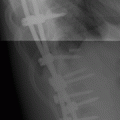
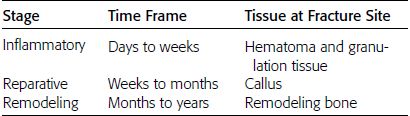
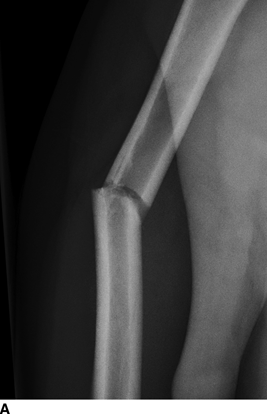
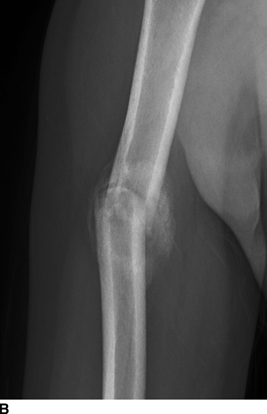
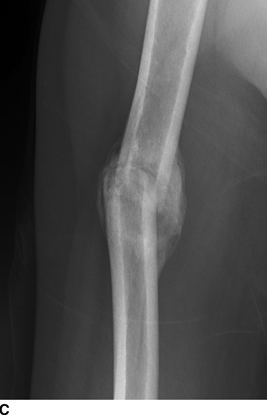
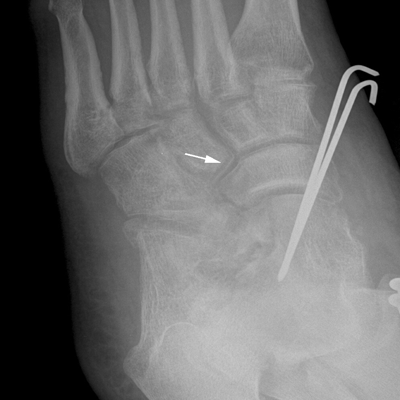
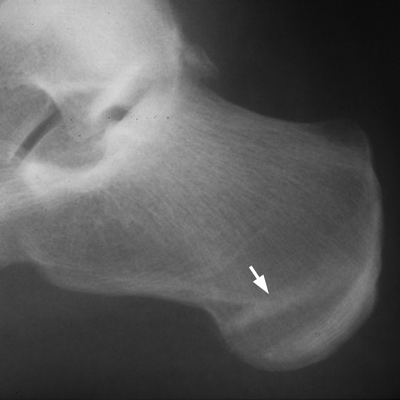
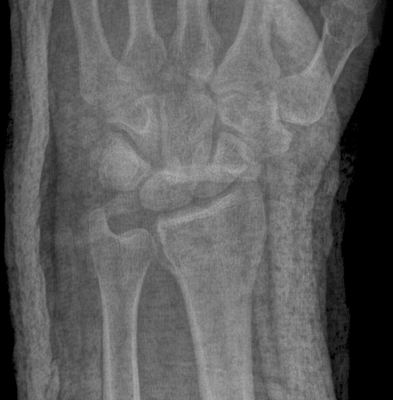
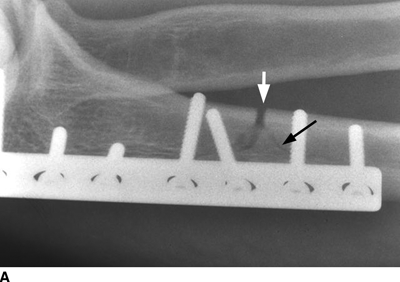
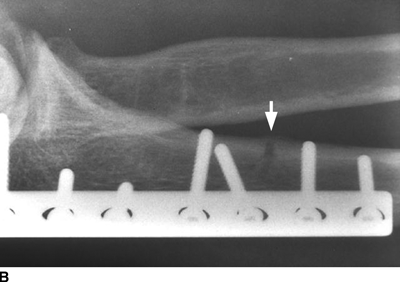
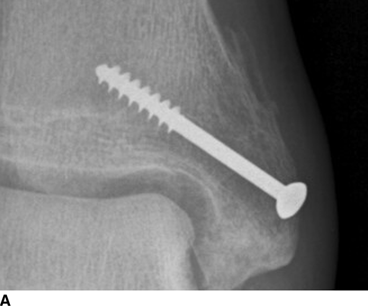
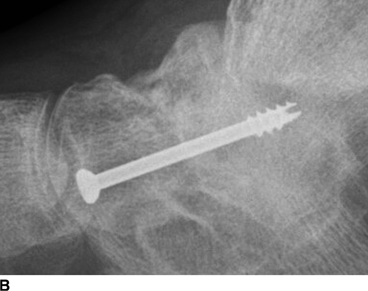
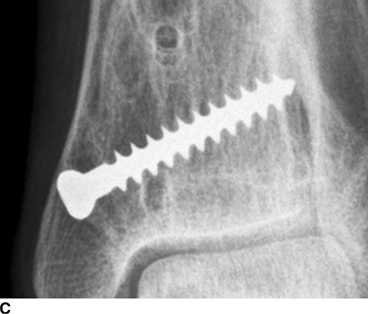
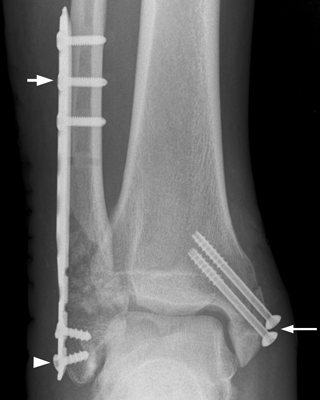
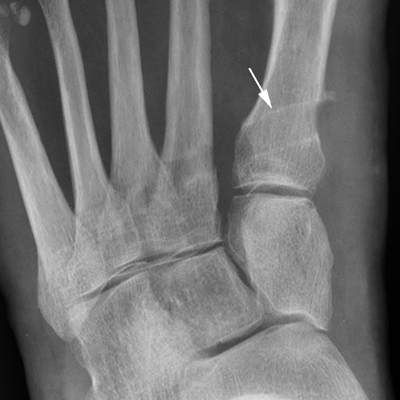
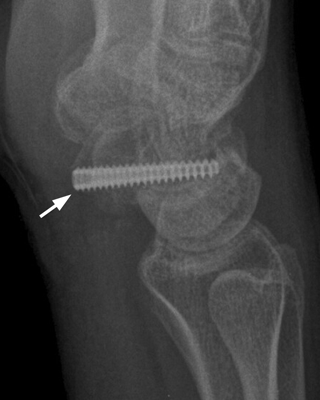
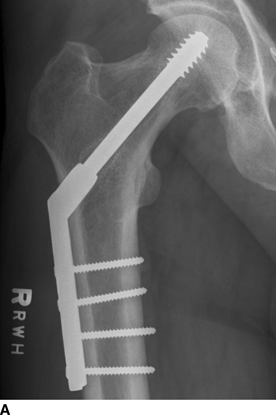
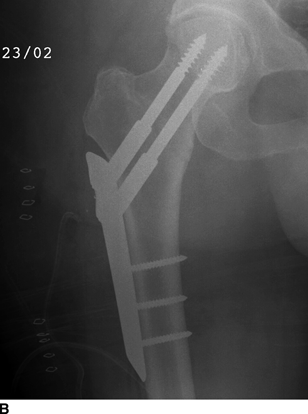
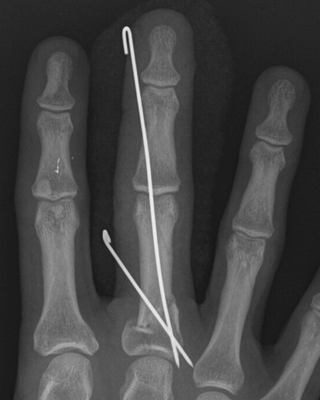
CHAPTER 6 The seriousness of an injury is not always related to the radiographic severity of the fracture. The patient’s general state of health, associated injuries and conditions, degree of soft-tissue injury, and consistency of underlying bone can have a vast influence on outcome. For example, a minimally displaced, closed femur fracture in a frail, osteoporotic woman is often life threatening, whereas a comminuted, displaced femoral fracture in an otherwise healthy child probably is not. In choosing the mode of fracture treatment, considerations other than the location and morphology of the fracture are crucial. The natural history of an uncomplicated long-bone fracture is union through the formation of callus. This secondary fracture healing occurs in three stages: an inflammatory stage, a reparative stage, and a remodeling stage (Table 6.1 and Fig. 6.1). Immediately after the fracture, hematoma and devitalization of soft tissues and bone at the fracture site provoke an acute, intense inflammatory reaction. On radiographs, soft-tissue swelling and sharp fracture lines are present. By 10 to 14 days after injury, the fracture lines may have become more readily visible because of bone resorption. Acute regional osteoporosis of the involved extremity, caused by the hyperemia that accompanies inflammation, is usual (Fig. 6.2). As the hematoma organizes into granulation tissue capable of osteogenesis, the reparative phase begins. External periosteal callus is formed in the subperiosteal regions adjacent to the fracture. Fibrous tissue, cartilage, and immature bone form within the mass of granulation tissue around the fracture. This mass, called primary or soft callus, is fusiform in shape and bridges the fracture gap. In the proper environment of ample blood supply and limited motion and stress, the primary callus forms bone. Ossification in primary callus may be seen on radiographs as early as 10 days after injury in children and 2 weeks in adults. Because external callus expands the diameter of the bone at the site of fracture healing, often by a factor of 2 or 3, mechanical stability (clinical union) is generally achieved within 6 to 12 weeks. Radiographs should show abundant, well-defined callus bridging the fracture site, with fracture lines becoming fuzzy. Bone repair continues with the formation of intramedullary (IM) callus and the eventual remodeling of woven bone to lamellar bone along the lines of stress. Remodeling of callus may take place over a period of months to years. In time, there may be scant radiographic indication of the previous fracture. By contrast, fractures of cancellous bone, particularly if impacted, tend to form internal callus rather than external callus as they heal. Healing in a fracture that is wholly confined to cancellous trabeculae may be evident radiographically only as increasing and then decreasing sclerosis at the fracture site (Fig. 6.3). TABLE 6.1 Stages of Fracture Healing FIGURE 6.1. Fracture healing of cortical bone without fixation in an adult. A: Acute fracture of the humeral shaft. B: At 6 weeks, calcified callus is visible and the fracture lines are becoming obscured. C: At 12 weeks, the fracture has almost completely healed. FIGURE 6.2. Acute osteoporosis accompanying fracture healing. Radiograph 6 weeks after injury shows subchondral bone resorption (arrow). FIGURE 6.3. Sclerosis (arrow) indicates healing fracture in the cancellous bone of the calcaneus. Injuries of the soft tissues heal through the process of localized necrosis, inflammation, and repair. Ligament and tendon injuries heal with a bridging scar if the ends are not too far distracted. The scar may eventually remodel along the lines of stress. Cartilage heals through a different process because of the lack of vascularization. Localized necrosis occurs, but there is no inflammatory phase. Superficial injuries that do not extend to the bone marrow heal by migration of cells from the synovial fluid or from elsewhere in the cartilage. In injuries that extend to the bone marrow, an initial blood clot is replaced by granulation tissue. The resulting fibrous scar undergoes progressive hyalinization and chondrification to become fibrocartilage. The vast majority of fractures are treated closed, that is, without open surgery. The fractures in soft tissues are reduced, and the fracture is stabilized but not completely immobilized. Muscle activity, joint motion, and load transmission promote external callus formation. The two common methods of closed fracture treatment are casts and traction. Casts can be used to reduce and control fractures with angular deformity through three-point fixation. The cast is shaped so that it pushes at the apex of the fracture and at the opposite ends of the bone, tending to keep it straight. Slow-setting plaster of Paris (Fig. 6.4) is applied while reduction maneuvers are performed. Casts are typically applied over a stockinette and a layer of padding so that a radiolucent zone is present between the limb and the cast on radiographs. A second layer of cast material can be applied to provide strength and durability. Plaster casts are often covered with a layer of fiberglass for durability and may be replaced completely by fiberglass as the fracture begins to heal and the patient regains the use of the limb (Fig. 6.5). Fiberglass casts can be made into more functional braces through the addition of hinges where the cast crosses a joint. Some fractures of the thoracic and lumbar spine are treated with casts or braces that envelop the torso and stabilize the spine by compressing the soft tissues of the abdomen. The position and alignment of reduced fractures of the limbs can be maintained in a similar manner. The shape and relative rigidity of the cast use the patient’s own soft tissues to turn the cast into a fluid-filled cylinder that resists swelling and deformation. Stable fractures, when subjected to normal stresses, maintain their reduction. External supports such as casts, splints, or braces are load-sharing devices that restrict motion after a stable fracture has been reduced. Traction can be applied and maintained in a variety of ways. Skin traction, in which the limb is gripped with adhesive bandages and connected to a system of hanging weights, is seldom used except for femoral fractures in small children. Skeletal traction is applied by placing pins into the extremity distal to the fracture and connecting the pins to weights. Dynamic traction allows the physiologic motion that is generally beneficial to the formation of periosteal callus. Traction on fractures of the clavicle and proximal humerus can be applied with a figure-of-eight harness and a long-arm cast, respectively. The upper limb itself becomes the hanging weight, and the direction of traction depends on the point of suspension along the cast. Some fractures of the cervical spine are treated with a halo brace that functions on the same principle but works against gravity by stretching the neck. FIGURE 6.4. Plaster cast applied to distal radius fracture. FIGURE 6.5. Fiberglass cast applied to distal radius fracture. Open reduction and internal fixation (osteosynthesis) requires surgical exposure of the fracture. The fracture is reduced, the soft tissues are repaired, and the fragments are fixed with hardware. If a bone undergoes plastic deformation before fracturing, the fracture fragments may not fit back together because of the distortion in shape that preceded the fracture. Fracture fixation hardware does not substitute for the native bony structure; rather, it provides temporary mechanical stability while the natural healing process occurs. The stability that comes with internal fixation is crucial to rapid restoration of mobility and function; many patients cannot tolerate bed rest and prolonged hospitalization. Fixation devices include screws, plates, rods, pins, nails, and wires. Many fixation devices can be inserted percutaneously under fluoroscopic guidance or through minimal incisions. A second operation is necessary to remove many types of hardware after the fractures have healed. Internal fixation that holds bone fragments together rigidly promotes direct bony union (primary fracture healing). New intracortical haversian systems drill across the fracture site, leaving cores of new bone. Fracture callus is minimal or absent as the osteocytes remodel the fracture away (Fig. 6.6). On radiographs, primary fracture healing is seen as a gradual disappearance of the fracture line. A gap between fragments or excessive motion at the fracture site interferes with the migration of osteocytes across the fracture plane, and the fracture heals through the formation of periosteal and endosteal callus. Secondary fracture healing occurs more slowly in fractures with internal fixation because restriction of motion interferes with formation of callus. FIGURE 6.6. Healing internally fixed transverse fracture of the ulna with posterior butterfly fragment. A: Immediate postoperative film shows a cortical plate has fixed the fragments of the transverse portion of the fracture with 1 to 2 mm distraction (short arrow) while the oblique fractures are compressed (black arrow). B: After 7 weeks, endosteal callus bridges the transverse fracture (arrow) and the oblique fractures have remodeled and disappeared. Internal fixation devices are designed to function on the biomechanical principles of static or dynamic interfragmentary compression, bridging, or splintage. In static compression, a metal implant holds the fracture fragments together under compression. In dynamic compression, the implant transforms physiologic loading into compression at the fracture site. There is direct bony union in both types of compression. Internal fixation bridges a fracture site when it is secured to uninjured bone on either side of the fracture. Physiologic loads are transferred from the bone on one side of the fracture to the bone on the other side. If the fragments are not directly apposed and there is motion between them, periosteal and endosteal callus fills the gaps between the bones. Length and alignment are maintained while the bones heal. Internal fixation devices that function as internal splints allow motion at the fracture site and promote periosteal callus while maintaining reduction. Orthopedic screws are available in a variety of sizes and shapes, often for use in specific circumstances (Fig. 6.7). The parts of a screw are the head, shaft, thread, and tip. Most types of screws have a head socketed to receive a hexagonal shaft driver and a threaded shank. The heads have a hemispheric undersurface that allows contact even when the screw is inclined. Screws used for cancellous bone have a wider thread diameter relative to the core shank diameter and a deeper thread pitch (larger distance between threads) than screws used for cortical bone (Fig. 6.8). Most screws are inserted into drill holes. These holes may be tapped or threaded to receive a screw, or the screw may be self-tapping and cut its own threads as it is driven into the hole. Cannulated screws are hollow in the center. These allow the placement of screws over a guide wire, improving the ability of the orthopedist to place screws accurately without the need for supplementary clamp fixation of the site. Some cannulated screws are self-drilling and self-tapping and can be percutaneously inserted over a guide wire. Screws are made of metal, commonly stainless steel or titanium alloy. Bioabsorbable screws and other nonmetallic orthopedic implants for fracture fixation may be difficult to recognize on radiographs, but have markedly decreased artifacts on MRI (Fig. 6.9). FIGURE 6.7. Common types of orthopedic screws. A: Compression or lag screw. B: Cannulated compression screw. C: Fully threaded screw with cancellous threads. D: Fully threaded screws with cortical threads. FIGURE 6.8. Ankle fracture with internal fixation. Two cannulated lag screws (long arrow) with cancellous threads fix the medial malleolus. The cortical plate is fixed to the fibular shaft by three screws (short arrow) with cortical threads, and to the lateral malleolus by two cancellous screws (arrowhead). FIGURE 6.9. Bioabsorbable screw. Radiograph of the foot shows lucency indicating drill hole for bioabsorbable screw fixing first and second metatarsals (arrow). When screws are used to secure bony fragments to each other, they are called interfragmentary screws. Interfragmentary screws work biomechanically by converting torque applied to the screw into axial tension between the bone fragments. When screws are used to secure cortical plates or other hardware to bone, they are called position screws or neutralization screws. Headless screws are used where the presence of a head may interfere with motion or cause soft-tissue irritation. Headless screws may be inserted below the surface of the bone, which is desirable in osteochondral fractures and intra-articular fractures. Screws with heads may also be inserted flush with the bone surface by countersinking or drilling a larger hole for the head to drop into as the screw is driven. Compression screws, also called lag screws, are threaded only at the distal portion of the shank. This type of screw compresses two objects together (bone against bone or bone against another fixation device). The object into which the screw is threaded is pulled against the object through which the screw is passed. Maximal compression is obtained when the screw is oriented perpendicular to the fracture plane. A fully threaded screw fixes objects together without compressing them because the threads force them to maintain their relative positions. Screws that are fully threaded along their shanks may also be used in compression if the drill hole near the head (the glide hole) is drilled to a size that the threads pass through freely. Subsequent extraction of screws is easier if they are fully threaded. The Acutrak screw is a headless, fully threaded, cannulated screw with a tapered profile and a variable thread pitch (Fig. 6.10). The thread pitch is wider at one end of the screw, so that each turn of the screw compresses fragments together because of the difference in thread pitch. These screws are commonly used for internal fixation of intra-articular fractures of small bones such as the scaphoid. Were it not for the cost, they could be exceedingly useful in cabinetmaking. FIGURE 6.10. Headless, tapered, variable thread pitch compression screw (arrow) fixing scaphoid waist fracture. Dynamic hip screws (telescoping hip screw, sliding hip screw) (Fig. 6.11) and dynamic condylar screws with side-plates are designed for dynamic compression of fractures of the proximal and distal femur, respectively. The screw fits into a sleeve in the side-plate into which it can slide or telescope. In an intertrochanteric hip fracture, for example, the screw extends through the femoral neck into the head, and the side-plate is fixed to the lateral cortex of the proximal shaft. With weight bearing, the unthreaded shank of the screw slides into the sleeve at the end of the side-plate, compressing the fracture fragments together. A smaller set screw that is threaded into the near end of the large-diameter sliding screw can be used to apply static compression to the fracture site at the time of surgery. FIGURE 6.11. Fixation for intertrochanteric fractures. A: Telescoping (dynamic) hip screw fixing an intertrochanteric fracture. B: Percutaneous compression plate fixing an intertrochanteric fracture. Note the small size of the skin incisions, as indicated by the skin staples. Kirschner wires (K-wires) are used to fix cancellous bone in situations in which a screw might also be suitable. They are introduced percutaneously, and their purchase in bone is exclusively by friction (Fig. 6.12), which makes them easier to pull out than screws. The end of the wire is typically left protruding from the skin so that the wires can be extracted when the fracture heals. FIGURE 6.12. K-wire fixation. Radiograph of hand shows two K-wires fixing a fracture of the proximal phalanx of the middle finger. A tension band transforms tensile stress into interfragmentary compression (Fig. 6.13). Tension bands are commonly used where asymmetric muscle tension tends to distract fragments. The tension band is usually a wire loop or figure-of-eight that is placed across the fracture site along the line of tensile force. When the muscle contracts, the tension band acts like a hinge to compress the fracture fragments together. For example, a transverse fracture of the olecranon process could be fixed by a tension band along the posterior aspect of the triceps mechanism. With contraction of the triceps muscles, the tension band functions as a hinge and converts the distractive force along the posterior aspect of the olecranon to compressive force on the opposite side (Fig. 6.14). Tension bands are also commonly used to fix transverse fractures of the patella. FIGURE 6.13. Biomechanical concept of tension band fixation. The band acts as a hinge, transforming tension on the olecranon into interfragmentary compression.
Imaging of Fracture Treatment and Healing

 FRACTURE HEALING
FRACTURE HEALING
 CLOSED FRACTURE TREATMENT
CLOSED FRACTURE TREATMENT
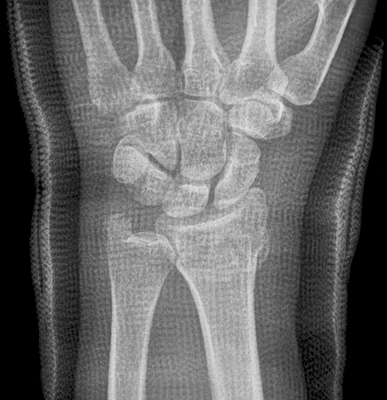
 OPEN REDUCTION AND INTERNAL FIXATION
OPEN REDUCTION AND INTERNAL FIXATION
 SCREWS
SCREWS

 WIRES AND CABLES
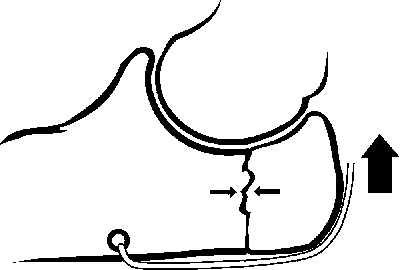
WIRES AND CABLES
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree