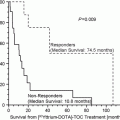
Fig. 1
Sodium iodide symporter
Several anions are transported by NIS, namely, I, SeCN, SCN, ClO3, and NO3 (in descending order of affinity). NIS also transports technetium pertechnetate and rhenium perrhenate. The only apparent common denominator of these transportable substrates is anionic monovalency and a monovalent anion size close to that of iodide (Eskandari et al. 1997). In addition, the specificity of sodium-dependent co-transporters for the sodium ion is not absolute, for example, Li+ can drive iodide transport at a reduced level (10–20 % of Na-driven transport level) (Eskandari et al. 1997). However, iodide transport through NIS is not driven by H+ (acidification).
3.3 Regulation
3.3.1 Thyroid-Stimulating Hormone
Many studies, in different experimental models, have demonstrated that thyroid-stimulating hormone (TSH) and the activation of the cyclic adenosine monophosphate (cAMP) pathway are the principal regulators of iodide uptake (Filetti et al. 1999). TSH increases radioiodine uptake in thyroid cancer cells and in normal thyrocytes, as evidenced by radioiodine whole-body scans. Furthermore, the upregulations of NIS mRNA and protein are known to be mediated by the cAMP pathway in rodent cell lines, a Fisher rat thyroid cell line (FRTL-5 cells) (Weiss et al. 1984), in PC Cl3 immortalized rat thyroid cells (Trapasso et al. 1999), and in human primary thyroid cells (Kogai et al. 2000a, b).
This upregulation of NIS by TSH occurs at the transcriptional and posttranslational levels. In fact, TSH activates NIS promoter and NIS upstream enhancer (Endo et al. 1997; Ohmori et al. 1998), increases the half-life of NIS protein, and stimulates the trafficking of NIS to the plasma membrane (Riedel et al. 2001). Furthermore, several observations suggest that other mechanisms, including cAMP-dependent phosphorylation and the participations of other activating or inhibitory proteins, are involved in the posttranslational regulation of NIS activity.
3.3.2 Iodine Intake
Treatment with small to moderate amounts of iodide does not influence the uptake of simultaneously administered I-131 by the thyroid, but larger doses progressively inhibit organic binding, which is referred to as the acute Wolff–Chaikoff effect. Furthermore, in vivo studies have shown that iodide inhibits the expressions of thyroid peroxidase (TPO) and NIS mRNAs in the dog thyroid (Uyttersprot et al. 1997). However, when a high serum iodide concentration (100–200 ug/dL) is maintained by repeated iodide administration, this inhibitory effect disappears and thyroid iodine organification increases. Not surprisingly, this is referred to as escape from the Wolff–Chaikoff effect, and it has been suggested that it is caused by a decrease in NIS, which lowers intrathyroidal iodine content below a critical inhibitory threshold, and thus allows iodide organification to resume (Eng et al. 1999).
3.3.3 Cytokines
Interleukin-1 (IL-1), tumor necrosis factor, and interferon all inhibit TSH-stimulated hNIS gene expression and iodide uptake in thyrocyte cultures (Riesco-Eizaguirre and Santisteban 2006), which suggests that iodide uptake inhibition by these cytokines is mediated, at least in part, by the downregulation of NIS gene expression. Furthermore, tumor necrosis factor, interferon-gamma, IL-1a, IL-1b, and IL-6 have been shown to inhibit NIS mRNA expression and iodide uptake activity in FRTL-5 and human thyroid cells (Ajjan et al. 1998a, b; Pekari and Hersam 1998). These entities are produced by inflammatory infiltrates and thyroid follicular cells in autoimmune thyroid disease, and thus, they could participate in autoimmune hypothyroidism by downregulating hNIS mRNA expression. Similar mechanisms could also contribute to the thyroid abnormalities associated with subacute thyroiditis and nonthyroidal illness (Ajjan et al. 1998a, b), which is consistent with irregular reductions in radioiodine uptake in thyroiditis on thyroid scans.
3.3.4 Transcription Factors
3.3.5 Glycosylation and Phosphorylation of NIS Protein
It has been proposed that NIS glycosylation and phosphorylation contribute to the regulation of NIS trafficking to the membrane (Dohan et al. 2005). The cytoplasmic carboxyl-terminal domain of NIS contains a PDZ target motif and a dileucine motif tail, which are important for protein–protein interactions. Moreover, a recent study reported that the deletion of these motifs prevents iodide transportation and the insertion of NIS protein into the plasma membrane. Accordingly, it appears that these motifs are likely to be involved in the posttranslational regulation of NIS by TSH (Kogai et al. 2006).
When synthesized in low amounts, hNIS does not undergo glycosylation and remains in intracellular compartments (Trouttet-Masson et al. 2004). Moreover, the speed of iodide transport by NIS has been shown to be modulated by the phosphorylation statuses of Ser-43 and Ser-581 (Vadyssirisack et al. 2007), and more generally, phosphorylation is known to affect the functional activities, subcellular localizations, and/or protein stabilities of various channels and transporters.
3.3.6 Others
Thyroglobulin (Tg) acts as a potent suppressor of thyroid-specific genes, and suppresses NIS mRNA levels and iodide uptake activity (Riesco-Eizaguirre and Santisteban 2006). Although it has not been established whether Tg acts directly, the Tg-mediated suppression of NIS may represent a negative feedback autoregulatory mechanism that counterbalances the stimulation of follicular function by TSH (Saito et al. 1998). This is in accord with the immunohistochemical distribution of NIS observed in the normal thyroid, that is, low or null NIS expression is found in larger thyroid follicles that are composed of inactive and flattened epithelial cells. In contrast, larger amounts of Tg are found in smaller follicles that are composed of active cubiodal cells.
Interestingly, estradiol downregulates NIS expression and iodide uptake by FRTL-5 cells, and also downregulates their proliferation, which suggests that estradiol contributes to the higher prevalence of goiter observed in women (Furlanetto et al. 1999).
3.4 The Normal Distribution of NIS
3.4.1 Thyroid Tissue
In normal thyroid tissue, follicular epithelial cells exhibit a heterogeneous pattern when stained with hNIS antibodies. Inside any given follicle, certain follicular cells confined to the basolateral membrane are strongly immunostained, and are quite distinct from weakly stained or unstained cells. Filetti et al. (1999) reported that approximately 30 % of follicular cells express detectable amounts of hNIS protein. On the other hand, the immunostaining pattern of TSH receptor is quite different. In fact, it is constitutionally expressed on all normal follicular cells. Stromal cells, lymphocytes, intrafollicular macrophages, and vascular endothelial cells in normal thyroid tissue are immunonegative for hNIS protein (Caillou et al. 1998).
3.4.2 Nonthyroid Tissue
NIS mRNA is detected in many nonthyroid tissues, including those of the salivary and lacrimal glands, stomach, choroid plexus, ciliary body of the eye, skin, placenta, the lactating mammary gland, and thymus (Riesco-Eizaguirre and Santisteban 2006). Somewhat surprisingly, a large immunostaining survey revealed that the following tissues express NIS; bladder mucosa, endometrial glands, distal and collecting renal tubules, bronchial epithelium, intrahepatic bile canaliculi, gallbladder mucosa cells, prostate epithelium, and pancreatic exocrine cells. Other tissues of the adrenal gland, epididymis, and small bowel have also been found to express NIS, but in a sporadic manner (Wapnir et al. 2003). The above findings concur with observations that radioiodine and Tc-99m pertechnetate are almost always taken up by the salivary glands, stomach, breast, and placenta. Furthermore, observations that radioiodine is secreted in tears and that Tc-99m pertechnetate shows supraorbital uptake in healthy patients suggest that the lacrimal glands actively absorb iodide (Shen et al. 2001).
Salivary glands express hNIS protein, but NIS protein immunostaining is only observed in ductal cells, in which it is diffusely expressed, and not in acinar cells. In the human stomach, NIS expression is restricted to parietal cells (Filetti et al. 1999), whereas in lactating mammary glands NIS is expressed at the basolateral membrane of alveolar epithelial cells. An examination of NIS protein expression at various physiologic stages showed that it is exclusively expressed in the mammary gland during gestation and lactation (Weiss et al. 1984). The expression of NIS in normal mammary tissues appears to be driven by hormonal factors, for example, oxytocin (a hormone released during lactation) induces NIS expression and radioiodine transport, whereas prolactin (a hormone required for milk production) suppresses this effect (Tazebay et al. 2000).
Spitzweg et al. (1998) found that the nucleotide sequences of hNIS cDNA derived from the parotid gland, mammary gland, and gastric mucosa are identical to that of hNIS cDNA derived from the thyroid. However, TSH stimulates radioiodine uptake in thyroid tissues and not in these extrathyroidal tissues, because they do not express TSH receptors. Diminished iodide transport in extrathyroidal tissues may be a result of attenuated NIS gene transcriptional activity, perhaps due to an altered promoter structure or function, or changes in NIS mRNA or protein turnover. Furthermore, thyroid transcription factor 1 may be capable of activating NIS gene expression in the thyroid gland, and thus, could account for the lower levels of NIS mRNA observed in extrathyroidal tissues (Spitzweg et al. 1998).
3.5 Relations Between the NIS Gene and Other Genes
It has been suggested that the expressions of the NIS, thyroglobulin, TSH receptor, and the TPO genes are regulated by distinct molecular mechanisms, or alternatively, that they may respond in different ways to the mechanisms of oncogenic transformation. Trapasso et al. (1999) found similar discrepancies in vitro, namely, that oncogene-transformed rat thyroid cells lack iodine uptake, but express the thyroglobulin, TPO, and TSH receptor genes to variable extents. The regulation of NIS expression at the mRNA level appears to differ from those of other thyroid-specific markers. It may be that the reduced expressions of unidentified nuclear factors reduce NIS expression and that this explains the absence of iodide uptake in some papillary thyroid cancers (Kogai et al. 2001). Magliano et al. (2000) demonstrated that the reintroduction of paired domain transcription factor into PCPy cells was sufficient to activate the expressions of endogenous genes encoding thyroglobulin, TPO, and NIS, which provided direct evidence regarding the ability of paired domain transcription factor to activate the transcriptions of thyroid-specific genes at their chromosomal loci, and strongly suggested that this transcription factor plays a fundamental role in the maintenance of the functional differentiation of thyroid cells.
Furthermore, NIS mRNA expression levels have been shown to be lower in oncogene-transformed PC Cl3 rat thyroid cell lines (PC v-erbA, PC HaMSV, PC v-raf, and PC E1A), which suggests that oncogene activation may be involved in the pathophysiology of reduced NIS expression in thyroid cancer (Trapasso et al. 1999). Different oncogenic pathway activations, for example, of the PyMLV, p53143ala, or ras pathways, may produce the same effect, and the same oncogenic pathway (v-ras Ha, v-ras Ki) may have different effects on the transcriptional regulation of the NIS gene.
Recently, activating mutations have also been reported in BRAF in papillary thyroid carcinoma (Trovisco 2004; Fugazzola et al. 2006). The most frequent alteration found was a T1799A transversion in codon 15 that translates into a V600E amino acid substitution. Interestingly, BRAF-positive papillary thyroid carcinomas are associated with radioiodine scan negativity and the impairment of NIS targeting to the cell membrane as determined by immunostaining (Riesco-Eizaguirre and Santisteban 2006; Riesco-Eizaguirre and Gutierrez-Martinez 2006).
It would appear that further studies on the mechanisms of NIS are likely to provide new information and provide tools that more effectively treat thyroid carcinomas with impaired radioiodine uptake.
4 NIS Expression in Thyroid Cancer
4.1 NIS Expression in Primary Tumors
Available reports vary considerably with respect to the quantitative expression of NIS in tumors. Using RT-PCR (reverse transcription-polymerase chain reaction), Lazar and Park found variable or reduced hNIS mRNA expression in thyroid cancers (Lazar et al. 1999; Park et al. 2000). Arturi et al. (1998) reported that the NIS transcript was present in 73–96 % of patients with differentiated thyroid cancer, and (Saito et al. 1998) reported increased NIS expression in 7 of 17 papillary thyroid cancer patients by immunoblotting and in 8 of 12 papillary cancer patients by immunohistochemistry. Similarly, (Dohan et al. 2001) found that 70 % of their thyroid cancer samples overexpressed NIS versus normal surrounding tissues.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree