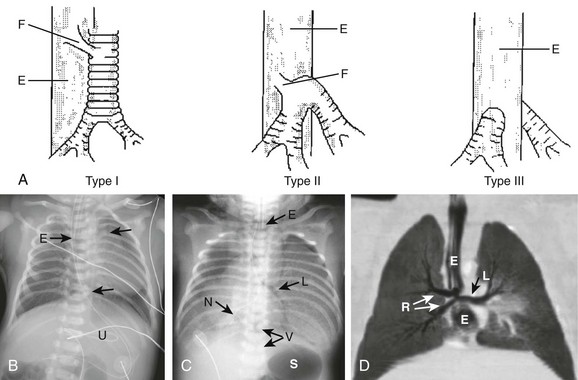
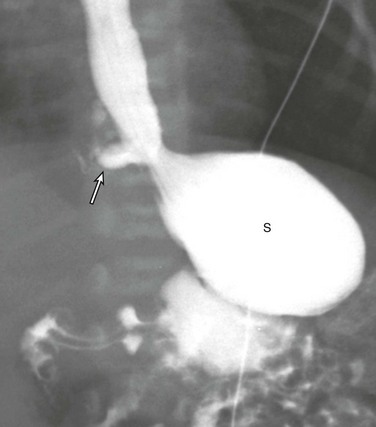
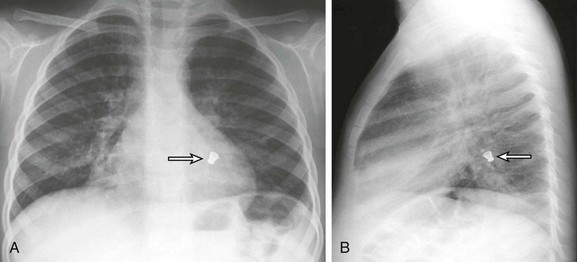
Chapter 52 Disorders of the lower large airways are common in the pediatric population and have the potential to be life threatening.1–3 Because these disorders are associated with nonspecific clinical symptoms, the diagnosis frequently is missed or delayed, particularly in infants and young children. After careful investigation of the clinical history and physical examination, imaging evaluation is the next management step. Imaging plays an important role in the diagnosis of congenital and acquired lower large airway disorders. By becoming familiar with the characteristic imaging findings of lower large airway disorders, radiologists can play an important role in ensuring prompt diagnosis and guiding appropriate management of these often acute and complex conditions in pediatric patients. This chapter reviews the etiology, imaging findings, and management of the most frequently encountered congenital and acquired lower large airway disorders in the pediatric population. Large airway disorders due to primary benign neoplasms and extrinsic compression due to mediastinal vascular anomalies are not included in this chapter because they are discussed in detail in other chapters (Chapters 51 and 77, respectively) in this book. Etiology: Tracheal agenesis, which is a rare congenital anomaly of unknown etiology, is characterized by either partial or complete tracheal underdevelopment.4–6 This condition frequently is associated with maternal polyhydramnios, and a tracheoesophageal or bronchoesophageal fistula often is present concomitantly.4–7 Three main types of tracheal agenesis exist. Type 1 consists of absent upper trachea and connection of the lower trachea to the esophagus; type 2 consists of a common bronchus connecting bilateral main bronchi to the esophagus; and type 3 consists of independent bilateral main bronchi arising from the esophagus (Fig. 52-1, A). Of these three types, type 2 is the most common. Affected patients typically present with severe respiratory distress and absence of an audible cry, and the airway cannot be intubated below the larynx immediately after birth.4–7 The diagnosis of tracheal agenesis should be considered in any infant who demonstrates improved lung ventilation after placement of the endotracheal tube in the esophagus following an initial unsuccessful intubation attempt. Once tracheal agenesis is diagnosed, radiologists should look carefully for other congenital anomalies that frequently are associated with this condition, such as congenital heart disease, duodenal atresia, and radial ray anomalies.4–7 Imaging: Chest radiographic imaging findings of tracheal agenesis often are nonspecific, such as absent or decreased lung volume. However, the diagnosis of tracheal agenesis should be considered when absence of the normal tracheal air lucency, abnormal carinal position, and placement of the endotracheal tube in the esophagus are seen on chest radiographs of infants with severe respiratory distress immediately after birth (Fig. 52-1, B and C). The diagnosis is confirmed by computed tomography (CT) and/or bronchoesophagoscopy.4–8 These studies can show both the partial or complete tracheal underdevelopment and anomalous bronchi connected to the esophagus (Fig. 52-1, D). Treatment and Follow-up: Because of difficulties related to both early diagnosis and treatment, tracheal agenesis usually is a fatal condition.4–7 The initial management of tracheal agenesis is aimed at early diagnosis at birth and immediate maintenance of airway patency, usually via the esophagus in the presence of a bronchoesophageal fistula. Although several surgical approaches have been proposed in the past, definitive treatment currently has not been established, and long-term survival of affected patients is rare. However, patients with short-segment tracheal agenesis may be amenable to direct tracheal anastomosis.5,7 Etiology: Tracheal bronchus is a congenital bronchial branching anomaly in which an ectopic (more frequently) or supernumerary bronchial branch arises from the lateral tracheal wall just above the carina.9–15 This condition also is known as bronchus suis because it is a normal finding in pigs. The incidence of tracheal bronchus in the pediatric population is between 0.1% and 5%.16 Although tracheal bronchus most frequently occurs on the right side, it also can present on the left side or bilaterally. Most patients with tracheal bronchus are asymptomatic, and it is usually an incidental finding detected on imaging studies obtained for the workup of other medical conditions. However, patients with tracheal bronchus also may present with symptoms such as persistent or recurrent upper lobe pneumonia, atelectasis, or air trapping.11 Additionally, tracheal bronchus may unexpectedly be discovered after intubation as a result of upper lobe atelectasis related to inadvertent occlusion of the ectopic upper lobe bronchial orifice by a low-lying endotracheal tube.14 Imaging: On chest radiographs, secondary imaging findings of tracheal bronchus such as upper lobe atelectasis or pneumonia can be detected, but the anomalous upper lobe bronchus cannot be reliably visualized. In the past, tracheal bronchus was evaluated with tracheobronchography. However, CT with two-dimensional (2D) and three-dimensional (3D) reconstructions is now the imaging technique of choice for evaluating anomalous tracheal bronchus and associated lung abnormalities17–19 (Fig. 52-2). Bronchoscopy can confirm the diagnosis of tracheal bronchus when necessary. Figure 52-2 Tracheal bronchus in a 1-year-old boy with recurrent right upper lobe atelectasis. Treatment and Follow-up: Pediatric patients with incidentally detected tracheal bronchus generally do not require any treatment. However, symptomatic children with recurrent upper lobe infection due to tracheal bronchus may require surgical resection, especially if permanent lung damage has developed or they are considered at risk for the development of permanent lung damage.1 Etiology: Esophageal bronchus or lung is a rare congenital anomaly.11,20 The term “esophageal bronchus” refers to the condition in which a lobar bronchus, typically the medial basal segment of the right lower lobe, arises directly from the esophagus. The term “esophageal lung” is used when the main bronchus arises directly from the esophagus. This condition most commonly presents in infants but may be diagnosed at any age. It is associated with a wide spectrum of clinical presentations ranging from asymptomatic to recurrent severe pulmonary infections or even death depending on the size and location of the anomaly. In general, symptomatic pediatric patients with esophageal bronchus or lung typically present with feeding difficulties and recurrent respiratory tract infections. Other associated congenital anomalies include congenital heart disease, duodenal atresia, duodenal stenosis, distal tracheoesophageal fistula, and esophageal atresia. Imaging: On chest radiographs, affected patients typically present as a result of aspiration during feeding, with air space opacification in the medial lower lobe in the case of esophageal bronchus and air space opacification that involves the entire lung in the case of esophageal lung.1,11 An esophagogram can provide a definitive diagnosis by allowing visualization of a direct communication between a bronchus and the esophagus (Fig. 52-3). CT may be helpful for evaluating associated lung parenchymal abnormalities and guiding surgery. Etiology: Congenital tracheal stenosis is a rare condition characterized by intrinsic narrowing of the tracheal lumen, usually as a result of underlying complete cartilaginous rings.2,3,21,22 Such cartilaginous rings with an absent or deficient posterior membranous portion render the tracheal lumen smaller and less pliable. Affected patients present in the first year of life with expiratory stridor, wheezing, and respiratory distress.2,3,21,22 Congenital