Chapter 42 Protocols for Imaging Studies in the Oncologic Patient
Well-thought-out protocols imaging sophisticated imaging studies are critical to ensure that the resultant images have the best possible chance to answer the clinical question. In the case of oncologic patients, this usually hinges on whether disease is stable, has regressed, or has progressed and whether there are new sites of disease. Beyond this fundamental question, our patients may have unexpected findings as well as complications from therapy. The ability to answer such questions relies on high-quality images and, in the case of computed tomography (CT), the best quality titrated with the least radiation exposure because patients generally go into a lifetime of surveillance. This is a significant challenge. In patients undergoing imaging for surgical intervention, especially for cure, these studies need to be directly targeted to the most likely sites of metastases (e.g., high-quality liver imaging for metastases in patients with orbital, choroidal melanoma) and have optimal image quality to detect metastatic disease.1–5 Imaging with multidetector computed tomography (MDCT) can be performed in multiple phases, and developing protocols to detect hyper- as well as hypovascular metastases is critical in evaluating patients with tumors such as carcinoid, islet cell tumors of the pancreas, and a number of other primaries. Timing of the contrast bolus and subsequent imaging is critical in magnetic resonance imaging (MRI) as well as current MDCT scanning.6–8
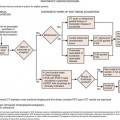
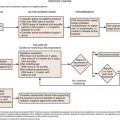
The protocols in this chapter can be accessed online at expertconsult.com. The charts provide a selection of common protocols developed by authors of this textbook and utilized in their daily practice. The protocols were prepared January 2010. They are grouped together in one chapter rather than being individually recorded for the reader’s convenience. They are simply provided for a reference within the context of this textbook, and scanning protocols should be developed and tailored to each individual physician’s practice.
MDCT: CT Imaging
Chest Protocols (MDCT 64 Slice)
Abdomen/Pelvis Protocols (MDCT 64 Slice)
Abdomen without and with Contrast
Abdomen and Pelvis with Contrast
Abdomen and Pelvis without Contrast
Abdomen and Pelvis without and with Contrast
Adrenals: Abdomen with Contrast
Adrenals: Abdomen without and with Contrast
Adrenals: Abdomen and Pelvis with Contrast
Adrenals: Abdomen and Pelvis without and with Contrast
Adrenals: Chest and Abdomen with Contrast
Adrenals: Chest and Abdomen without and with Contrast
Adrenals: Chest, Abdomen, and Pelvis with Contrast
Adrenals: Chest, Abdomen, and Pelvis without and with Contrast
Angiogram/Venogram: Abdomen and Pelvis
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree