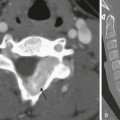
Chapter 59 The chest wall provides support and protection to the various thoracic vascular and nonvascular structures. In addition, it allows the important physiologic motion of the lungs and airways. The chest wall is less rigid and more cartilaginous in children than in adults and consists of several fundamental structural components, including bones (ribs, sternum, and vertebrae), nerves, muscles, vessels, and subcutaneous soft tissues.1 Within these structural components, a wide variety of localized or systemic processes (e.g., congenital and developmental anomalies, inflammatory and infectious diseases, benign and malignant neoplasms, and traumatic lesions) can occur in pediatric patients.1–3 During childhood, congenital and developmental anomalies of the thorax typically manifest as deformities or anterior chest wall defects that can be isolated or part of a syndrome. Most of these lesions do not have serious physiologic consequences but rather cause cosmetic problems. However, pediatric patients with severe degrees of congenital or developmental anomalies of the chest wall may present with pain, respiratory distress, or cardiovascular compromise. Reconstructive surgery can be offered to correct the chest wall deformities or defects in both asymptomatic and symptomatic pediatric patients. Imaging can provide a road map for the surgeon in evaluating the anatomy and associated anomalies that can affect the reconstructive options, as well as the timing of surgery. Furthermore, accurate recognition of the radiologic manifestation of congenital and developmental conditions that affect the chest wall often provides important clues that point to the correct diagnosis.4 Etiology: Most asymptomatic palpable anterior chest wall lesions in pediatric patients are normal anatomic osseous or cartilaginous variants of the shape of the costal cartilage, ribs, and sternum.5,6 These normal anatomic variations occur in approximately one third of children.5 The most common cause of an asymptomatic, palpable anterior chest wall mass on physical examination is prominent anterior convexity of a solitary rib, costal cartilage, or sternal tilt (Fig. 59-1).6 Symptoms that may raise concern and require further evaluation are focal pain and rapid growth of the mass.3,5 Figure 59-1 A chondral nodule in an adolescent boy who presented with a focal, palpable, painless lump in the anterior chest wall. Imaging: In the case of a palpable but otherwise asymptomatic anterior chest wall lesion in children, a chest radiograph with a BB marker is usually adequate to exclude a potentially aggressive or malignant underlying condition. When chest radiographic findings are equivocal, ultrasound can be performed.7 To minimize ionizing radiation exposure, computed tomography (CT) should be reserved for situations in which further characterization is still necessary after radiographic and ultrasound evaluation.3,6 Although it often is less available than CT, magnetic resonance imaging (MRI), which is not associated with ionizing radiation exposure, is a particularly helpful imaging modality for confirming and characterizing congenital and developmental chest wall lesions. Etiology: Two of the most common abnormalities of the chest wall are pectus excavatum and pectus carinatum, with the former being the most common congenital deformity of the sternum and the most common sternal deformity requiring surgery. The current leading theory for the development of pectus excavatum is a misdirected, rapid growth of the lower costal cartilages. Such abnormal growth of the lower costal cartilages, which often intensifies during growth spurts, displaces the sternum either inward or outward, resulting in pectus deformity.8 Pectus excavatum occurs in between 1 in 400 and 1 in 1000 live births.9 In persons with pectus excavatum, the inferior aspect of the sternum is depressed inward, resulting in varying degrees of anterior chest wall concavity and anterior protrusion of the costochondral junctions. Although most cases of pectus excavatum are isolated, approximately 45% of cases are familial.10,11 Pectus carinatum is a less common chest wall deformity that occurs in approximately 1 in 1500 live births and has a familial occurrence of approximately 25%.9 In persons with pectus carinatum, outward displacement of the sternum occurs, with secondary abnormal protrusion of the ribs. Pectus deformities may occur in association with scoliosis (more frequently with pectus excavatum), Marfan syndrome, Ehlers-Danlos syndrome, Poland syndrome, and congenital heart disease. In addition to cosmetic issues, severe pectus deformities also can cause chest pain, dyspnea, palpitations, and restrictive lung disease.3 Imaging: On frontal chest radiographs, the sternal depression of pectus excavatum may cause a pseudo-infiltrate over the right side of the heart and various degrees of leftward cardiac shift. On the lateral chest radiograph, the sternal depression causes narrowing of thoracic anteroposterior (AP) diameter (Fig. 59-2). Pectus carinatum usually is diagnosed on a lateral chest radiograph, which shows an increased AP diameter of the thoracic cavity and an extended retrosternal space (Fig. 59-3).3,8 Figure 59-2 Pectus excavatum in an 8-year-old girl. Figure 59-3 Pectus carinatum in an adolescent boy. The Haller or pectus index is used to estimate the severity of pectus excavatum. It is calculated from an axial CT image by dividing the maximum transverse dimension of the thorax from the inner aspect of the ribs by the AP dimension of the thoracic cavity at its narrowest point (Fig. 59-4). A pectus index greater than 3.25 in symptomatic pediatric patients typically initiates corrective surgery, whereas an index less than 2.56 is considered normal.12 Recent studies have advocated the use of chest radiographs instead of CT to preoperatively evaluate the severity of the deformity.13 In more severe cases, the use of a limited, low-dose CT scan with selective 5-7 axial CT images through the deformity can be obtained to generate the pectus index.14 When the primary purpose of imaging is to assess the Haller index, axial MRI can be used to avoid ionizing radiation.15 Treatment and Follow-up: Severe pectus deformity requires surgical correction, particularly in symptomatic pediatric patients. The Ravitch procedure for pectus excavatum includes resection of deformed cartilages and correction of the sternum by a wedge osteotomy in the upper sternal cortex. In the Nuss procedure, a convex metal bar is placed behind the sternum, pulling the sternum anteriorly. Corrective surgery for pectus carinatum also requires costochondral resection and a wedge osteotomy, but the sternum is pushed inward. The Nuss procedure has a 4% to 11% complication rate,16 and thus follow-up imaging is necessary to monitor the implanted bar and its complications. Infection and dislocation of the metallic bar are the two most common complications following the Nuss procedure.16–18 Etiology: Cleidocranial dysostosis is a rare syndrome usually caused by an autosomal dominant gene with high degree of penetrance and variable expression. In this condition, a mutation is present in the CBFA1 gene located in the chromosome 6p21, which encodes a protein necessary to activate osteoblast differentiation. The triad of partial or complete absence of the clavicles, supernumerary or impacted teeth, and delayed fontanel closure is highly suggestive of this syndrome. Other features of the syndrome include midface hypoplasia, short stature, and pelvic and distal phalangeal hypoplasia that causes brachydactyly.19–21 Imaging: Typical chest radiographic findings include a bell-shaped thorax, short ribs, and either complete or partial absence of the clavicles (e-Fig. 59-5). When the clavicle is partially absent, the distal portion of the clavicle usually is involved. Scoliosis may be present. Because many of the characteristic manifestations only become evident during adolescence, early clinical diagnosis may be difficult and often requires a skeletal survey. Other features of the syndrome can support the diagnosis.19–21 e-Figure 59-5 Cleidocranial dysostosis in an adolescent boy. Treatment and Follow-up: Multidisciplinary management by a team of specialists including pediatricians, geneticists, and orthodontists is the optimal approach for patients with cleidocranial dysostosis. Genetic counseling is recommended. No imaging follow-up is required once the diagnosis has been made.19 Etiology: Poland syndrome is a form of chest wall and breast hypoplasia that occurs in 1 in every 20,000 to 30,000 live births.22 The syndrome includes absence of the pectoralis muscles and ipsilateral syndactyly. Other associations include rib aplasia, amastia/athelia, and absence of axillary hair. Poland syndrome typically is unilateral and (more often) sporadic and occurs more frequently in boys than in girls, with a ratio of 2-3 : 1.23 The tendency toward unilaterality (with the right side affected more frequently than the left side) has raised the hypothesis that this anomaly is perhaps a result of interrupted or insufficient blood supply during limb bud development in the sixth week of gestation.23 Poland syndrome is diagnosed clinically by the apparent asymmetry of the chest wall (e-Fig. 59-6) and syndactyly. Cardiopulmonary impairment and functional deficiency of the shoulder, although rare, also can be present.3,22,23 e-Figure 59-6 Poland syndrome in an adolescent boy. Imaging: On chest radiographs, hyperlucency of the affected hemithorax is usually apparent in unilateral cases because of the absent pectoralis muscle and breast (Fig. 59-7). Because the extent of involvement is difficult to assess with clinical examination or chest radiographs, cross-sectional imaging with CT or MRI is useful (Fig. 59-8). Furthermore, it is imperative to preoperatively assess the presence of all of the chest wall and anterior abdominal wall muscles (e.g., the latissimus dorsi and rectus abdominis muscles), because muscle flaps are used in surgical reconstruction.2,22 Figure 59-7 Poland syndrome in an adolescent girl. Treatment and Follow-up: Corrective surgery often is performed for cosmetic reasons, particularly in girls. Such surgery includes (1) restoration of the structural integrity of the rib cage and (2) improvement in the appearance of the chest by performing transposition of musculocutaneous flaps (most commonly with latissimus dorsi and rectus abdominis muscles), as well as concomitant breast implants in female patients.8,22,23 Chest wall infections are relatively rare in children. Chest wall infections occur either by direct extension or, less frequently, by hematogenous spread. Such infectious processes can involve the soft tissues, cartilage, and osseous structures. Chest wall infections can be the result of bacterial, mycobacterial, or fungal infections. They range from superficial cellulitis to deeper infections, which include myositis, abscess, necrotizing fasciitis, and osteomyelitis.24,25 Etiology: Bacterial infections of the chest wall are rare in children. The common organisms that cause bacterial infections of the chest wall are Staphylococcus aureus and Salmonella species in persons with sickle cell disease. Sternal osteomyelitis may occur in patients with an underlying disease, such as immunodeficiency and hemoglobinopathies.11 Rib osteomyelitis is most commonly acquired by direct spread from an adjacent pleuropulmonary infection, such as severe pneumonia or empyema. Empyema necessitatis is a rare complication of empyema characterized by the extension of the infection from the pleural space into the chest wall. Pediatric patients with a bacterial chest wall infection often present with focal soft tissue erythema, edema, and pain. Additionally, other signs of infection, such as leukocytosis and elevated erythrocyte sedimentation rate, often are present.3,11,26,27 Imaging: Chest radiographs may reveal localized soft tissue edema in cases of cellulitis or fasciitis. Bone changes such as periosteal reaction or lytic or sclerotic lesions can be present, particularly in the late stage of disease. Concomitant pulmonary consolidation, empyema, and subcutaneous emphysema also may be present. Ultrasound, CT, and MRI are more sensitive than chest radiographs in detecting and characterizing chest wall infections. Ultrasound should be reserved for superficial and more localized chest wall infections because of the limited field of view (Fig. 59-9, A). The extent of the chest wall infection is best demonstrated on CT or MRI. For evaluation of chest wall abscess and bone marrow edema in the earlier stage of osteomyelitis, MRI is the most sensitive imaging modality (Fig. 59-9, B). CT is the imaging modality of choice for evaluating concomitant pulmonary parenchymal infection.2,11,26–28 Figure 59-9 Sternal osteomyelitis in a 6-year-old girl who presented with prolonged fever and a painful, palpable, and erythematous sternal lump. Treatment and Follow-up: Antibiotics are administered to treat bacterial chest wall infections. In cases of abscesses localized to the chest wall or empyema, drainage may be necessary to relieve the focus of infection and avoid further spread. Prolonged antibiotic therapy is necessary for cases of osteomyelitis.27,29 Evaluation of response to treatment by monitoring C-reactive protein in pediatric patients with osteomyelitis has dramatically decreased both the average duration of therapy (now 3 to 4 weeks) and the need for follow-up imaging.30 Etiology: Tuberculosis (TB) is a potentially deadly infectious disease caused by various strains of mycobacteria, usually Mycobacterium tuberculosis in humans. Tuberculosis infection of the chest wall often is a result of the hematogenous spread of pulmonary TB infection.31 However, tuberculosis of the chest wall also can occur as an isolated primary infection with no evidence of pulmonary disease, although this presentation is rare.32 Skeletal TB infection accounts for 10% to 20% of extrapulmonary cases and 1% to 2% of all TB infection cases.33 Affected patients present with a slow-growing soft tissue chest wall mass, often without associated pain or fever. Respiratory symptoms may be present in cases of lung involvement.32,34 Imaging: TB infection can involve any bone of the chest wall; however, the ribs are most commonly affected. On radiographs, osseous TB infections are usually lytic and sharply marginated. Associated periosteal reaction is a relatively rare finding.35 On CT or MRI, TB chest wall infections usually present as a rim-enhancing chest wall mass. CT and MRI can play an important role in demonstrating bone involvement from a chest wall TB infection that may not be seen on radiographs.32 Expansion and destruction of the bone with an adjacent soft tissue mass from a TB infection of the chest wall may mimic an underlying malignancy. Rim-enhancing masses with central necrosis and sequestrum indicating abscess formation, regional hypodense adenopathy, and vertebral body involvement also may occur in affected patients.31,33,34 Treatment and Follow-up: Treatment of chest wall TB infection currently is not well established. Some persons advocate the use of an antituberculous medication regimen alone for at least 6 months. Others suggest more aggressive management consisting of surgical excision of affected bones and soft tissues, in addition to preoperative and postoperative antituberculous medication regimens.32,36 Etiology: In humans, actinomycosis is most commonly caused by Actinomyces israelii, a branching gram-positive, facultative anaerobe. Actinomycosis infection typically affects the cervicofacial region in patients with dental caries. Pulmonary and chest wall involvement of actinomycosis in children is less frequent without underlying predisposing pulmonary conditions. Actinomycosis infection initially involves the lungs and then usually spreads to the adjacent soft tissues. Clinically, affected patients present with cough, intermittent fever, and weight loss. Pain develops once the microorganism invades the pleura and chest wall.37,38 Imaging: On a chest radiograph, the classic radiologic appearance of actinomycosis infection is a chronic lung consolidation that crosses the fissures with a pleural effusion. Because actinomycosis infection does not respect tissue boundaries, it tends to invade the surrounding tissues with fistulous tracts and abscess formation that are best seen on CT or MRI. Rib periostitis, pulmonary cavitation, and diaphragmatic invasion also may occur in more advanced cases and are very suggestive of actinomycosis infection.38,39Advanced actinomycosis infection of the chest wall may mimic TB or a malignancy of the Ewing sarcoma family of tumors (ESFT).37 Treatment and Follow-up: A definite diagnosis of actinomycosis of the chest wall requires either microscopic visualization of the typical sulfur granules representing the colonies of the microorganism or recovery of the Actinomyces organisms in an anaerobic culture. The standard treatment of actinomycosis is long-term, high-dose penicillin. In cases with an abscess, image-guided percutaneous drainage may help expedite recovery and isolate the organism. Rarely, surgical resection of the area involved is required in cases that are unresponsive to medical treatments.37,38 Because the chest wall is composed of several different types of tissues, a wide variety of both benign and malignant tumors may occur, including vascular, cartilaginous, osseous, muscular, or adipose tumors. Imaging evaluation plays a pivotal role in (1) initial detection, (2) assessment of the extent of disease, (3) guidance for tissue sampling, (4) evaluation of the response to treatment, and (5) surveillance for recurrence.7,25 Etiology: Infantile hemangiomas are benign vascular tumors of abnormally proliferating endothelial cells that follow a predictable course. Infantile hemangiomas are the most common tumor of childhood, with a reported incidence of approximately 10% in the general population.40,41 The etiology of hemangiomas currently is unknown. Several proposed theories include placental emboli, somatic mutation, and clonal expansion of progenitor stem cells.42,43 Infantile hemangiomas are more common in premature white children, with female predominance ratios ranging from 1.4 : 1 to 3 : 1.41 Hemangiomas can involve any part of the body, including the chest wall and breast bud. At birth, these lesions frequently are underdeveloped, with only a macule or discoloration representing a “precursor” lesion. Soon after birth, infantile hemangiomas grow during the so-called proliferative phase and become raised and red in color. Around the first year of life, they involute, leaving a fibro-fatty scar. Multiple lesions are found in 15% to 30% of patients.41,43 Imaging: Ultrasound is usually the first imaging modality of choice, especially for evaluating localized, superficial hemangiomas. For large and extensive lesions with a deep soft tissue component, MRI often is necessary for a complete evaluation. Although CT can be used when MRI is not available, it is less preferable because of the associated radiation and inferior soft tissue characterization. The imaging appearance of infantile hemangiomas may change according to the stage of disease. On ultrasound, hemangiomas are well-defined, lobulated, hyperechoic masses that become more heterogeneous during the involuting phase. Increased vascularity, containing arteries, veins, and even evidence of shunting, often is seen on color Doppler, especially during the proliferative phase (e-Fig. 59-10). On MRI, infantile hemangiomas are isointense or slightly hyperintense compared with muscle on T1-weighted images, and they are hyperintense on T2-weighted images, containing flow voids that represent arteries or rapid venous flow. Hyperintense fatty elements may be seen on T1-weighted images. The pattern of contrast enhancement also varies according to the stage of disease. Marked contrast enhancement usually is seen during the proliferative phase, whereas heterogeneous contrast enhancement reflecting areas of necrosis often is observed during the involuting phase. On CT, hemangiomas present as well-defined soft tissue masses that are isodense to muscle with marked postcontrast enhancement.43,44 e-Figure 59-10 An infantile hemangioma in a 6-week-old girl in whom a raised red cutaneous lesion developed in the anterior chest wall 3 weeks after birth. Treatment and Follow-up: Most infantile hemangiomas require no treatment because they typically involute. A pulsed dye laser can be used for the cosmetic management of superficial lesions. In the past, corticosteroids were the cornerstone of management of hemangiomas; however, secondary effects, such as cushingoid features, were commonly seen.30 Propranolol has been used recently in the treatment of hemangiomas with promising results and minor complications, such as hypoglycemia and hypotension.45,46 Etiology: Lymphatic malformations are a subtype of slow-flow vascular malformations. These lesions are fully developed at birth and grow commensurate to the patient’s growth. Lymphatic malformations consist of dilated lymphatic channels and spaces, with walls lined by mature endothelium that have normal rates of endothelial cell turnover. These lesions occur anywhere in the body, but the cervicofacial, axillary, and chest regions are the most common locations. Lymphatic malformations have no sex predilection. Except for very small lesions, these lesions present as a mass that usually is discovered at birth. The lesions have normal overlying skin and often display positive transillumination. With superimposed hemorrhage or infection, a sudden increase in the lesion size is typical.3,47 Imaging: Plain radiography plays no role in the evaluation of lymphatic malformations in the chest wall of pediatric patients. The imaging workup of lymphatic malformations includes ultrasound and MRI, with the former more commonly used for localized and superficial lesions. More extensive lesions are better evaluated with contrast-enhanced MRI, with CT as an alternative imaging modality. On ultrasound, lymphatic malformations appear as multiloculated cystic lesions that are macrocystic or microcystic, depending on the size of the locules. No internal blood flow is seen on color Doppler imaging. With associated bleeding or superimposed infection, echogenic material, low-level echoes, or fluid-fluid levels can be observed (Fig. 59-11, A). On MRI, the cystic lesions are hyperintense on T2-weighted images (Fig. 59-11, B
The Chest Wall
Congenital and Developmental Anomalies
Deformities of the Anterior Chest Wall
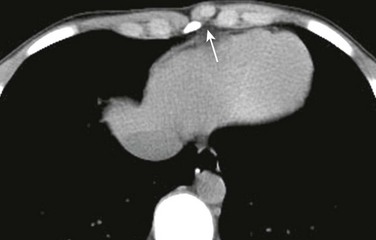
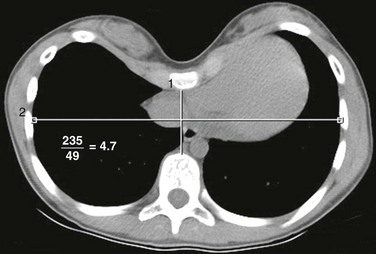
An axial computed tomography soft tissue window image shows a small, round, well-defined structure (arrow) protruding anteriorly in the chest wall to the left of the sternum with the same density as the adjacent costochondral junctions.
Pectus Deformity
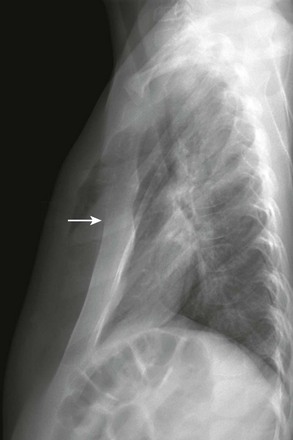
A lateral chest radiograph shows the sternal depression (arrow) causing narrowing of the anteroposterior diameter of the thorax.
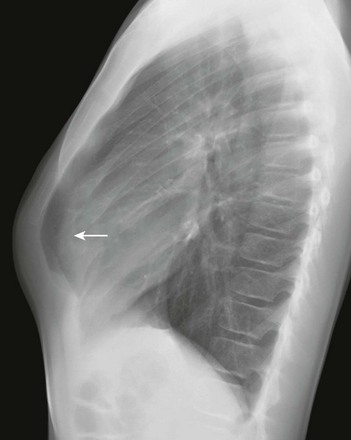
A lateral chest radiograph demonstrates an increased anteroposterior diameter of the thoracic cavity and extended retrosternal space (arrow).
Cleidocranial Dysostosis
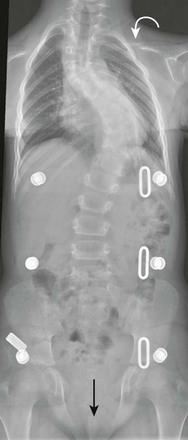
A chest and abdominal radiograph shows absence of the right clavicle and hypoplasia of the distal half of the left clavicle (curved arrow). Diastases (straight arrow) of the symphysis pubis also is present. The patient has scoliosis and is wearing a brace.
Poland Syndrome
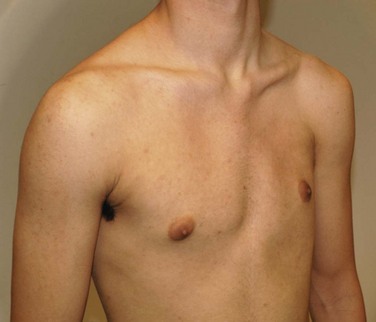
Asymmetry of the chest wall is apparent because of a lack of soft tissue on the left side.
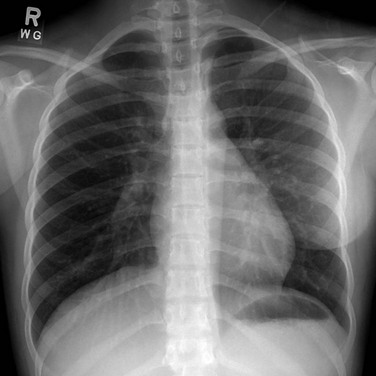
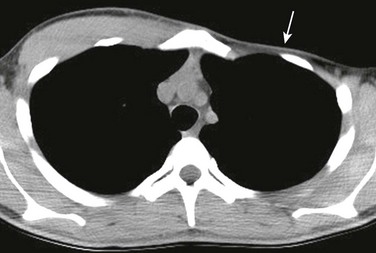
A frontal chest radiograph shows a hyperlucent right lung as a result of the absence of right chest wall soft tissues, including the breast.
Infectious Diseases
Bacterial Infection
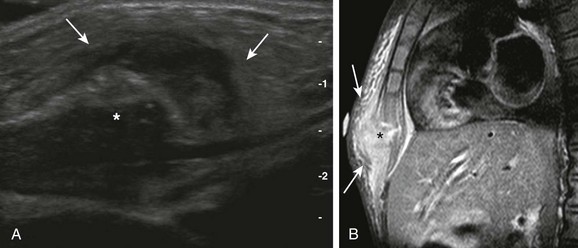
A, A longitudinal ultrasound view of the inferior aspect of the sternum (asterisk) shows marked surrounding soft tissue edema and swelling (arrows).
B, A sagittal contrast T1-weighted image of the chest with fat saturation demonstrates focal destruction of the distal ossification center of the sternum (asterisk) with contrast enhancement and edema of the adjacent soft tissues (arrows).
Tuberculosis
Actinomycosis
Tumors of the Chest Wall
Benign Tumors
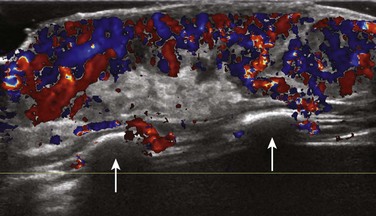
Color Doppler ultrasound of the lesion shows a well-defined soft tissue mass confined to the subcutaneous soft tissues that insinuates along the ribs (arrows) and involves the dermis. The lesion has a hyperechoic and markedly vascular soft tissue component containing arteries and veins.
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree