Localization: It is most commonly localized in the long bones, femur, tibia, and humerus. It prevails in the metaphyses and metaepiphyses, although a purely diaphyseal location may be seen. There is prevalence for the distal femur and proximal tibia, but not as pronounced as it is in OS.
Clinical: Pain and swelling usually of short duration. Pathologic fracture is common.
Imaging: It is a purely osteolytic tumor, centrally or eccentrically located. Osteolysis may be uniform with geographic ill-defined borders. Sometimes scattered or confluent radiolucent areas give a moth-eaten appearance. Infrequently some osteosclerosis is present at the margins of the tumor. The cortex is usually permeated or destroyed by the tumor. Periosteal reaction is not frequent. As in all purely osteolytic tumors, tumor extension in bone and in the surrounding soft tissues is often more pronounced than radiographs indicate. CT, MRI, isotope scan, and angiography, as well as gross and microscopic study, will show the real extension.
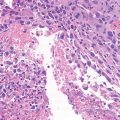
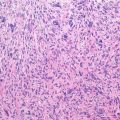
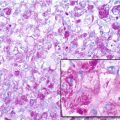
Histopathology: UPS usually breaches the cortex and extends to soft tissues. The tumor is soft, parenchymatous or encephaloid, with frequent yellowish or tan areas. It may appear more firm and whitish with frequent zones of necrosis or hemorrhage. The margins of the tumor show permeation both in bone and soft tissue. UPS is usually a pleomorphic, high-grade malignancy, with storiform pattern. Large and roundish histiocyte-like cells may be sometimes more spindle, with increasing collagenogenesis. In these fibroblastic areas, the storiform pattern is more evident. Cells have an extensive cytoplasm and are deeply stained, eosinophilic, or granular to foamy and thus clearer. Their nuclei are also large, round, or oval, with a thick nuclear membrane, chromatin lumps, and a prominent nucleolus. Some cells may have monstrous, multiple nuclei. Atypical mitoses are usually abundant. Benign sparse giant cells may be seen. The “fibrous” differentiation associates with a “normalizing” effect on cells, so that cells may be sparse, with small nuclei, and only subtle signs of anaplasia. Permeative patterns and coexistence of more cellular and anaplastic areas however will allow diagnosis. UPS of bone is frequently secondary (bone infarcts, old chondromas and chondrosarcomas, radiated bone, Paget, giant-cell tumor, osteomyelitis).
Course and Stage: Most UPS are stage II-B, occasionally stage II-A. As compared to OS, UPS has a higher tendency to multifocal involvement and to bone mets.
Treatment and Prognosis: UPS moderately responds to chemotherapy. After preoperative chemotherapy, the same used for OS, the percentage of good responders (necrosis >90 %) is less than in OS, but higher to that of fibrosarcoma. Postoperative chemotherapy is also indicated with the same schedules used for OS. With this aggressive treatment, the percentage of long-term survivors seems to be similar to that obtained in OS, around 60–70 %. UPS is also relatively responsive to radiation therapy, which can be used rarely as adjuvant to surgery or in inoperable cases.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree