Case presentation
A 14-month-old previously healthy male presents with limping for the past 5 days. Prior to this symptom, he had cough, congestion, and subjective fever, which his primary care provider had diagnosed as a viral upper respiratory infection. He appeared to be improving when he developed a left-sided limp, which appeared at times to be painful, although over-the-counter ibuprofen seemed to help with pain.
On examination, he is afebrile and has age-appropriate vital signs. Physical examination is unremarkable other than a painful gait when he attempts to ambulate. He had no tenderness in his knee or his hip, and he had a full range of motion on examination.
Imaging considerations
Plain radiography
Plain radiography is an excellent first-line imaging modality for children with presumed skeletal pain. Ionizing radiation exposure is low and the modality is readily available. Two views of the extremity (anteroposterior and lateral) are sufficient in most cases.
A Brodie abscess will often appear as a distinct, well-demarcated intramedullary lesion. There may be surrounding sclerosis and cortical thickening; cortical destruction may be seen; and periosteal reaction is typically present. Notably, plain radiographs may be unremarkable during the initial stages of abscess development, and radiographic changes may be delayed up to 10 days.
Computed tomography (CT)
This modality is useful in defining the extent of the lesion but is less useful for defining an inflammatory process. CT is excellent at detecting cortical destruction and periosteal reaction, although is not a first-line imaging modality.
Magnetic resonance imaging (MRI)
MRI is an excellent modality to visualize and define inflammatory processes, particularly early in the course of illness. This modality has a high sensitivity in detecting the pathology of bone and soft tissue and can define the extent of a pathologic process. Availability and the possible need for sedation may limit immediate use. MRI is typically used as a follow-up study when plain radiography demonstrates a lesion. Non–contrast-enhanced and contrast-enhanced imaging is employed.
A Brodie abscess visualized with MRI appears as a well-defined lesion with a central area that is hypointense on T1-weighted images but hyperintense on T2-weighted images; the surrounding bone marrow will also enhance; associated surrounding edema is hypointense on T1-weighted images but hyperintense on T2-weighted images.
Imaging findings
Due to the painful gait and history of subjective fevers, the child had bloodwork and plain radiography of the left lower extremity performed. The peripheral white blood cell count was 11,700/mm 3 , the erythrocyte sedimentation rate was 26 mm/hour, and the C-reactive protein was 1.4 mg/dL. His gait improved after he was administered ibuprofen. The images were reported to be unremarkable (not provided here). He was discharged with a diagnosis of toxic synovitis and appropriate follow-up instructions were provided.
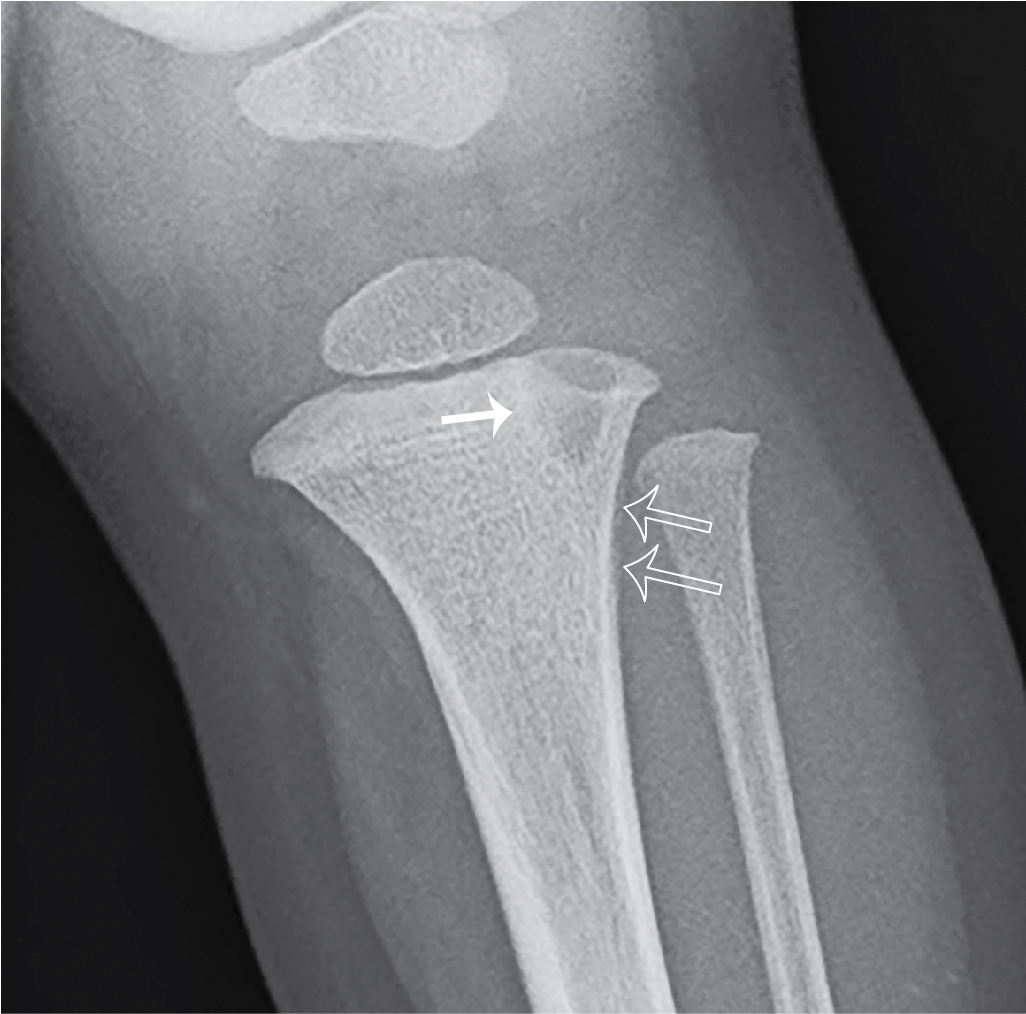
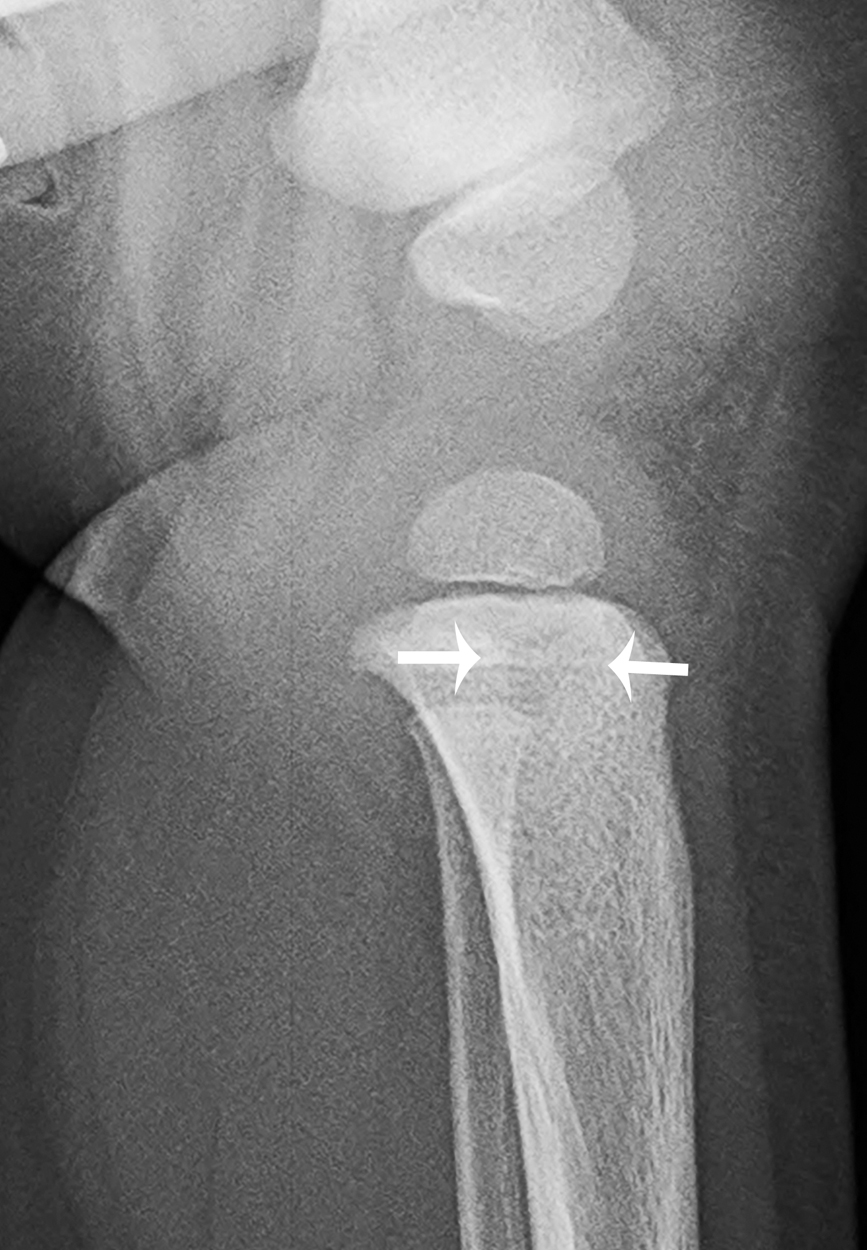
The child returned 10 days later with worsening and now persistent pain. In the interim period, he had days where the pain waxed and waned and initially was improved with ibuprofen, as before, but now there was no symptomatic improvement. Repeat bloodwork and imaging were obtained. The peripheral white blood cell count was 11,300/mm 3 , the erythrocyte sedimentation rate was 35 mm/hour, and the C-reactive protein was 0.8 mg/dL. Plain radiography demonstrates a 9-mm lytic proximal tibial metaphyseal lesion with slightly ill-defined sclerotic borders, and subtle proximal tibial periostitis ( Figs. 73.1 and 73.2 ). MRI was subsequently performed; selected images are provided here. The lesion in the proximal left tibial metaphysis is of low signal intensity on T1-weighted images and high signal intensity on T2-weighted images and shows rim enhancement. On MRI, the lesion extends through the physis and has an irregular extension into the epiphysis. The surrounding bone marrow and soft tissues show edema and mild enhancement, with no soft tissue mass ( Figs. 73.3–73.5 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree