Case presentation
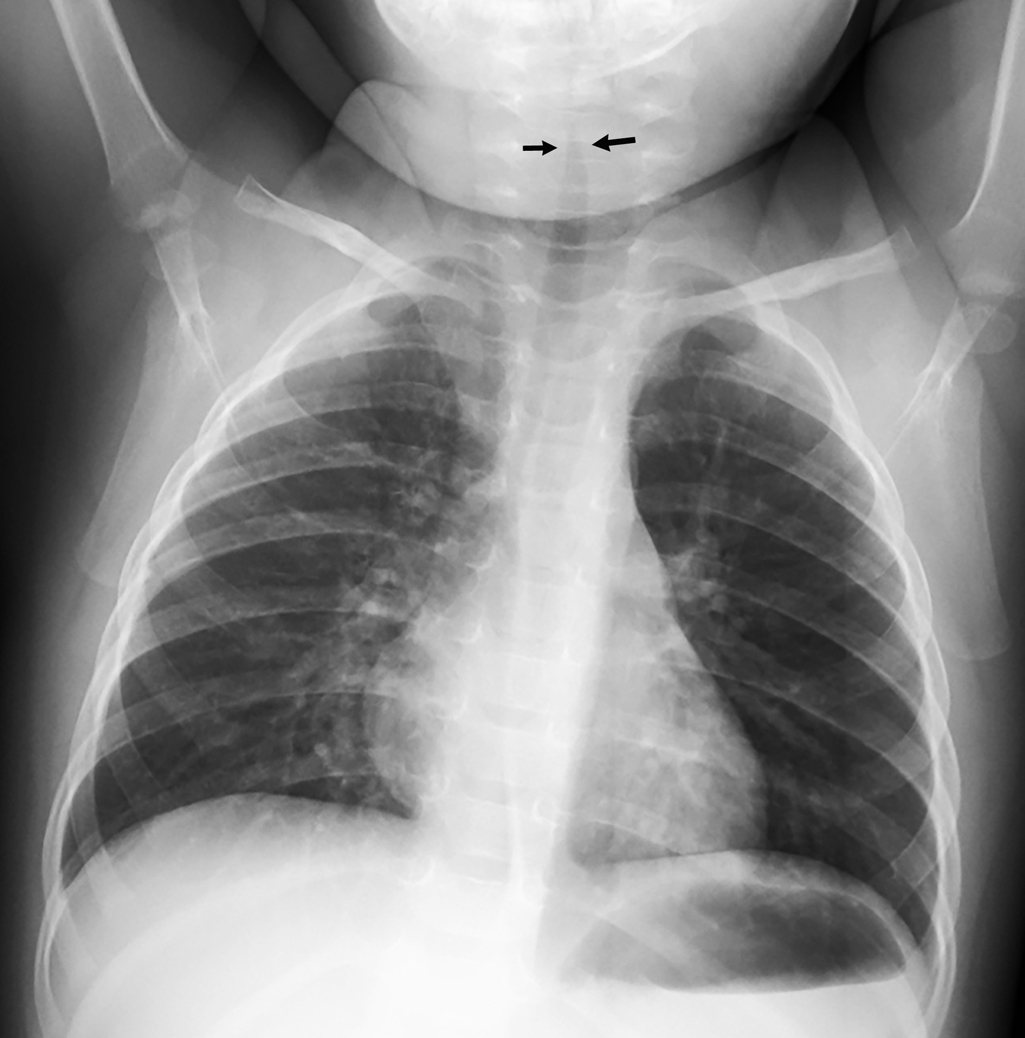
A 14-month-old, previously healthy child presents to the Emergency Department in the middle of the night with respiratory distress, hoarseness, and a barky cough. He has had mild congestion and a low-grade fever for a day. On physical examination, the child is in moderate respiratory distress and is anxious appearing while struggling to inhale each breath. His respiratory rate is 58 breaths per minute, his pulse oxygenation saturation is 98% on room air, and he has prominent subcostal and suprasternal retractions. He is not febrile. On auscultation, he has stridor, but no wheezing or rales in all lung fields, and breath sounds are equal throughout. The child is looking around anxiously without neck movement restrictions or drooling. The parents are concerned that the child “choked on something” since the child’s respiratory distress was so acute in onset. They were seen at an urgent care facility just prior to arrival and had plain chest radiographs performed, which they have provided for review.
Imaging considerations
Plain radiography
Croup is a clinical diagnosis, and radiographs are not commonly indicated. However, the “steeple sign” is the typical finding on an anterior-posterior (AP) view of the chest or a soft tissue neck radiograph. Also called the “wine bottle sign,” it is a description of the appearance of the tracheal narrowing in the subglottic area. The lateral radiograph may demonstrate narrowing and haziness of the subglottic trachea with overdistention of the hypopharynx. If plain radiography is utilized to diagnose suspected croup, a lateral view should be obtained, since epiglottitis has a similar appearance to croup on the AP view. Dedicated soft tissue neck radiographs are useful for this purpose and can provide greater detail.
Advantages of plain radiography include relatively low exposure to ionizing radiation, rapidity, and availability, but imaging should be performed only if the diagnosis of croup is in question or a patient is not responsive to appropriate management for croup. Radiographic findings suggestive of other conditions include swelling of the epiglottis, a foreign body, an asymmetric compromise of the airway, an irregular or edematous trachea, and tracheal compression or deviation. If there is concern for a nonradiopaque foreign body, a more serious infectious process (such as tracheitis, or an oropharyngeal or retropharyngeal abscess), or an anatomic issue (such as a vascular ring or sling), then advanced imaging modalities may be indicated.
Computed tomography (CT)
This imaging modality may be utilized if alternative diagnoses that may present in a manner similar to croup are being considered. These include foreign body ingestion/aspiration, tracheitis, anatomic variants (such as a vascular ring/sling), an airway hemangioma, or conditions causing tracheal compression, such as masses. CT is not otherwise routinely indicated or used.
Magnetic resonance imaging (MRI)
Similar to CT, MRI is utilized as a secondary or tertiary imaging modality in patients who are suspected to have an alternative diagnosis that requires advanced imaging. This may be the case with anatomic variants or masses.
Ultrasound (US)
This imaging test may also be useful to detect etiologies that may mimic the clinical symptoms of croup, in particular, swallowed foreign bodies. The lack of ionizing radiation, availability, and portability of this modality make it particularly attractive in the urgent or emergent setting. However, US is operator dependent and has limited application for infectious cases or patients with complex vascular anatomy that may be causing croup-like symptoms.
Imaging findings
Two-view radiography of the chest is provided. The lungs demonstrate normal volume without evidence of infiltrate, atelectasis, or air trapping. The heart appears normal. There is mild subglottic narrowing ( Figs. 81.1 and 81.2 ). An illustration comparing the normal radiographic appearance of the subglottic airway to the appearance of the subglottic airway in croup is shown in Fig. 81.3 . A different patient, a 4-year-old with findings of croup shown on dedicated soft tissue views of the neck, is presented in Fig 81.4 .