, Carlos Capuñay1, Carlos E. Sueldo2 and Juan Mariano Baronio3
(1)
Diagnóstico Maipú, Buenos Aires, Argentina
(2)
University of California, San Francisco, CA, USA
(3)
CEGYR, Buenos Aires, Argentina
One of the distinct characteristics of the virtual studies is the possibility of obtaining images of the pelvic structures, with sufficient quality so as to be evaluated. Because it is an exam done through computed tomography, it possesses all the diagnostic capacity that derives from this method, allowing the observation of lesions located in other organs and structures. In this way, the extra-uterine findings constitute an unavoidable part of the virtual hysterosalpingography (VHSG).
The implication of the incidental findings was shown in other areas like in virtual colonoscopy [1–3]. In these cases the exam can be utilized as a screening method, allowing the detection of pathologies in a pre-clinical state, leading to an early diagnosis and treatment of some previously unknown conditions in asymptomatic patients. This particular situation is benefited because in the ethereal group of the population in study, in general over 50 years old, the prevalence of chronic pathologies is higher than usual [4, 5]. On the other hand, in patients with fertility problems and 35 year-old in average, the prevalence of extra-uterine pathology is lower.
Besides, one must take into account that the diagnosis of an unexpected finding has a potential impact on different levels. A report with an unexpected finding usually produces a certain level of anxiety, which can be excessive in some patients. The economic impact generated by the complementary exams and treatments that derive from the incidental finding of these lesions must also be taken into account, as well as a possible increase in the morbid-mortality risk if the patient is subjected to invasive procedures [6, 7].
Classification
Similar to the extra colonic findings in virtual colonoscopy studies [8], the incidental diagnosis in VHSG can be classified according to its clinical importance: high, moderate and low.
(i)
Findings of high clinical importance:
They are those which require an immediate intervention or the carrying out of other complementary exams. The following have been reported within this group: pelvic limphadenopathies, suspicious ovarian masses, complicated colonic diverticula, pelvic collections, fistulas, and suspicious lytic or blastic bone lesions (Fig. 11.1).
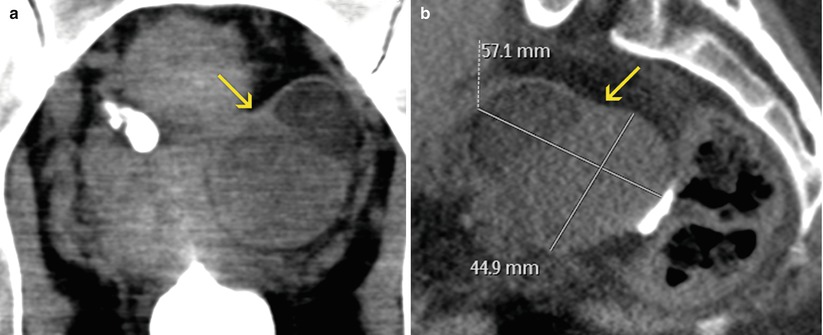

Fig. 11.1
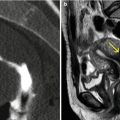
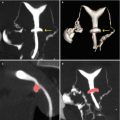
Findings of high clinical importance. (a, b) Coronal and sagittal VHSG images with soft tissue window. An ovoid lesion can be observed in the left adnexal region (arrow) with heterogeneous density and internal septa, suggesting a suspicious malignant ovarian mass. It requires continuing diagnostic algorithm for its classification
(ii)
Findings of moderate clinical importance:
They are generally benign and their re-evaluation can be deferred. Reported in this group are: undetermined adnexal masses, inguinal hernias, non complicated colonic diverticula and undetermined bone lesions (Fig. 11.2).
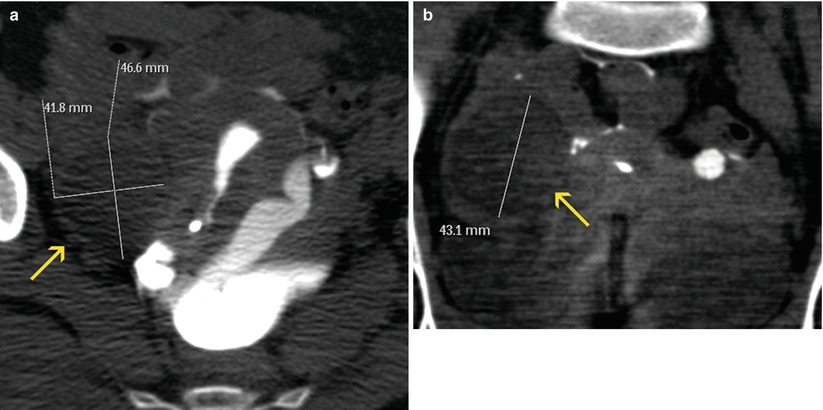

Fig. 11.2
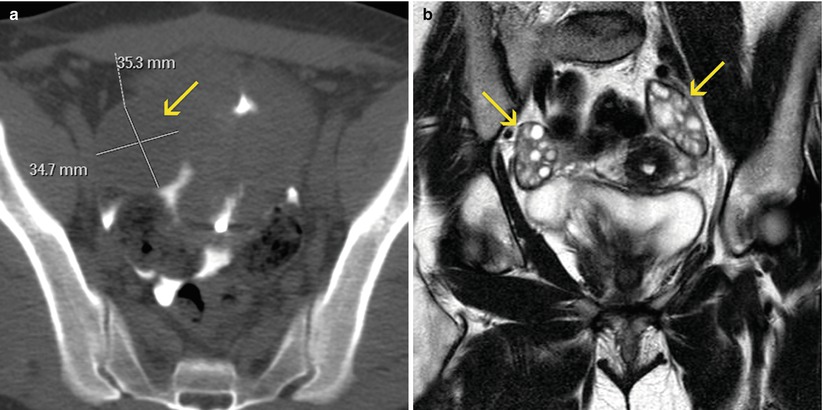
Findings of moderate clinical importance. (a, b) Axial and coronal VHSG images with soft tissue window. An ovoid lesion larger than 4 cm (arrows) can be observed in the right adnexal region, with well defined walls and homogeneous low density. As an undetermined ovarian mass, requires a differed evaluation with a specific method
(iii)
Findings of low clinical importance:
They are the ones that do not require another type of analysis or treatment. The most frequent benign lesions are: ovarian cysts and teratomas, vascular calcifications, sacral perirradicular cysts and degenerative bone lesions (Fig. 11.3).
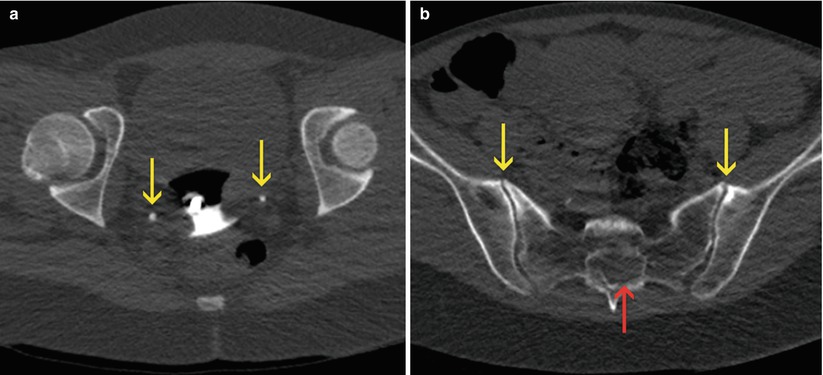

Fig. 11.3
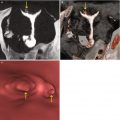
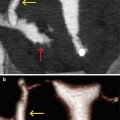
Findings of low clinical importance. (a) Axial VHSG image showing two focal images with calcium density (arrows) in the lower region of the pelvic cavity, corresponding to vascular calcifications (phleboliths) and should not be confused with urinary stones. (b) Axial VHSG image showing deformity in the sacral spinal canal due to the presence of a periradicular cyst (red arrow) and degenerative sclerosis in the anterior region of the sacroiliac joints (yellow arrows)
Incidence and Valorization of Extra-Uterine Findings
The report of the unexpected lesions is of great responsibility for the radiologist because the next steps to follow depend on its valuation. On the other hand, the referral physician must know the reaches of the method requested and be ready to face the results comprehensively. It is imperative to consider at this point the importance of the extra time the radiologist puts into the exploration of the rest of the soft and bone pelvis. It is necessary to analyze the acquired axial images in their totality and give them a different treatment than the uterine evaluation.
As mentioned before, the frequency of these incidental lesions is low due to the fact that most of the patients are young, asymptomatic and are in a study for infertility. The unexpected findings of low clinical significance represent a large part of the reports, and generally do not require complementary exams to clarify their diagnosis. The lesions of moderate importance are usually doubtful or undetermined diagnoses, hence the anxiety produced by the uncertainty. In these cases a re-evaluation is vital, and its following depends on each particular case. One example is the unspecific bone lesions, that require new short term imaging studies. The potentially important findings are extremely rare in this group of patients. These are the ones that can affect the health of the patient. Despite their infrequency, one must always be watchful and ready for these findings due to their high impact on morbi-mortality.
Ovarian Pathology
Both functional as well as structural abnormalities affect the ovaries and can be the cause of infertility. For the fecundation to be a success, it is necessary that the ovulation process and follicular development be normal [9]. The study which evaluates these functional parameters, as well as the structural anatomic characteristics, is ultrasound [10]. The conventional hysterosalpingography studies can only infer the existence of an abnormality in the ovary size when displacement and compression is observed in the adjacent uterine tube [11]. Nevertheless, these findings are not specific, because the tubes have a variable position and because other processes can generate a mass effect of the ovaries. On the other hand, in VHSG exams, one can correctly individualize the ovaries, measure their size, and evaluate their density and position in order to characterize pathologic processes (Fig. 11.4). The instilled contrast material which passes to the peritoneal cavity helps delineate the ovaries outline. One disadvantage is associated to the lack of intravenous contrast which is fundamental to detect solid areas and pathologic signs.
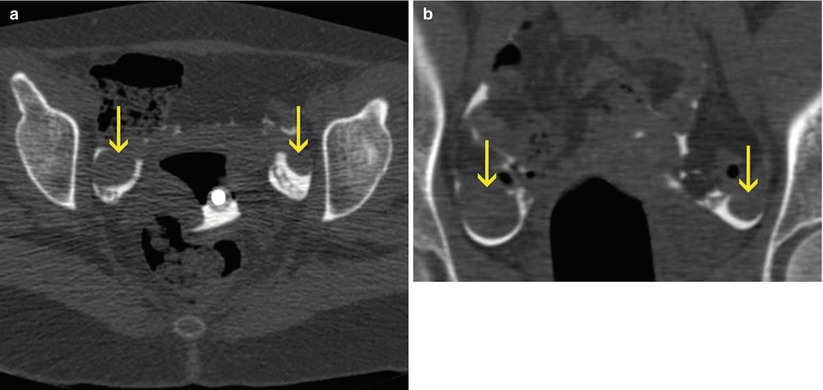

Fig. 11.4
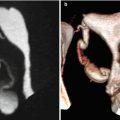
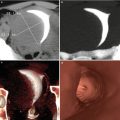
Normal ovaries. (a, b) Axial and coronal VHSG images where both ovaries of normal size and morphology can be observed (arrows) surrounded by contrast material in the peritoneal cavity
The polycystic ovary syndrome is the structural abnormality that most frequently causes infertility [9]. The ovary is enlarged and multiple cysts of different sizes are distinguished in its interior (Fig. 11.5). There exist cases where a complicated cyst can be found, with a high density content that suggests hematologic remains, frequent in endometriosis cases (Fig. 11.6). Another finding difficult to diagnose are mature cystic ovarian teratomas. They are round or ovoid masses of different dimensions that characteristically present a heterogeneous density, predominantly fat, alternated with solid and calcium areas (Fig. 11.7). When the ovarian masses are not typically benign, a complementary evaluation is required for its improved characterization. The parameters that suggest a malignity are: an ovarian size larger than 4 cm, mixed internal structure (solid-cystic), parietal or septal thickening, and the presence of associated swollen lymph nodes or ascites [12, 13] (Fig. 11.8).