tracheal stenosis traditionally is classified into three types, including (1) focal (50%), (2) generalized (30%), and (3) funnel shaped (20%).23 Other congenital anomalies often associated with congenital tracheal stenosis are tracheoesophageal fistula, pulmonary agenesis or hypoplasia, pulmonary artery sling type 2, and bronchial stenosis.2,3,11,24 Imaging: Although neck and chest radiographs or fluoroscopy may lead to the suspicion of congenital tracheal stenosis when a narrowed trachea is encountered in pediatric patients with respiratory symptoms, CT is the imaging modality of choice for diagnosis and characterizion.2,4,24 With CT, the diagnosis of congenital tracheal stenosis is based on the identification of decreased caliber of the trachea without evidence of tracheal wall thickening. The size of the subglottic region (which does not contain tracheal cartilage) can serve as an internal reference standard. The use of 2D/3D reconstructed CT imaging is particularly helpful for increasing detection of subtle stenoses, improving measurement of craniocaudal extent of disease, and enhancing evaluation of its anatomic relationship with other mediastinal structures for preoperative assessment (Fig. 52-4).2,4,24 Virtual bronchoscopic images can confirm the diagnosis of complete rings by showing concentric rings extending along the posterior wall of the trachea.25 This appearance contrasts with the normal appearance in which the C-shaped rings do not extend to the posterior membranous wall.25 In addition, virtual bronchoscopy has the capability of evaluating the airways distal to high-grade trachea stenoses, beyond which a conventional bronchoscope cannot pass.2,4,24,25 CT also may aid in the detection of other associated anomalies that often have an abnormal lung component. Treatment and Follow-up: Treatment of congenital tracheal stenosis mainly depends on the following three factors: (1) degree, (2) location, and (3) extent of the tracheal narrowing. A short tracheal stenosis may be treated by end-to-end anastomosis, whereas a longer lesion may require a patch or autograft repair.22 Other available options for short-segment tracheal stenosis include stent placement or balloon dilatation, although these methods are used more commonly to treat acquired tracheal stenosis. Etiology: Tracheobronchomegaly, also known as Mounier-Kuhn syndrome, is a rare disorder characterized by dilatation of the trachea and main bronchi.26–28 Although the exact etiology of this condition currently is unknown, a defect in the elastic and muscular tissues of the large airways is presumed to be a potential underlying cause. The increased compliance of the large airway walls as a result of the atrophy of longitudinal elastic fibers with thinning of the muscularis mucosa often results in the development of broad, diverticulum-like protrusions of redundant musculomembranous tissue between the cartilaginous rings. It may occur either as a familial condition or in association with a connective tissue disorder such as Ehlers-Danlos syndrome.29 It typically occurs in pediatric patients who have received prolonged ventilatory support or who have a chronic pulmonary infection such as cystic fibrosis. Although the clinical manifestations of tracheobronchomegaly are nonspecific, affected patients may present with a harsh cough, copious purulent sputum, occasional hemoptysis, and progressive dyspnea. Imaging: Chest radiographs alone may be adequate to detect the enlargement of trachea and bronchi in severe cases (Fig. 52-5), but CT is the imaging modality of choice for diagnosing tracheobronchomegaly, potential tracheal diverticulum, and associated lung abnormalities (Fig. 52-6).1 Because of the increased incidence of tracheobronchomalacia (TBM) in patients with tracheobronchomegaly, a dynamic CT study consisting of both inspiratory and expiratory phase imaging may be beneficial for detecting concomitant TBM. Figure 52-5 Tracheobronchomegaly. Treatment and Follow-up: Asymptomatic pediatric patients with tracheobronchomegaly require no specific treatment. For symptomatic patients, treatment usually is conservative, including chest physiotherapy for assistance with clearing of secretions and antibiotics for treatment of pulmonary infections.30,31 Unfortunately, the generalized nature of this disorder limits possible benefits from surgical management. Etiology: Foreign body aspiration into the tracheobronchial airway is a frequent cause of acute respiratory distress in pediatric patients, especially those between 6 months and 3 years of age.1–3,32,33 Each year, aspirated foreign bodies are responsible for approximately 160 deaths in children aged 14 years or younger in the United States alone, along with substantial additional morbidity.32,33 Although some pediatric patients may present with a clinical history of possible aspiration followed by cough, wheezing, respiratory distress, or decreased breath sounds, most affected pediatric patients present with a history that is either lacking or misleading.1–3,32,33 Therefore a high clinical suspicion and thorough investigation are required for any infants and young children with respiratory symptoms suspicious for possible foreign body aspiration. Only approximately 10% of aspirated foreign bodies within the tracheobronchial airway are radiopaque.34 The remaining 90% of nonradiopaque foreign bodies are particularly difficult to diagnose early in pediatric patients. Nearly 70% of aspirated foreign bodies lodge in the bronchi, with the right side (52%) affected more frequently than the left side (18%).32 The remaining 30% of aspirated foreign bodies lodge in the trachea (13%) and less common locations (17%).32 In the early phase of foreign body aspiration, affected patients typically present with cough, wheezing, respiratory distress, or decreased breath sounds. During the late phase of missed foreign body aspiration, affected patients often present with episodic wheezing and/or recurrent pneumonias. Imaging: Radiographic findings of foreign body aspiration depend on the size, location, duration, and nature of the aspirated foreign body (Fig. 52-7). Radiopaque foreign bodies usually are detected easily with radiographic studies, which should include frontal and lateral films encompassing the upper airway from the nasopharynx to the upper abdomen. When the foreign body is not radiopaque, careful inspection of the tracheobronchial airway with high-kilovoltage films or fluoroscopy may show a faintly visible opacity interrupting the air column within the large airways. If the foreign object is located in the trachea, the chest radiograph may be normal or may show bilateral hypoinflation or hyperinflation depending on the degree of obstruction. Many intratracheal foreign bodies escape detection without the use of CT.
Lower Large Airway Disease
Overview
Spectrum of Lower Large Airway Disease
Tracheobronchial Branching Anomalies
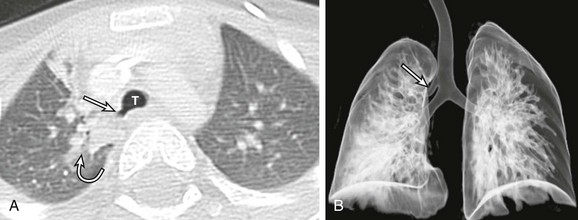
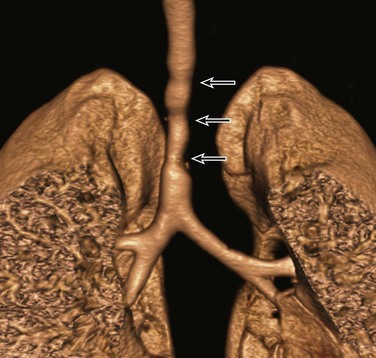
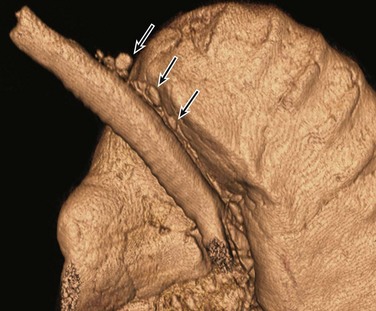
A, An axial lung window computed tomography (CT) image shows an anomalous right upper lobe bronchus (straight arrow) directly arising from the trachea (T). Atelectasis (curved arrow) is present in the medial right upper lobe. B, A frontal three-dimensional (3D) volume-rendered image of the central airways and lungs shows an anomalous right upper lobe bronchus (arrow) directly arising from the trachea. The location, size, and course of this anomalous right upper lobe bronchus (i.e., tracheal bronchus) are better demonstrated on a 3D volume-rendered image than on an axial CT image (A).
Congenital Tracheal Stenosis
Tracheobronchomegaly
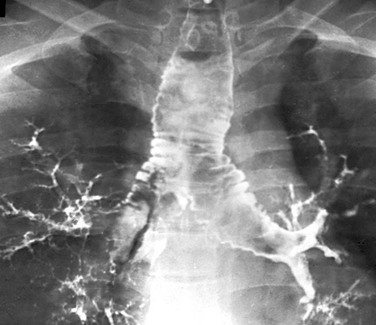
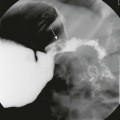
A tracheogram shows marked dilatation of the trachea and larger bronchi and indentations of the tracheal wall between the cartilaginous rings. (From Katz I, Levine M, Herman P. Tracheobronchomegaly: the Mounier-Kuhn syndrome, AJR Am J Roentgenol 88:1084, 1962.).
Acquired Abnormalities