, Gustav Andreisek2 and Erika J. Ulbrich2
(1)
Phoenix Diagnostic Clinic, Cluj-Napoca, Romania
(2)
Institute of Diagnostic and Interventional Radiology, University Hospital Zürich, Zürich, Switzerland
8.1 Anatomy and Normal MRI Appearance
8.1.1 Capsule and Synovial Compartments
The articular capsule of the knee consists of a thick outer layer, the fibrous capsule, and a thinner inner layer, the synovial membrane (synovium).
The synovium is a mesenchymal tissue composed of two to three layers of specialized cells (synoviocytes) and a supporting connective tissue that includes a well-developed vascular network and relatively abundant adipose tissue [1]. This hypervascular membrane is responsible for the secretion of the synovial fluid, which lubricates and nourishes the joint [2]. The synoviocytes also have a role in removing intra-articular particles including cartilaginous debris [2].
The knee joint can be seen as common joint space that is subdivided by synovial membranes into several interconnected compartments. Anteriorly, at the central femoropatellar compartment, the synovial membrane attaches to the patellar borders and extends circumferentially beneath vastus lateralis and vastus medialis muscles to the anterior femoral shaft. It covers also the anterior aspects of the cruciate ligaments. The medial and lateral femorotibial compartments of the synovial membrane are represented by the lateral and medial extensions of the central portion [2]. These compartments are separated by the infrapatellar synovial fold anteriorly and by a reflection of the synovium that extends from the sides of the posterior cruciate ligament onto the fibrous capsule, posteriorly [2]. The anterior and posterior cruciate ligaments, menisci, and the infrapatellar fat pad are located “extrasynovially” which means that they are located outside the abovementioned synovial compartments.
8.1.2 Synovial Bursae and Synovial Recesses
Synovial bursae or synovial recesses are extensions of the synovial membrane between different anatomical structures, and their role is to reduce the friction during the motion of these structures. The knee bursae are numerous and, in the absence of pathological changes, rarely apparent on MR imaging [3]. The knowledge of the locations of synovial bursae is important since in pathological conditions, they may become apparent and a cause for misdiagnosis or diagnostic uncertainty [2]. The classification of the bursae is made on their anatomic location (Table 8.1). Readers of MR images should look for anterior and posterior bursae on sagittal planes and for medial and lateral bursae on axial planes. However, they should have in mind that normal bursae are generally not visible on MR imaging.
Compartment | Bursa/recess | Anatomy |
|---|---|---|
Anterior | Suprapatellar bursa (Fig. 8.2) | Located between the quadriceps tendon and femur |
Prepatellar bursa (Fig. 8.3) | Superficially located between the patella and subcutaneous tissue | |
Superficial infrapatellar or pretibial bursa | Superficially located between the tibial tubercle and subcutaneous tissue | |
Deep infrapatellar bursa (Fig. 8.4) | Located posterior to the distal part of the patellar tendon between the tendon and anterior tibia | |
Suprahoffatic recess (Fig. 8.5) | Located close to the inferior border of the patella | |
Infrahoffatic recess (Fig. 8.5) | Located anterior to the inferior portion of the infrapatellar plica (also called ligamentum mucosum) | |
Central synovial recess (Fig. 8.6) | Located anterior to the anterior cruciate ligament | |
Posterior | Medial posterior femoral recess or medial gastrocnemius bursa (Fig. 8.7) | Located between the posterior horn of the medial meniscus and the knee capsule and the medial head of the gastrocnemius muscle; may communicate with the articular cavity |
Lateral posterior femoral recess or lateral gastrocnemius bursa (Fig. 8.7) | Located between the posterior horn of the lateral meniscus and the knee capsule and lateral head of the gastrocnemius muscle; may communicate with the articular cavity | |
Gastrocnemius-semimembranosus bursa (Fig. 8.8) | Double-bursa located between the semimembranosus and the medial head of the gastrocnemius muscle | |
Subpopliteus bursa (Fig. 8.9) | Located between the posterior horn of the lateral meniscus and the popliteus tendon; communicates with the superior tibiofibular joint in 10 % of adults | |
Posterior capsular recess (Fig. 8.10) | Located in the midline behind the posterior cruciate ligament; is an extension of the medial femorotibial compartment | |
Lateral | Iliotibial bursa | Located between the distal portion of the iliotibial band and the adjacent tibia |
Lateral collateral ligament-biceps femoris bursa (Fig. 8.11) | Located at the fibular insertion, the lateral collateral ligament and the biceps tendon form a conjoined tendon. Between the two structures, the lateral collateral ligament-biceps femoris bursa is constantly described | |
Parameniscal recesses (Fig. 8.12) | Located superior and inferior to the level of the lateral meniscus in contact with the lateral femoral and tibial condyle | |
Medial | Medial collateral bursa | Located between the superficial and deep layer of medial collateral ligament |
Pes anserinus bursa | Located between the pes anserinus (tendons of sartorius, gracilis, and semitendinosus muscles) and the medial collateral ligament; does not typically communicate with the joint | |
Medial collateral ligament-semimembranosus bursa | Located between the semimembranosus tendon and the medial collateral ligament |
8.1.3 Synovial Plicae
Synovial plicae are normal anatomical structures representing embryologic remnants of the synovial membrane and are defined as thin, vascularized synovial folds without a known function [2, 4]. The plicae are usually asymptomatic, and they can be found at MR imaging within the knee joints as low-signal-intensity thin bands (Fig. 8.1). The most encountered plicae of the knee are the suprapatellar plica, the infrapatellar plica, the lateral patellar plica, and the mediopatellar plica (Table 8.2).
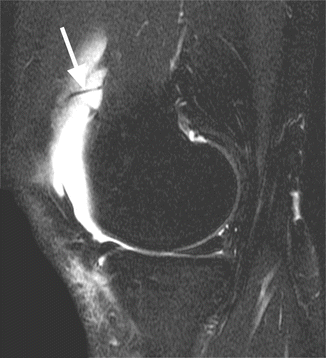
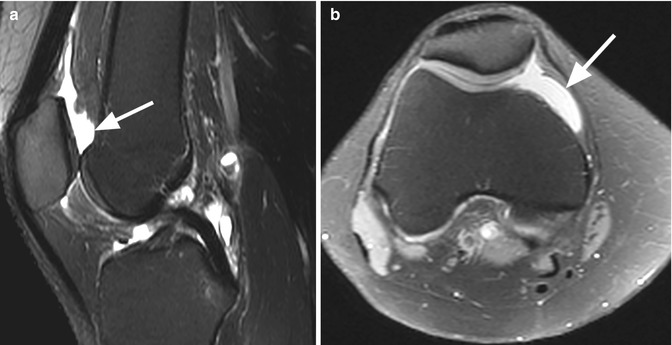
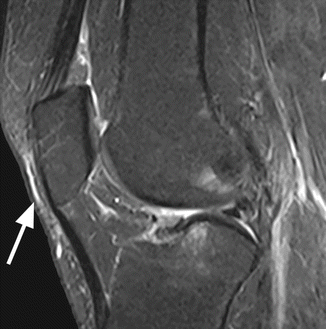
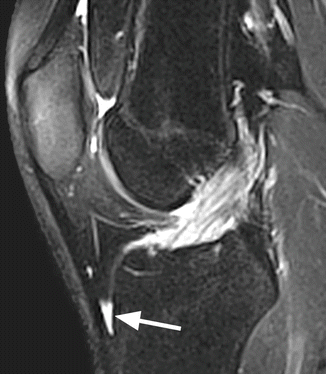
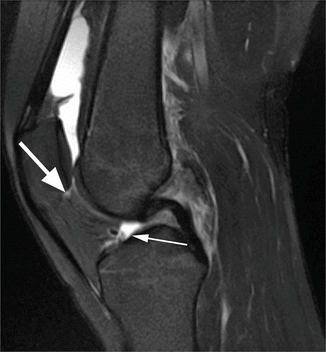
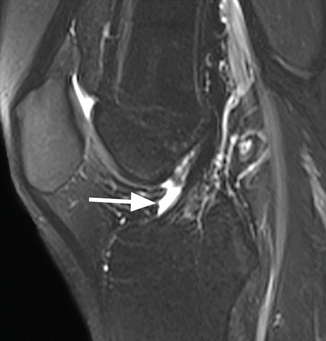
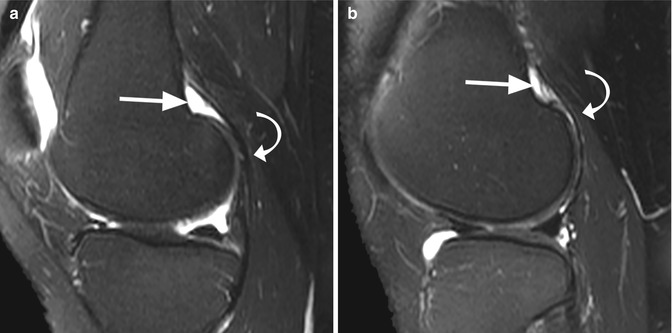
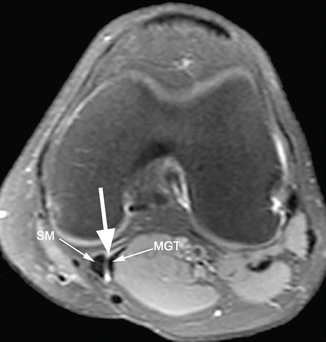
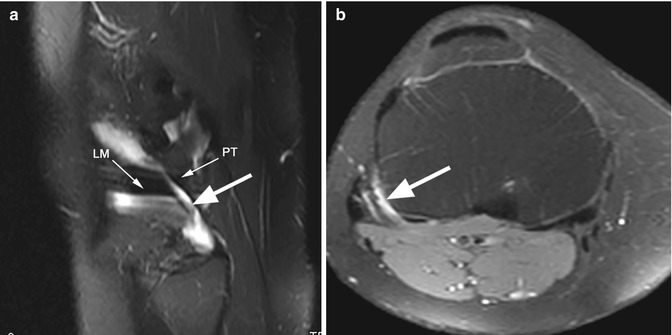
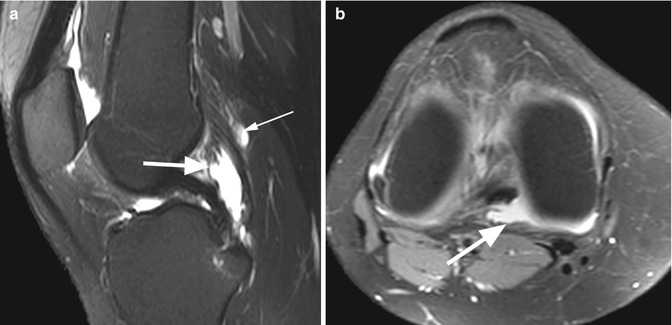
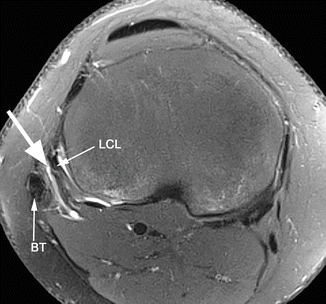
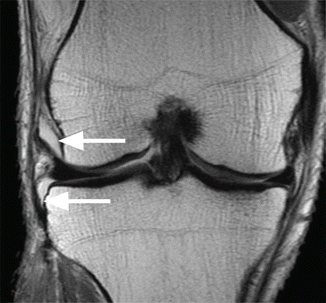
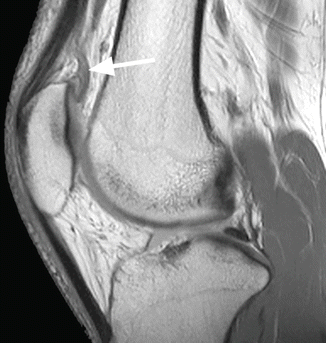
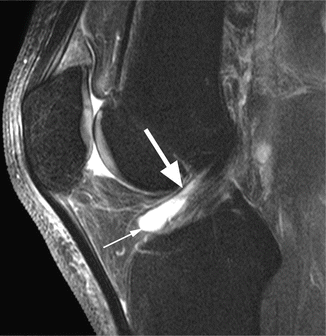
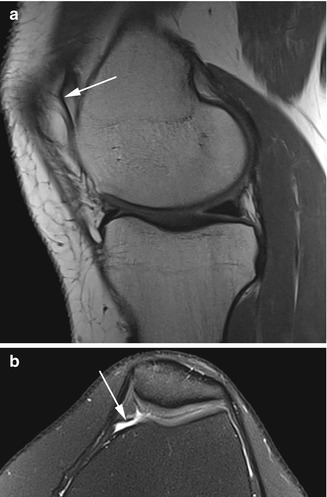
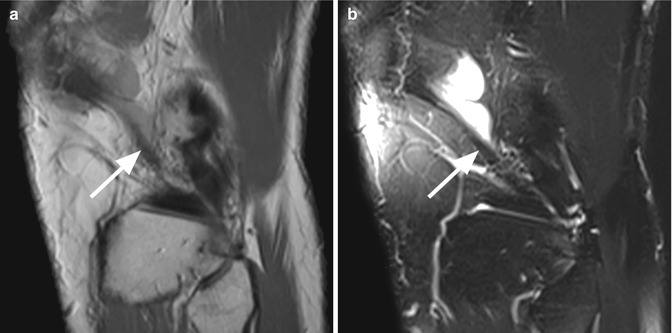

Fig. 8.1
Suprapatellar plica in a 28 year old female. Sagittal T2-weighted fat-suppressed image shows the synovial plica as a low-signal-intensity thin band (arrow)

Fig. 8.2
Suprapatellar bursa in a 40 year old female. Sagittal T2-weighted fat-suppressed image (a) and axial proton-density (PD) fat-suppressed image (b) show the fluid in the suprapatellar bursa (arrow)

Fig. 8.3
Prepatellar bursa in a 55 year old male. Sagittal T2-weighted fat-suppressed image shows a small amount of fluid in the prepatellar bursa (arrow)

Fig. 8.4
Deep infrapatellar bursa in a 22 year old female. Sagittal T2-weighted fat-suppressed image shows the deep infrapatellar bursa posterior to the distal part of the patellar tendon between the tendon and anterior tibia (arrow)

Fig. 8.5
Suprahoffatic and infrahoffatic recesses in a 19 year old female. Sagittal T2-weighted fat-suppressed image shows the suprahoffatic recess (large arrow) close to the inferior border of the patella and the infrahoffatic recess (small arrow)

Fig. 8.6
Central synovial recess in a 30 year old female. Sagittal T2-weighted fat-suppressed image shows the recess located anterior to the anterior cruciate ligament (arrow)

Fig. 8.7
Medial posterior femoral recess (medial gastrocnemius bursa) and lateral posterior femoral recess (lateral gastrocnemius bursa) in a 40 year old female. Sagittal T2-weighted fat-suppressed images through the medial compartment (a) and lateral compartment (b) show the medial gastrocnemius bursa (arrow in a) between the knee capsule and the medial head of the gastrocnemius muscle (curved arrow in a) and the lateral gastrocnemius bursa (arrow in b) between the knee capsule and the lateral head of the gastrocnemius muscle (curved arrow in b)

Fig. 8.8
Gastrocnemius-semimembranosus bursa (popliteal cyst or Baker’s cyst) in a 36 year old male. Axial proton-density (PD) fat-suppressed image shows a small amount of fluid in the popliteal bursa (arrow) which is located between the semimembranosus (SM) and the medial head of the gastrocnemius muscle (MGT)

Fig. 8.9
Subpopliteus bursa in a 40 year old female. Sagittal T2-weighted fat-suppressed image (a) and axial proton-density (PD) fat-suppressed image (b) show the subpopliteal bursa (large arrow in a, b) located between the posterior horn of the lateral meniscus (LM) and the popliteus tendon (PT)

Fig. 8.10
Posterior capsular recess in a 40 year old female. Sagittal T2-weighted fat-suppressed image (a) and axial proton-density (PD) fat-suppressed image (b) show the posterior capsular recess (large arrow in a, b) located in the midline behind the posterior cruciate ligament. In cases of posterior capsule lesions, the fluid from this recess may be identified posteriorly to the capsule (small arrow in a)

Fig. 8.11
Lateral collateral ligament-biceps femoris bursa in a 25 year old male. Axial proton-density (PD) fat-suppressed image shows a small amount of fluid in the lateral collateral ligament-biceps femoris bursa (large arrow) which is located between the lateral collateral ligament (LCL) and the biceps femoris tendon (BT)

Fig. 8.12
Parameniscal recesses in a 41 year old male. Coronal proton-density (PD) image shows the parameniscal recesses (arrows) in contact with the lateral femoral and lateral tibial condyle
Anatomy | MR imaging appearance | |
|---|---|---|
Suprapatellar plica (Fig. 8.13) | Located between the suprapatellar bursa and the knee joint cavity; runs from the posterior aspect of quadriceps tendon, above the patella upward to the anterior aspect of the femur | Low-signal-intensity linear band posterior to the patella |
Infrapatellar plica or ligamentum mucosum (Fig. 8.14) | The most commonly plica in the knee; runs from the femoral origin anterior to the intercondylar notch downward to the inferior pole of the patella | Low-signal-intensity band of various dimensions anterior and parallel to the anterior cruciate ligament, often within the infrapatellar fat pad |
Mediopatellar plica (Fig. 8.15) | Runs from the medial capsule of the knee obliquely downward to the synovium of the infrapatellar fat pad | Low-signal-intensity linear band that may be connected to the suprapatellar plica; can extend between the medial facet of the patella and medial face of the trochlea |
Lateral patellar plica (Fig. 8.16) | The least common plica of the knee; runs from the popliteus hiatus and attaches to the infrapatellar fat pad | Low-signal-intensity linear longitudinal band 1–2 cm lateral to the patella |

Fig. 8.13
Suprapatellar plica in a 33 year old male. Sagittal proton-density (PD) image shows the suprapatellar plica within the suprapatellar fat pad (arrow). The plica appears thickened indicating a suprapatellar plica syndrome

Fig. 8.14
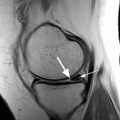
Infrapatellar plica or ligamentum mucosum in a 43 year old male. Sagittal T2-weighted fat-suppressed image shows the ligamentum as low-signal-intensity thin band (large arrow) anterior and parallel to the anterior cruciate ligament. Note the fluid in the central synovial recess (small arrow)

Fig. 8.15
Mediopatellar plica in a 26 year old male. Sagittal proton-density (PD) image (a) and axial proton-density (PD) fat-suppressed image (b) show a normal mediopatellar plica (arrow in a, b) as a thin low-signal-intensity band in the medial suprapatellar fat pad

Fig. 8.16
Lateral patellar plica in a 38 year old male. Sagittal proton-density (PD) image (a) and sagittal T2-weighted fat-suppressed image (b) show the lateral patellar plica (arrow in a, b) extending from the popliteus hiatus to the patella
8.2 MRI Pathological Findings
8.2.1 Joint Effusions
Synovial Fluid
The synovial fluid is a viscid fluid secreted by the synovium. The knee synovial fluid is commonly depicted on MR imaging, but a definitive criterion that enables to define the quantity of the effusion as normal or pathological has not been clearly established. Clinically, knee effusions of less than 6–8 mL cannot be appreciated. However, on MR imaging, a volume of 1 mL of effusion may be visible adjacent to the femoral condyles [13]. Some authors demonstrated that a volume of 4 mL of fluid is depicted on plain radiography and, on midline sagittal MR images, leads to an anteroposterior diameter of the midline suprapatellar recess of 4 mm [13, 14]. This volume of effusion was considered to be clinically important [15]. With increasing volumes of effusion, the fluid first collects in the suprapatellar bursa and subsequently in the posterior recesses and popliteal tendon sheath [13].
Although the knee effusion may be the only finding on MR imaging, most commonly the synovial fluid is the result of a different underlying pathology (e.g., inflammatory diseases, trauma, degenerative changes, tumors). On MR imaging, the joint fluid appears homogeneously hypointense or of intermediate signal intensity on T1-weighted images and hyperintense on T2-weighted images.
Hemarthrosis and Lipohemarthrosis
Hemarthrosis is the result of the hemorrhage within the joint due to ligamentous injury, bone fracture, patellar dislocation, or other diseases including pigmented villonodular synovitis, hemophilia, articular tumors, neuroarthropathy, gout, and anticoagulant therapy [12, 16, 17]. The MRI appearance of hemarthrosis depends on the stage of the hemorrhage. In the early stage, the hemorrhage has a double-layer fluid level appearance with a superior layer of blood serum floating on an inferior layer of cellular debris of intermediate signal intensity on T1- and T2-weighted images. Gradient-echo images are especially useful for the identification of blood products due to the “blooming” effect.
Lipohemarthrosis, the presence of blood and fat within the joint, is a very strong indicator for intraarticular fracture. Most commonly, lipohemarthrosis is seen on MR imaging as a three-layer fluid level that appears approximately 3 h after trauma (Fig. 8.17) [18]. The superior layer with fat signal intensity (hyperintense on T1- and T2-weighted images and hypointense on fat-suppressed images) represents the floating fat. The intermediate or the central layer appears as a normal joint fluid and represents the blood serum, and the inferior layer of cellular debris is seen as intermediate signal intensity on T1- and T2-weighted images. In the very early stage, lipohemarthrosis may show a double-layer appearance with entrapment of globules of fat [18].
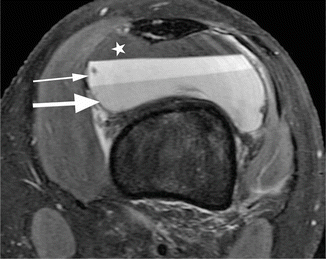

Fig. 8.17
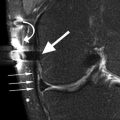
Lipohemarthrosis in a 16 year old female. Axial proton-density (PD) fat-suppressed image shows the superior layer of floating fat which appears hypointense on fat-suppressed sequences (star), the intermediate or the central layer which appears as a normal joint fluid and represents the blood serum (small arrow), and the inferior layer of cellular debris which is seen as intermediate signal intensity (large arrow)
8.2.2 Intra-articular Bodies
Intra-articular bodies are best depicted on MR imaging in the presence of joint effusion as they are nicely outlined by the surrounding joint fluid. They appear as filling defects within the fluid (Figs. 8.18, 8.19, 8.20, and 8.21). The best technique to visualize intra-articular bodies is direct MR arthrography where the contrast agent is administered directly into the joint space increasing the amount of the intra-articular joint fluid. However, in the knee, intra-articular bodies are often large, and usually there is enough joint fluid present. Thus, MR arthrography in the knee for the detection of intra-articular bodies is not recommended as a standard procedure, but can be helpful in cases where intra-articular bodies are suspected but cannot be otherwise detected.
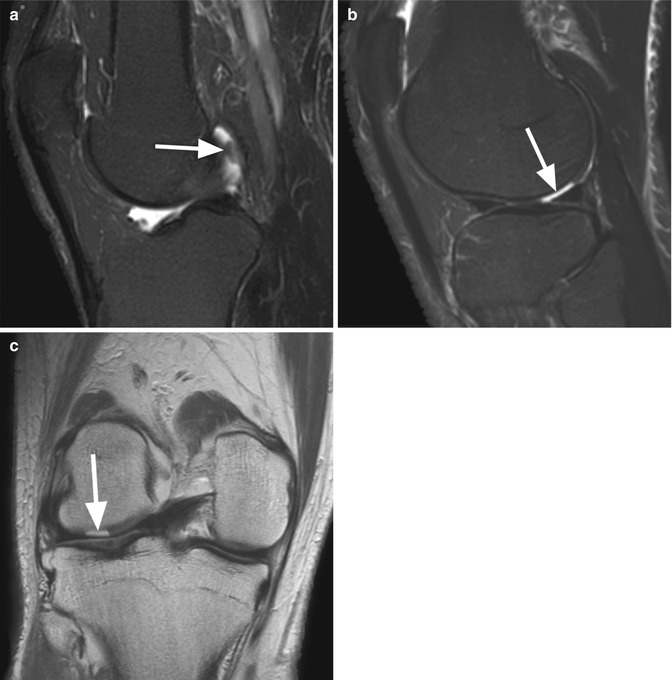
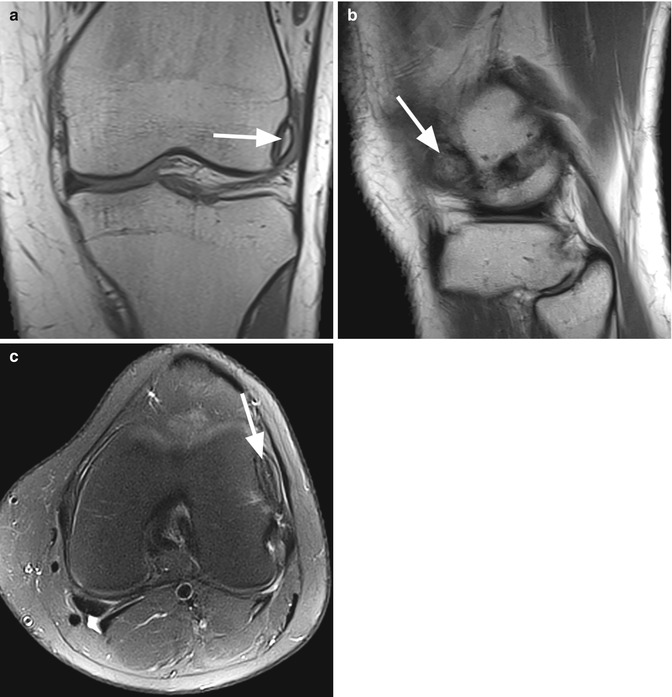
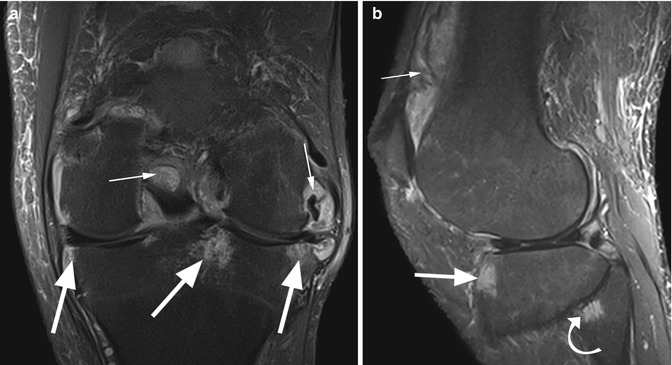
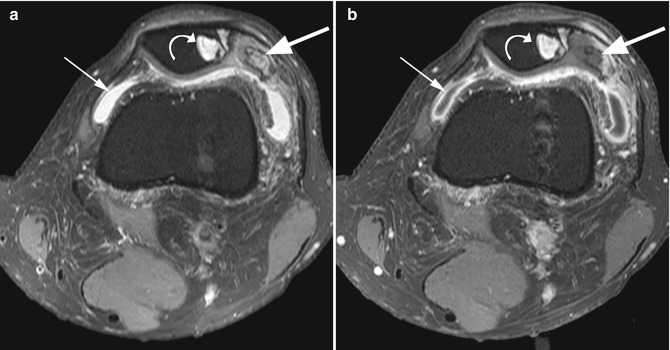

Fig. 8.18
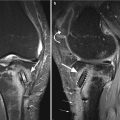
Intra-articular free cartilage fragment in a 43 year old male. Sagittal T2-weighted fat-suppressed image (a) shows a small fragment of cartilage surrounded by joint fluid (arrow). Sagittal T2-weighted fat-suppressed image (b) and coronal proton-density (PD) image (c) demonstrate the lateral femoral condyle as the donor site (arrows in b, c)

Fig. 8.19
Detached bone fragment in a 21 year old female 3 years after knee injury. Coronal T1-weighted image (a), sagittal proton-density (PD) image (b), and axial proton-density (PD) fat-suppressed image (c) show a bone fragment detached from the lateral femoral condyle (arrows). The chronicity of the condition is demonstrated by the synovial reaction around the lesion and the absence of bone marrow edema

Fig. 8.20
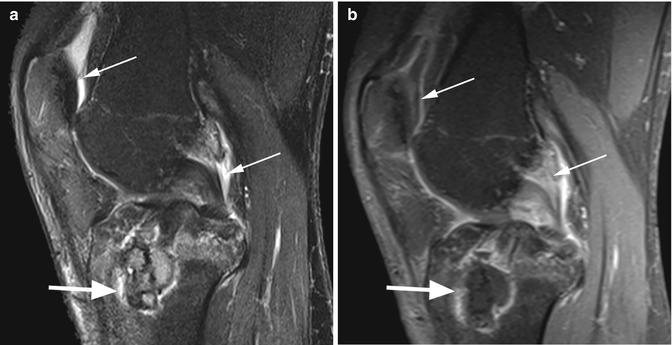
Rheumatoid arthritis in a 45 year old male. Coronal proton-density (PD) fat-suppressed image (a) shows small innumerable nodules within the synovial membrane (small arrows). Subchondral erosions are seen in the tibial subchondral bone (large arrows). Sagittal T2-weighted fat-suppressed image (b) also shows subchondral bone marrow edema of the anterior tibial plateau (large arrow), synovitis (small arrow), and erosion of the fibular head (curved arrow)

Fig. 8.21
Acute gout in a 55 year old male. Axial proton-density (PD) fat-suppressed image (a) and axial T1-weighted fat-suppressed postcontrast image (b) show the gout tophus of relatively high signal intensity on a fat-suppressed image (large arrow in a) but without enhancement after contrast administration (large arrow in b). Subchondral cysts are seen within the adjacent patella (curved arrows in a, b) resulting from repetitive gout attacks. The synovia is thickened and joint effusion is present (small arrows in a, b)
Intra-articular bodies may have different etiologies, and the MRI signal appearance depends on the structure and origin of the bodies (Table 8.3). In the knee, intra-articular bodies are usually found beneath the medial collateral ligament, within the intercondylar notch, and in the tendon sheath of the popliteus tendon, or they can migrate into Baker’s cysts [12]. It needs to be noted that intra-articular bodies are difficult to detect during arthroscopy, i.e., when they are located in recesses or compartments, which are hardly or even non-accessible by the arthroscope.
Etiology/structure | MRI findings |
|---|---|
Cartilage/meniscus (Fig. 8.18) | Similar signal intensity with joint cartilage/meniscus; MR images should be carefully scrutinized for donor site; the size of the body should match the size of the donor site |
Bone (Fig. 8.19) | Signal intensity of bone marrow; MR images should be carefully scrutinized for donor site |
Osteochondral fragment | Cortical bone of low signal intensity on all MR sequences with attached cartilage of intermediate signal intensity on T1- and T2-weighted; may mirror the defect at the donor site |
Inflammatory synovitis (including tuberculosis) (Fig. 8.20) | Intermediate- to low-signal-intensity small innumerable nodules along the synovial membrane (rice bodies) |
Gout (Fig. 8.21) | Soft tissue tophi of monosodium urate crystal deposits with inhomogeneous T2-weighted signal intensity; enhances after i.v. contrast administration |
Primary synovial osteochondromatosis | Multiple circumscribed nodules of metaplastic hyaline cartilage (range from 2.0 mm to more than 1.0 cm); the signal intensity varies according to the maturity of the nodules and the presence of calcifications within the nodules; may present as conglomerate mass |
Pigmented villonodular synovitis | Conglomerate or scattered nodules within the joint; low signal intensity on T1-weighted images and low to high signal intensity on T2-weighted images; “blooming” on gradient-echo images due to iron deposition |
Hemophilic arthropathy | Similar appearance with pigmented villonodular synovitis |
Metallic foreign bodies | Filling defects with susceptibility artifacts |
Intra-articular gas | Low-signal-intensity globular filling defects with “blooming” on gradient-echo images |
8.2.3 Synovitis
Synovitis, the inflammation of the synovial membrane, can be the result of several disorders including inflammatory arthritis, osteoarthritis, infection, pigmented villonodular synovitis, chronic intra-articular hemorrhage, metabolic diseases, tumors, and trauma. The MR imaging diagnosis of synovitis is based on the evaluation of the synovium thickness and the presence of synovial effusion. The synovial hypertrophy may involve the entire knee synovium or may be focal and is seen on T2-weighted and on gradient-weighted images as hyperintense synovial membrane having a thickness of more than 2–3 mm (Fig. 8.22) [19]. A better appreciation of synovitis is obtained on postcontrast T1-weighted MR images that enable a superior delineation of the hypertrophied synovial membrane from the joint effusion (Fig. 8.23). Due to hyperemia of the inflamed synovium, there is an increased synovial enhancement on postcontrast T1-weighted images that can be also used to differentiate between acute and chronic inflammation.
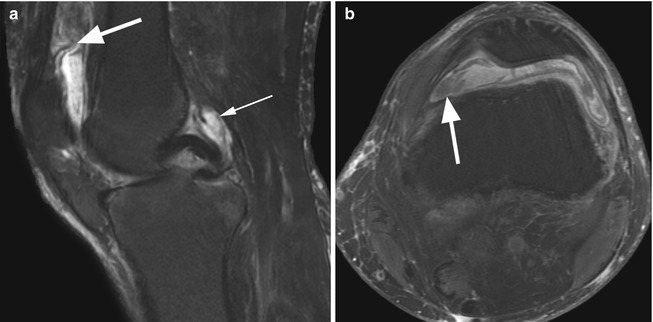
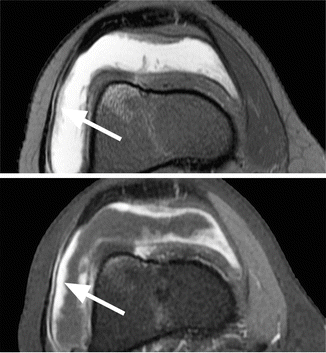

Fig. 8.22
Chronic synovitis in a 65 year old male. Sagittal T2-weighted fat-suppressed image (a) and axial proton-density (PD) fat-suppressed image (b) show a synovium with a thickness of more than 3 mm but without a clear delineation from the joint fluid (large arrows in a, b). Note the diffuse involvement of the entire synovium including the posterior recess (small arrow in a)

Fig. 8.23
Acute synovitis in a 25 year old female. Axial proton-density (PD) fat-suppressed image (a) shows synovial hypertrophy and irregularity (arrow). Axial T1-weighted fat-suppressed postcontrast image (b) shows an increased enhancement and enables a superior delineation of the hypertrophied synovial membrane (arrow) from the joint effusion
Signal alterations in Hoffa’s fat pad are a finding that can be seen in a multitude of diseases and can be used as a surrogate for knee synovitis [20–22].
Inflammatory Synovitis in Rheumatological Disorders
In rheumatological disorders (rheumatoid arthritis, psoriatic arthritis, and ankylosing spondylitis), the synovium is affected first, followed by involvement of the cartilage and bones. MR imaging enables the diagnosis of all intra-articular pathological changes including synovitis and joint effusion, bone marrow edema, and subchondral erosions (Fig. 8.20). There are different MRI techniques used in the evaluation of the synovial proliferation that are used either for qualitative or quantitative evaluation. Synovitis is best identified on T2-weighted images and postcontrast T1-weighted images as uniform or irregular thickening of the synovial membrane. Different quantitative evaluations of synovitis have been described including the synovial volume measurement and the rate of contrast enhancement. Dynamic contrast-enhanced T1-weighted sequences may differentiate between active and chronic phases of the disease with a rapid synovial enhancement (30–60 s) after contrast administration in active or acute phases [23, 24]. Nevertheless, synovial volume or enhancement rate measurements require post-processing work, which is time consuming in clinical practice and thus rarely used [12]. Apart from demonstrating the synovial proliferation, MRI demonstrates periarticular inflammation and tendon and ligament inflammation as well as complications such as ruptures of the tendons, presence of “rice-bodies” bursitis, osteonecrosis, and stress fractures [25, 26].
Although rheumatoid arthritis and the seronegative spondyloarthropathies share similar pathological changes, several findings can narrow the differential diagnosis [12]. In rheumatoid arthritis, there are symmetrical abnormalities, and the extent of subchondral erosions and the degree of synovial inflammation are more prominent. However, intra-articular rheumatoid nodules are rarely seen [27]. The rheumatoid nodules are solitary or multiple nodules that appear as inhomogeneous isointense or hypointense lesions on T1-weighted images and inhomogeneous isointense or hyperintense on T2-weighted images compared with muscles (Fig. 8.24). They may enhance homogeneously or heterogeneous predominantly in the periphery. In ankylosing spondylitis and other seronegative spondyloarthropathies, the knee joint is involved in 30 % of the patients with long-standing disease, and the bone marrow edema has a perientheseal distribution that is not commonly seen in patients with rheumatoid arthritis [12, 28]. The osseous fusion is also more common in seronegative spondyloarthropathies. Overall, however, differential diagnosis remains difficult on MR images, and in the clinical routine, one might not be disappointed when a final diagnosis cannot be made with 100 % confidence.
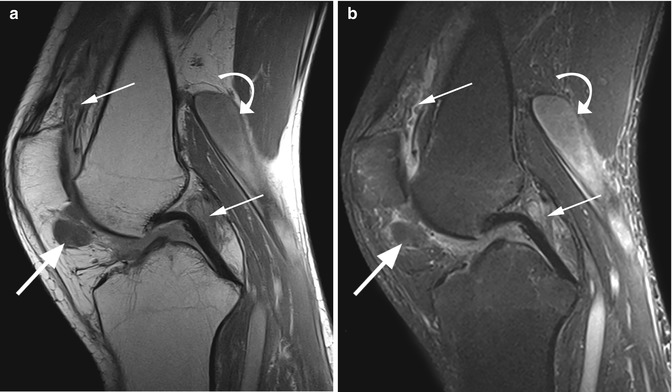

Fig. 8.24
Rheumatoid nodules in a 45 year old male with rheumatoid arthritis. Sagittal proton-density (PD) image (a) and sagittal T2-weighted fat-suppressed image (b) show two infrapatellar nodules with signal intensity similar to muscles (large arrows in a, b). Note the synovitis in the suprapatellar bursa and central recesses (small arrows in a, b) as well as the inflammation of the Baker’s cyst (curved arrow in a, b) which appears with inhomogeneous signal intensity and diffuse pericystic changes
Synovitis in Osteoarthritis
Synovial proliferation and joint effusion in osteoarthritis is the result of ligament injuries, loose bodies, cartilage deterioration, and meniscal damage (Fig. 8.25) [29, 30]. Synovitis is present even in the early phase of osteoarthritis, and there is evidence that synovial proliferation is not only a secondary phenomenon but that it also plays a role in progression of cartilage loss [29]. Synovial inflammation is believed to contribute to pain in patients with knee osteoarthritis, and several studies have indeed shown that high-grade synovitis in patients with knee osteoarthritis is statistically associated with pain [29, 31].
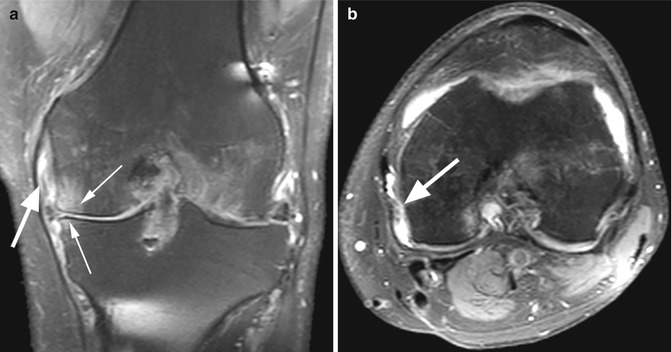

Fig. 8.25
Chronic medial collateral bursitis in a 45 year old male with advanced medial knee osteoarthritis. Coronal proton-density (PD) fat-suppressed image (a) and axial proton-density (PD) fat-suppressed image (b) show the presence of fluid between the superficial and the deep layers of the medial collateral ligament (MCL) (large arrows in a, b). Note the subchondral edema and the cartilage absence in the medial compartment (small arrows in a)
Infectious Synovitis
The imaging findings in infectious synovitis are nonspecific, and MRI cannot differentiate septic from nonseptic arthritis. The clinical history is key for differential diagnosis. Early detection of infectious synovitis is crucial in the treatment management and in preventing bone deformities. Thus, if there is clinical suspicion for infection, MR should be performed immediately and any destructive monoarticular process should be regarded as infection until proven otherwise [12]. There are several MRI findings that suggest an infectious etiology. These include synovial thickening, soft tissue edema, and extensive bone marrow edema with enhancement involving both sides of articulation and bone erosions (Fig. 8.26) [32, 33]. Inhomogeneous joint effusion with septa and debris or the presence of synovial or bone abscess is highly correlated with septic arthritis (Fig. 8.26). The evolution and the variation of the imaging findings can help narrowing down the differential diagnosis. In bacterial arthritis, there is a rapid evolution with extensive erosions, whereas in tuberculosis, the evolution is slow and the granulation inflammatory tissue extends in the subchondral bone (pannus) [12].