Case presentation
A 12-year-old male presents with a left fifth phalanx injury (his “pinky” finger). He was jumping on a trampoline and somehow injured the digit; he believes he landed on the digit. Since then, he has had pain and swelling.
His examination reveals a patient complaining of digit pain. There is swelling and tenderness of the left fifth digit at the proximal interphalangeal (PIP) joint with limited range of motion secondary to the pain. He is grossly neurovascularly intact and there is no apparent wrist, forearm, elbow, upper arm, or shoulder injury. He does state he has “hand pain” as well, proximal to his swollen finger.
Imaging considerations
Plain radiography
This is the imaging modality of choice for the evaluation of phalanx injuries. A minimum of two views (posterior-anterior and lateral) should be utilized, although an oblique view may be useful as well, as some injuries may not easily be visible in two planes; the clinician should consider obtaining an oblique view if there is a strong clinical suspicion and two-view imaging does not demonstrate a fracture.
Ultrasound (US)
There has been interest in point-of-care US (POCUS), done at the bedside by emergency physicians, for detecting fractures of the phalanges and hand. This imaging modality has proven to be sensitive and specific in the detection of phalanx fractures in adult patients. Ultrasonography has been shown to be efficacious at detecting other hand fractures such as metacarpal fractures, with reported sensitivities and specificities of 92% and 87%, respectively, in patients aged 5 to 55. , One study, done in adult patients, demonstrated a sensitivity of 79% and a specificity of 90% utilizing POCUS for proximal and middle phalanx fractures; although, in this study, smaller fractures were more difficult to detect, particularly middle phalanx volar fractures.
Large-scale studies specifically evaluating the efficacy of phalanx fracture detection in the pediatric population using US are lacking. However, the lack of ionizing radiation, availability, and apparent efficacy in the adult population at fracture detection make this modality an attractive imaging option.
Computed tomography
While computed tomography may be helpful to assess complex fracture injury extent and anatomy, this modality is not indicated for phalanx fractures. If there is an associated complex metacarpal or carpal fracture that requires better radiographic visualization, then computed tomography may be indicated to assist with the management of those fractures.
Magnetic resonance imaging (MRI)
This modality is not indicated as an initial imaging test for suspected phalanx fractures.
Imaging findings
Imaging of the left fifth finger was obtained. The images are provided. There is a Salter-Harris type II fracture of the fifth proximal phalanx. There is fracture of the proximal metaphysis of the proximal phalanx, seen as a buckling of the cortex. Although the fracture is nondisplaced, there is volar and radial angulation of the fracture apex ( Figs. 62.1–62.3 ).


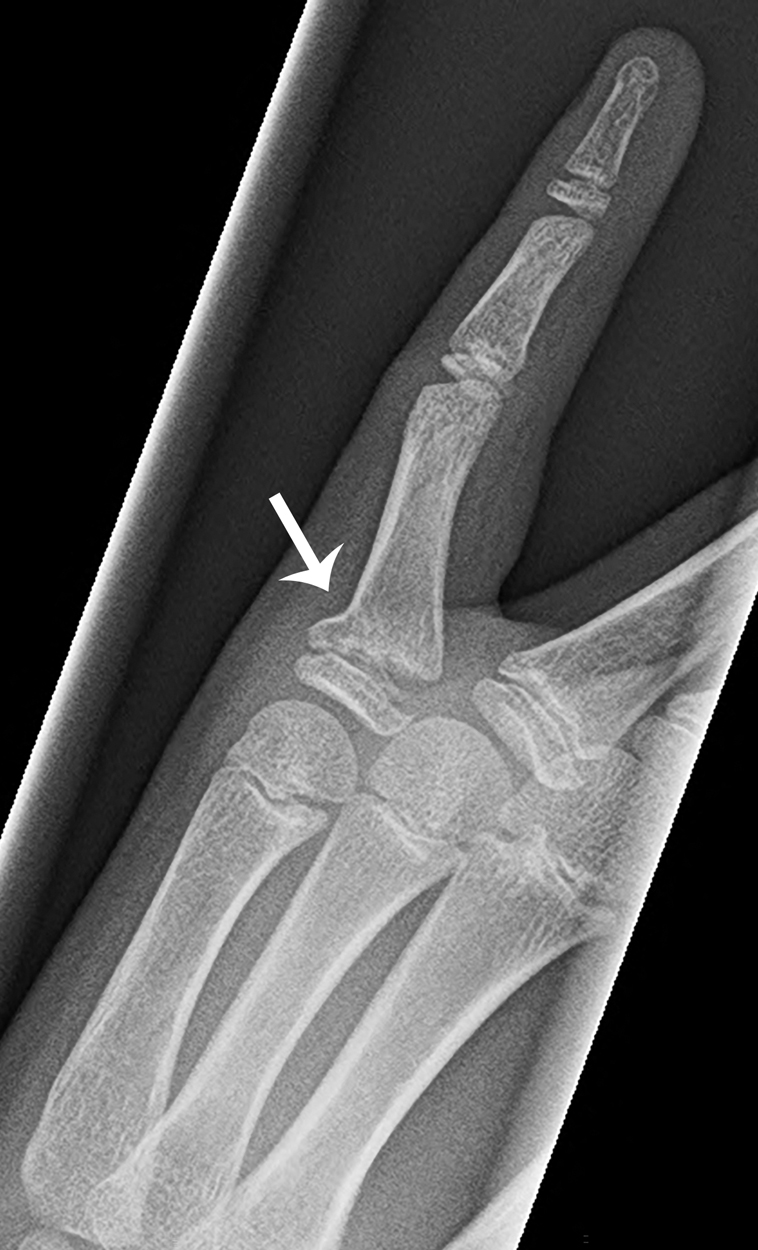
Case conclusion
The child was placed in an ulnar gutter splint and follow-up was arranged with Hand Surgery, after closed reduction. The injury did not require operative intervention.
Phalanx fractures are among the most frequent hand fractures in pediatric patients. , , With an incidence of 27 per 1000 patients, these fractures make up the second most common reason to seek fracture care in an emergency setting. , Injury patterns are associated with age; toddlers and school-age children are more likely to sustain phalanx fractures (often from crush injuries or lacerations) in a home location, whereas older children often have injuries associated with sports activities. , ,
Management of phalanx fractures depends on fracture location, displacement, and orientation. Fracture type, including the Salter-Harris classification system for fractures involving the growth plate, can aid in management. Most phalanx injuries in pediatric patients can be managed nonoperatively. Generally, lower-grade fractures, such as Salter-Harris types I and II, are managed nonoperatively with closed reduction; types III and IV may require either closed or open reduction; and type V injuries require surgical consultation. Buddy taping versus splinting has been investigated. A study comparing buddy taping and splinting for fracture management demonstrated that the risk for secondary displacement of extraarticular phalanx fractures (both those requiring closed reduction and those not requiring closed reduction) was low in both groups, with patient satisfaction and comfort higher in the buddy taping group.
Fractures of the base of the phalanx are often Salter-Harris type II fractures , , and are among the most common hand injuries in the pediatric population. Due to excellent bone remodeling, these fractures tend to heal quite well. Displaced fractures should have closed reduction attempted, while severe comminution, ligament disruption, and flexor tendon interposition at the fracture site are indications for open operative reduction and fixation. , Most phalanx fractures are immobilized for 3 weeks. Some authors recommend follow-up plain radiography 3 to 7 days after reduction to ensure that the fracture has not displaced. Proximal phalanx fractures that are displaced and have failed closed reduction should be operatively repaired with pinning, although patient age, along with fracture type and displacement, is a factor in deciding if operative repair is warranted. Pediatric patients who have undergone closed reduction and percutaneous pinning (after failing closed reduction) have been shown to have good functional and cosmetic outomes.
Fractures of the phalangeal shaft with no or minimal displacement are often treated by buddy taping for several weeks, followed by gradual return to normal range of motion and activity. , , Displaced fractures should be reduced (typically by closed reduction), followed by immobilization (often with splinting then casting). , , These fractures are usually Salter-Harris type III and typically are immobilized for 3 weeks. Referral for follow-up care to a qualified hand or orthopedic specialist is appropriate.
Fractures that involve the neck of the phalanx are managed based on the degree of displacement. Nondisplaced fractures may be splinted and followed closely, while displaced fractures, due to inherent instability, are usually managed surgically, most often with closed reduction and percutaneous pinning. , , , Interestingly, a small study comparing closed reduction and immobilization versus operative intervention in children demonstrated similar outcomes between the two groups. These injuries occur almost exclusively in the pediatric population. , In addition to being unstable, these fractures have poor remodeling potential, and if malunion occurs, overlapping of the digits during flexion can occur. Distal finger fractures are usually Salter-Harris type I or II and open fractures are not uncommon, as there are often associated nail injuries, including lacerations of the nailbed and nail avulsion. Consultation with a qualified hand specialist is appropriate for these patients for follow-up care.
Complications of phalanx fractures include cosmetic deformities and impairment of function, including growth arrest (associated with physeal injury), avascular necrosis (if blood supply is disrupted), infection, and arthofibrosis. , Some fracture types are associated with higher complication rates, including Salter-Harris type IV fractures and Seymour fractures. Phalanx fractures that have malunion may be treated with osteotomy. ,
One particular fracture worth mentioning is the Seymour fracture, first described in 1966. , This often overlooked fracture, typically a Salter-Harris type I or II, involves the distal phalanx and an associated laceration of the nail matrix with avulsion of the proximal nail plate. This most commonly is due to an axial load injury and often involves the middle finger. , , , This injury results in exposure of the cuticle seal and there is potential for infection. While radiography demonstrates a physeal injury, there may only be dorsal widening of the physis. These fractures should be thoroughly explored and oral antibiotics initiated. Consultation with a qualified hand surgeon is appropriate in these cases.
Another fracture deserving special mention is the volar plate avulsion fracture. This injury occurs when the PIP joint is hyperextended, and the volar plate ligament produces an avulsion fracture at the volar base of the middle phalanx. This fracture is usually managed initially with splinting for a short duration (7 to 10 days is sufficient), followed by early range of motion exercises. , Prolonged immobilization should be avoided, since healing occurs not by bony union but by fibrous nonunion, and prolonged casting can lead to joint contracture. ,
For comparison, several images of phalanx injuries are provided:
The 17-year-old patient in Figs. 62.4 and 62.5 was involved in a motor vehicle collision. The vehicle’s airbag deployed and caused his left fifth digit (the “pinky finger”) to hyperextend. He presented with pain to the volar side of the digit. Lateral and oblique views show a volar plate avulsion fracture of the middle phalanx of the fifth finger at the PIP joint. He was placed in a finger splint and followed up with Hand Surgery 1 week later.











