The peritoneal cavity is formed by the fourth embryonic week and is derived from the mesoderm.
2 The abdominopelvic cavity is lined with a thin continuous layer of peritoneum. The cavity is completely sealed in males but communicates with the external environment via the fallopian tubes in females. Peritoneum that envelops the organs is referred to as
visceral peritoneum, and the peritoneal layer that lines the walls of the abdominopelvic cavity is referred to as
parietal peritoneum. This thin layer coating all surfaces of the peritoneal cavity and its organs secretes a small amount of serous fluid, approximately 50 mL, which acts to lubricate visceral surfaces, allowing them to move without friction.
1As organs develop along the posterior abdominal wall and protrude into the peritoneal cavity, they are covered by visceral peritoneum except at their hilum, where blood vessels, nerves, and lymph enter and exit the organ. The hila of peritoneal organs are considered bare areas because they lack a peritoneal covering. These bare areas are part of the retroperitoneum.
Divisions of the Peritoneal Cavity
The peritoneal cavity is generally divided into two compartments: the greater sac and the lesser sac. The
greater sac is the largest, housing the liver, spleen, stomach, first portion of the duodenum, jejunum, ileum, cecum, transverse colon, sigmoid colon, and the upper two-thirds of the rectum.
1 This large sac contains several potential spaces that must be evaluated for free fluid.
The lesser sac may be thought of as a diverticulum of the greater sac and is also referred to as the omental bursa by some. The lesser sac does not contain any organs. This potential space lies immediately posterior to the stomach, extending superiorly to the left suprahepatic recess between the posterior left lobe of the liver and the left hemidiaphragm.
The lesser sac extends inferiorly into the fold of the greater omentum. This may also be referred to as the
inferior recess of the lesser sac or
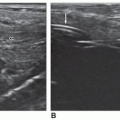
omental bursa. Note that this fold is patent in infants and small children but generally fuses in adults, thereby significantly limiting the caudal extent of the lesser sac (
Fig. 5-3A, B). The lesser sac’s anterior wall is formed by the posterior stomach, whereas superiorly it is enclosed by the lesser omentum, also called
hepatogastric ligament. The splenorenal and gastrosplenic ligaments create the left lateral wall of this pocket (
Fig. 5-4). The omental foramen, also called the
foramen of Winslow, is located at the right lateral aspect of the lesser sac and is the only opening communicating with the greater sac. This opening is found posterior to the
hepatoduodenal ligament, the thickened right border of the lesser omentum that guides the portal triad into the liver (
Fig. 5-4).
The lesser omentum—also called the
small omentum,
gastrohepatic omentum, and
gastrohepatic ligament—is a fused double layer of peritoneum stretching between the lesser curvature of the stomach and the left sagittal fissure for the ligamentum venosum (transverse fissure). This ligament creates the anterior superior border of the lesser sac, separating it from the supracolic compartment of the greater sac (
Fig. 5-5).
Within the greater sac is a large apron-like double-layered sheet of peritoneum called the
greater omentum that extends inferiorly from the greater curvature of the stomach and transverse colon. The greater omentum extends inferiorly, anterior to the bowel, folds inward, and travels superiorly to attach on the transverse colon. The anterior and posterior adjacent layers are separate in infants but typically fused
in adults and contain a variable amount of fat
3 (
Fig. 5-3). The greater omentum functions to prevent the parietal peritoneum of the anterior abdominal wall from adhering to the visceral peritoneum. This mesenteric drape is very mobile and moves to areas of inflammation, surrounding the inflamed area by creating adhesions to wall off infection (
Fig. 5-6A, B). It also acts to cushion the abdominal organs to prevent trauma and acts to prevent the loss of body heat from abdominal organs.
The greater omentum subdivides the greater sac into a supracolic (above the colon) compartment and an infracolic (below the colon) compartment. The supracolic compartment is located anterior to the greater omentum and stomach and inferior to the liver. The infracolic compartment is located posterior to the greater omentum, surrounding the small bowel and colon within the remainder of the greater sac (
Fig. 5-7). This division is important because it limits the spread of infected materials, pus, ascitic fluid, and malignant
cells within the peritoneal cavity. Communication between these two compartments is via the paracolic gutters, the lateral borders of the ascending and descending colon.
Potential Spaces of the Peritoneum
As organs grow into the peritoneal cavity, several pockets and recesses are formed by the organs, their vascular connections, and suspensory ligaments, thereby creating a complex landscape for sonographers to examine when performing abdominal and pelvic examinations. Ligaments divide portions of the peritoneal cavity. Sonographers require a working knowledge of these ligaments to understand where to look for fluid within the peritoneal sac and how to image and describe its location. See
Table 5-1 for a description of the ligaments of the peritoneal cavity.
Potential spaces are areas created by the peritoneal layer, reflecting between two organs or an organ and the peritoneal wall (typically posterior). A potential space is an empty fold; however, when disease is present, fluid or other materials may collect in this space. Because many pathologies present with excretions (ascitic fluid, blood, pus) into the peritoneal cavity, sonographers must examine these potential spaces and characterize the fluid as part of the abdominal and pelvic examinations. The following text includes anatomic descriptions of each major potential space of the peritoneal cavity.
Left Anterior Subphrenic Space
The left anterior subphrenic or suprahepatic space is an extension of the greater sac between the diaphragm and the anterior superior liver leftward of the falciform ligament.
Left Posterior Suprahepatic Space
The left posterior suprahepatic space is also called the
superior recess of the lesser sac; this space is an extension of the lesser sac between the diaphragm and the posterior superior liver. See
Figures 5-3 and
5-7.
Right Subphrenic Space
The right subphrenic or suprahepatic space is an extension of the greater sac between the right hemidiaphragm and the anterior superior liver rightward of the falciform ligament (
Fig. 5-8).
Hepatorenal Space
The hepatorenal space is also referred to as
Morrison pouch. This peritoneal potential space is created by the peritoneum, reflecting from the liver over the right kidney and right posterior peritoneal wall. When the patient is in a supine position, this space is the most gravity-dependent potential space of the abdominal cavity, collecting fluid from the supracolic area and the lesser sac. See
Figure 5-8.
Omental Bursa
The omental bursa, or lesser sac, is sandwiched between the posterior stomach and parietal peritoneum covering the anterior pancreas (front to back) and the splenorenal and gastrosplenic ligaments and epiploic foramen (side to side). In cases of posterior gastric wall perforation or inflammation or trauma to the pancreas, fluid or a pseudocyst may be identified in this space (
Fig. 5-9).