George M. Bridgeforth and George Holmes
A 41-year-old woman presents with severe toe pain several hours after a horse stepped on her toe.
CLINICAL POINTS
- Evidence of infection (swelling, warmth, erythema, and purulent drainage), especially in patients with diabetes, may be seen.
- Throbbing pain may be a common complaint.
- Delayed capillary refill indicates impaired blood flow and necessitates a “stat” referral.
Clinical Presentation
Fractures of the phalanges (toes) are rather common and are often diagnosed and treated by primary care physicians. They are characterized by pain, swelling, and tenderness of the fractured phalanx. Patients commonly complain that they are not able to wear a regular shoe. When walking, they characteristically exhibit a poor push-off, with limited weight bearing of the forefoot. The mechanism of injury in toe fractures is direct trauma (e.g., from stubbed toes or falling objects).
The clinician should perform a careful physical examination. Assessment and documentation of deformity of the injured digit is essential. (The phalanges [toes] are numbered one through five, starting with the big toe.) To distinguish contusions from fractures, it is necessary to view the radiographs. In addition, the examiner should inspect the skin for open wounds or significant injury that may lead to necrosis. It is also necessary to inspect the nails for subungual hematomas and other nail injuries such as paronychia, an infection that subsequently develops along the nail edge. Patients with painful subungual hematomas who do not have associated phalangeal fractures may undergo a trephination in which a small hole is placed in the nail with a sterile heated needle or electrical cautery. The pressure under the nail caused by the hematoma is relieved. Pain and soreness between the third and the fourth phalanges may be secondary to a Morton’s neuroma. This is a painful irritation of the plantar digital nerve. It is more common in females and may be caused by high heels or tightly fitting shoes. It does not appear on radiographs and it is marked characterized by tenderness of the web space. Lastly, the examiner should check the pulses and inspect for coldness, cyanosis, and discoloration. The neurovascular examination should always be well documented.
PATIENT ASSESSMENT 
- Pain, swelling, and tenderness of the affected phalanx/phalanges
- Poor range of motion
- Antalgic gait (limp) with a poor push-off
Patients with diabetes who have foot contusions or fractures are more likely to develop serious infections and should be monitored carefully. Severe infections in these patients may lead to an associated osteomyelitis (i.e., an infection of the bone), and close follow-up is critical. They present initially with minor foot (phalangeal fractures) or contusions; without careful monitoring, they can decompensate within a 3- to 4-week period.
Radiographic Evaluation
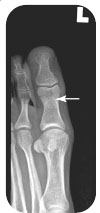
Anteroposterior (AP) (Fig. 28.1), lateral (Fig. 28.2), and oblique views should be obtained.
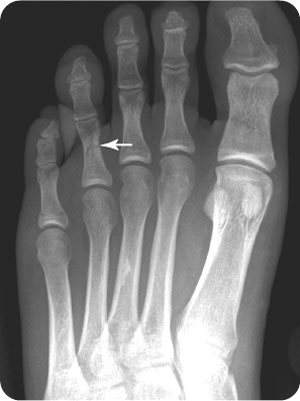
FIGURE 28.1 Anteroposterior radiograph demonstrates a comminuted fracture of the fourth proximal phalanx.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree