. Insights Imaging. 2014; 5(5):585–602 Roh JL, Ryu CH, Choi SH, et al. Clinical utility of 18F-FDG PET for patients with salivary gland malignancies. J Nucl Med. 2007; 48(2):240–246Case 115

Clinical History
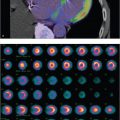
46-year-old male with history of chronic lymphocytic leukemia (CLL) status post allogeneic hematopoietic stem cell transplant with new bilateral cervical lymphadenopathy (▶Fig. 115.1).
Key Finding
F-18 FDG uptake in the thyroid
Top 3 Differential Diagnoses
Thyroiditis. F-18 FDG is a radiolabeled glucose analogue that competes with glucose for intracellular transport via the GLUT 1 and 3 transporters. F-18 is cyclotron produced, has a physical half-life of 110 minutes, and undergoes positron emission resulting in two directly opposed 511-KeV gamma photons after an annihilation reaction. FDG is phosphorylated by hexokinase but does not undergo glycolysis. As the thyroid is not unique in its affinity for glucose, FDG is not an ideal radiotracer for dedicated thyroid imaging. However, thyroid uptake on FDG studies employed for other reasons is common. Diffusely increased uptake within the thyroid gland is nonspecific, but is most often seen in the setting of thyroiditis (approximately 80% of cases), including both Hashimoto’s and subacute forms. Reactive lymphocytes and inflammatory cells uptake the FDG, with increased uptake present early in the disease which may be diffuse or patchy. The gland itself is usually normal in size. As the disease progresses, the thyroid gland becomes “burned out,” and will demonstrate decreased or absent uptake.
Normal thyroid. The thyroid gland normally has mild to moderate symmetric FDG uptake. One study reported that the average standardized uptake value (SUV) in the thyroid is 1.39 ± 0.31 for men, and 1.23 ± 0.27 for women. Alternatively, decreased or near absent FDG uptake within the thyroid could be a normal finding, but may also be seen in the setting of ectopic thyroid, after radioactive iodine ablation or post thyroidectomy. No thyroid uptake in a woman should prompt evaluation of the pelvis to exclude struma ovarii. Correlating the functional PET images with the anatomic CT images, in conjunction with lab analysis, should help narrow the differential.
Malignancy. Interestingly, thyroid cancers often demonstrate an inverse relationship between radioiodine and FDG uptake; higher-grade/less well-differentiated tumors tend to have increased FDG and decreased radioiodine avidity. This is the reason F-18 FDG PET/CT is used for a thyroid cancer patient with new elevated thyroglobulin levels on follow up and a negative whole-body radioiodine scan. Focal FDG uptake within thyroid is malignant in about one out of five cases, and should be considered malignant until proven otherwise. Malignant nodules usually demonstrate uptake twice the background level. Ultrasound and biopsy are recommended in most cases. Thyroid lymphoma, alternatively, will show diffuse increased FDG uptake, usually significantly higher than seen with thyroiditis.
Additional Diagnostic Considerations
Grave’s disease: In this disease, the autonomously hyperfunctioning thyroid gland is responsible for the increased FDG uptake, as opposed to reactive lymphocytes and inflammatory cells in thyroiditis. The gland is generally enlarged and FDG avid throughout the disease course.
Multinodular goiter: A multinodular goiter may demonstrate a variety of uptake patterns, from focal to patchy to symmetrically increased uptake, depending on the activity level of the individual nodules. Anatomic imaging is likely to demonstrate an enlarged, heterogeneous thyroid gland in this setting.
Diagnosis
Papillary thyroid carcinoma.
✓ Pearls
A diffusely hyperactive thyroid gland on FDG PET/CT is more often thyroiditis than lymphoma.
Focal FDG uptake within the thyroid should be considered malignant until proven otherwise.
Thyroid cancers are often FDG avid but not iodine avid; well-differentiated tumors may be negative on FDG PET.
Suggested Readings
Barrio M, Czernin J, Yeh MW, et al. The incidence of thyroid cancer in focal hypermetabolic thyroid lesions: an 18F-FDG PET/CT study in more than 6000 patients. Nucl Med Commun. 2016; 37(12):1290–1296 Blodgett TM, Fukui MB, Snyderman CH, et al. Combined PET-CT in the head and neck: part 1. Physiologic, altered physiologic, and artifactual FDG uptake. Radiographics. 2005; 25(4):897–912 Nakamoto Y, Tatsumi M, Hammoud D, Cohade C, Osman MM, Wahl RL. Normal FDG distribution patterns in the head and neck: PET/CT evaluation. Radiology. 2005; 234(3):879–885Case 116

Key Finding
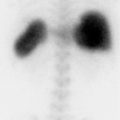
Solitary hypermetabolic pulmonary lesion on PET scan
Top 3 Differential Diagnoses
Malignancy. Standard PET imaging is performed from the skull base to proximal thighs 45 to 90 minutes after injection of around 10 to 15 mCi of F-18 FDG. Corresponding low-dose CT is performed for attenuation correction and anatomic localization. Malignant cells have increased metabolic activity and generally have upregulated glucose transporters along with downregulated glucose-6-phosphatase. Positron emission tomography/computed tomography (PET/CT) is indicated for detection and staging of malignancies, including posttherapy response. PET/CT has sensitivity of about 95% and specificity of about 80% for determining whether a solitary pulmonary nodule greater than 1 cm in size is benign or malignant. Negative findings on PET are less helpful in the setting of high pretest likelihood of malignancy. Standardized uptake value (SUV) is a semiquantitative index for tumor metabolism and a maximum SUV (SUVmax) of 2.5 is generally regarded as a cutoff for malignancy. However, any uptake within a pulmonary nodule is suspicious. False negatives may occur due to the partial volume effect in subcentimeter nodules and low-grade or well-differentiated malignancies.
Active granulomatous disease. FDG uptake is nonspecific and can be seen within active nonneoplastic processes, including granulomatous diseases such as sarcoidosis, fungal infection, and tuberculosis. Increased glycolysis within activated macrophages is likely responsible for FDG uptake. SUV may be high (>2.5) within these benign lesions. A biopsy or close follow-up may be the next appropriate step for definitive diagnosis. Dual-time point imaging in some instances may improve accuracy since nonneoplastic lesions generally do not demonstrate increasing FDG accumulation on delayed scan.
Pulmonary infection/inflammation. Increased activity is also seen within sites of active infection or inflammation, likely due to inflammatory cell metabolism and mediators. Focal pulmonary infection, abscesses, radiation pneumonitis, active fibrosis, and postsurgical changes can demonstrate high FDG uptake simulating malignancy. Correlation with the patient’s history and corresponding anatomic imaging (i.e., CT scan) can aid in making appropriate diagnosis.
Diagnosis
Airway centered acute or chronic inflammation and fibrosis; no evidence of malignancy.
✓ Pearls
Patient preparation prior to PET includes 4-hour fasting, no recent regular insulin, and serum glucose < 200 mg/dL.
FDG uptake is nonspecific and is seen in the setting of neoplasm and active infection or inflammation.
An SUV ≥ 2.5 is generally considered as the cutoff for malignancy, but is not reliable in small lesions.
Bronchoalveolar carcinoma (BAC) or mucinous metastases to the lung may be falsely negative on PET scan.
Suggested Readings
Bunyaviroch T, Coleman RE. PET evaluation of lung cancer. J Nucl Med. 2006; 47(3):451–469 Choromańska A, Macura KJ. Evaluation of solitary pulmonary nodule detected during computed tomography examination. Pol J Radiol. 2012; 77(2):22–34 Truong MT, Ko JP, Rossi SE, et al. Update in the evaluation of the solitary pulmonary nodule. Radiographics. 2014; 34(6):1658–1679Case 117

Clinical History
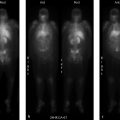
79-year-old female with right lower lobe enlarging ground glass nodule on chest CT (▶Fig. 117.1).
Key Finding
Solitary hypometabolic pulmonary lesion on PET scan
Top 3 Differential Diagnoses
Granuloma. PET/CT is a useful tool for the evaluation of solitary pulmonary nodules. The main advantage of PET/CT is the negative predictive value (NPV), meaning a lesion without uptake is unlikely to be malignant (NPV around 97%). Using PET/CT for evaluation can thus prevent some unnecessary biopsies of benign lesions. Pulmonary granulomas are frequently encountered lesions. While characteristic calcifications (central, diffuse, or laminated) are frequently seen allowing for accurate morphologic diagnosis, calcifications are not always present. An active granuloma will still have F-18 FDG uptake and may be a false positive. When present, the uptake should usually be less than a 2.5 standardized uptake value (SUV)max (and less than the mediastinal blood pool), but further evaluation would still be required to exclude malignancy.
Adenocarcinoma in situ (AIS). Formerly known as bronchoalveolar carcinoma (BAC). These well-differentiated tumors are known to be hypometabolic on F-18 FDG PET/CT. Around half of these will not demonstrate increased FDG uptake, particularly the mucinous variety.
Carcinoid. These low-grade malignancies account for a very small portion of lung neoplasms, around 1 to 2%. The majority of these occur within central bronchi. They do have the ability to invade and metastasize, but are generally slow growing with low metabolic rates.
Additional Considerations
Hamartoma: Imaging features are often characteristic, including popcorn chondroid calcifications and intranodular fat.
Small bronchogenic carcinoma: Spatial resolution for PET is around 7 to 8 mm. For this reason, small metabolically active lesions may appear photopenic secondary to volume averaging.
Metastasis: A solitary lesion makes metastatic disease less likely, although it is still possible. Metastases from some primary malignancies, such as renal cell carcinoma and mucinous neoplasms, are often hypometabolic.
Diagnosis
Invasive adenocarcinoma.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree