© Springer-Verlag Berlin Heidelberg 2012
Richard P. Baum (ed.)Therapeutic Nuclear MedicineMedical Radiology10.1007/174_2012_727Radioembolization (Yttrium-90 Microspheres) for Metastatic Hepatic Malignancies
(1)
FACRO Co-Medical Director, Wake Radiology Oncology, 300 Ashville Ave Suite 110, Cary, NC 27518, USA
(2)
Department of Biomedical Engineering, Department of Mechanical and Aeronautical Engineering, North Carolina State University, Raleigh, NC, USA
Abstract
Radioembolization is the process of permanently implanting radioactive microspheres into hepatic malignant tumors using the hepatic arterial system for delivery. The most common therapeutic radioisotope used in this form of brachytherapy (placing radioactive sources into or next to a tumor) is yttrium-90 (90Y). Since the earliest attempts to implant liver tumors, the technique has been surprisingly similar—a catheter is situated into a branch of the hepatic artery, and microspheres (25–35 micron diameter) containing 90Y preferentially flow to tumors as opposed to normal liver. The microspheres are small enough to penetrate into the tumors but too large to pass out of the hepatic capillary beds, and so they permanently reside in the tumor. The most common cancers treated with 90Y microspheres are primary hepatocellular carcinoma, and metastatic tumors from primary colorectal, neuroendocrine, pancreas, and breast carcinomas. The toxicity profile is highly favorable for this outpatient procedure with fewer than 2% serious adverse events (gastric ulceration 1–2%, radiation-induced liver failure 0.8%). Overall response rates are 30–75% (RECIST) based on tumor type, and in colorectal cancers, there is a proven survival improvement with 90Y in patients whose chemotherapy agents are no longer inducing a response. The use of radioembolization continues to rapidly grow for a variety of patient subgroups which now include first line therapy in neuroendocrine and colorectal tumor types.
The liver is one of the most commonly involved organs for metastatic carcinoma, second only to the lymph nodes (Hess et al. 2006). The majority of patients with metastatic liver cancer initially present at advanced disease progression, thereby ablative therapy is eliminated as a treatment option. Most patients with liver metastases are managed with systemic chemotherapy; however, the current agents and biological products serve to varying extents in controlling the cancer, not eradicating it. As many as 80 % of patients with colorectal cancer and liver metastases die from liver failure resulting from the local effects of hepatic tumors (Allen-Mersh 1989). At the time of death, an estimated 30–70 % of these patients have liver metastases. Radioembolization (RE), the implantation of internal radiation sources (brachytherapy with radiolabeled microspheres) into tumors, can be used as part of a liver-focused strategy to target multiple sites of hepatic disease. The two types of Yttrium-90 (90Y) radioactive microspheres, resin and glass, are delivered to hepatic tumors via the hepatic artery system. Compared with other techniques such as radiofrequency ablation, surgical resection, and external beam radiotherapy, which are limited by the number, location, and distribution of metastatic tumors, RE does not present a significant risk for non-target radiation (Nicolay et al. 2009). Rather, the radiation source is delivered directly into the hepatic artery, which provides blood flow to the tumor, thus capitalizing on the essential principles of tumor hypervascularity and concentrating radiation within the tumor while simultaneously minimizing the risks to the normal liver parenchyma.
In this chapter we discuss patient selection for and clinical results of this novel treatment for metastases from three primary sites: the colon/rectum, neuroendocrine system, and breast.
1 Patient Selection
Appropriate patient selection is integral to successful outcomes resulting from RE. The radioembolization brachytherapy oncology consortium (REBOC) consensus panel report provides detailed guidelines for patient selection with RE using 90Y-labeled microspheres (Kennedy et al. 2007). Eligibility requirements call for patients to complete a comprehensive evaluation and standard treatment of the primary tumor, demonstrating unequivocal, measurable evidence of liver metastases that cannot be surgically resected or ablated with curative intent. Further assessment for eligibility involves multiple factors including the patient’s history of chemotherapy, surgical resection, and infusion pump placement with surgically altered vascularity. The consideration of which patients are most likely to benefit from this treatment modality is made by the careful assessment of a multidisciplinary team of individuals.
Liver-dominant tumor burden is carefully assessed using imaging findings (Salem and Thurston 2006). During the RE procedure, a small amount of normal liver tissue immediately adjacent to the tumor will be destroyed by radiation; therefore, sufficient liver reserve is required. RE eligibility in each patient is therefore governed by the well-established and accepted parameters for liver reserve and vascular access. Primary parameters indicating adequate liver tolerance for RE include a lack of ascites, normal synthetic liver dysfunction (e.g., albumin >3 g/dl), and normal total bilirubin of less than 2.0 mg/dl (<34 μmol/l).
An essential determinant of eligibility is performance status, typically eastern cooperative oncology group (ECOG) criteria. Patients presenting with clearly compromised functional status (ECOG stage 2–4) are at high risk for rapid onset of liver failure and treatment-related morbidity. Therefore, treatment decisions for these clinically compromised patients are especially challenging.
By contrast, good candidates for referral are patients with a life expectancy of more than 12 weeks and ECOG status of 0–2, particularly for certain tumor types where RE can be safely combined with systemic chemotherapy. Most optimal outcomes may be achieved by earlier referral of patients with unresectable liver-dominant or liver-only disease. Integrating RE earlier into the patient’s treatment paradigm can provide additional treatment options which might lead to improved patient survival and quality of life. These options include the use of systemic chemotherapy, which can serve as a radiosensitizer, and may control extrahepatic metastases, may permit a reduction in hepatic disease, and may help to conserve remaining liver function.
2 Clinical Results
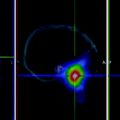
RE using 90Y microspheres has the potential to provide substantial clinical benefits through increased progression-free periods and length of survival, as well as through improved response rates. The typical side-effect profile for RE is, in general, of lower intensity than the profiles of transarterial embolization (TAE) or transarterial chemoembolization (TACE) with virtually no cases of true post-embolization syndrome. Appropriate patient selection involves accurate interpretation of pretreatment investigations, including angiography and Technetium-99 macro aggregated albumin (99mTc-MAA), which can significantly reduce the incidence of serious adverse events.
Most current reports in the literature use the common toxicity criteria of adverse events (CTCae) 3.0, although a large part of the literature uses CTCae 2.0 and World Health Organization (WHO) criteria. As is the case with embolic therapy to the liver in these tumor types, release of active peptides from abrupt tumor lysis can lead to severe symptoms. Although rare, respiratory distress and/or dangerous hypertension may develop even while the patient is receiving microsphere therapy in the interventional suite.
Although the studies conducted to date have been small, at least 30 prospective trials using RE have been reported. A number of larger randomized controlled trials are examining the role of 90Y resin microspheres in combination with chemotherapy in first-line treatment of colorectal hepatic metastases, and other trials are under way to assess 90Y microspheres either in combination with chemotherapy or as monotherapy in non-colorectal metastases and in primary liver tumors. The results of these studies will help to further define the role of RE as cancer therapy.
2.1 Colorectal Metastases: Toxicity and Outcomes
In colorectal carcinoma, it is the presence or absence of liver metastases, rather than the primary carcinoma, that leads to significant clinical morbidity and determines the life expectancy for the patient (McMillan and McArdle 2007). In a subset of patients with liver-only metastatic colorectal cancer (mCRC) in whom surgical resection of disease can be achieved, the probability of five year survival is 30–40 %, and 20 % of patients achieve a long-term cure (Nordlinger et al. 2007). A prospective evaluation of 1,325 patients with colorectal cancer demonstrated that median survival following the diagnosis of colorectal liver metastases was approximately 10 months (range 4.6–23.1 months), and that the age of patient and the extent of disease were the key limiting factors for surgical resection and palliative chemotherapy (Leporrier et al. 2006).
To improve overall survival for patients with mCRC, ongoing research is helping to identify the means of achieving local tumor control or increasing the downsizing rates of liver metastases. Localized high-dose tumor-directed radiation effectively reduces mCRC burden. A single RE treatment induces profound cytoreduction of mCRC in the liver and significantly prolongs time to progression (TTP), progression-free survival (PFS), and overall survival (OS) even among patients with highly chemorefractive disease.
In this setting, RE therapy is given (1) alone after failure of first-line chemotherapy, (2) combined with FUDR during first-line therapy, or (3) during first- or second-line chemotherapy on a clinical trial, and (4) in salvage therapy combined with 5-fluorocil (5FU), leucovorin, oxaliplatin, or irinotecan.
For the first-line therapy of patients with advanced unresectable liver metastases and with or without extrahepatic metastases, RE augments the treatment response of systemic chemotherapy. Progression free survival (PFS), overall survival (OS), and response rates compare favorably with phase II/III data for modern chemotherapy regimens with or without biologics (Kulik et al. 2005, 2006; Rhee et al. 2005; Salem et al. 2005). In a randomized controlled trial comparing 90Y RE with resin microspheres plus first-line systemic 5-fluorouracil/leucovorin (5FU/LV) chemotherapy versus 5FU/LV alone, the cohort comprised 21 patients with unresectable liver metastases that could not be treated by resection or any local ablative technique. No patient had received prior chemotherapy or radiotherapy for the mCRC (Van Hazel et al. 2004). Prior to randomization, patients were stratified by institution, presence or absence of extrahepatic metastases, and extent of liver involvement by tumor (>25 or <25 %). Both treatment arms received the mayo clinic regimen of 5FU/LV (425 mg/m2/day and 20 mg/m2/day respectively) for five consecutive days and a repeated dose at four weekly intervals. A single administration of 90Y resin microspheres added to a 5FU/LV regimen was associated with significant increase in response rate (91 vs. 0 %; P < 0.001), TTP (18.6 vs. 3.6 months; P < 0.0005), and median OS (29.4 vs. 12.8 months; P = 0.02) compared with systemic chemotherapy alone. Importantly, at 3 months posttreatment, the addition of 90Y resin microspheres to 5FU/LV chemotherapy was associated with a significant improvement in health-related quality of life compared with 5FU/LV alone (P = 0.03) (van Hazel et al. 2009). As first-line therapy, a trial of FOLFOX4 chemotherapy combined with 90Y resin microspheres has been completed (Sharma et al. 2007) and is the therapeutic basis for two ongoing phase III studies (FOXFIRE and SIRFLOX) that includes more than 800 patients. (http://clinicaltrials.gov/ct2/show/NCT00724503; Sharma et al. 2008).
RE as second- or third-line chemotherapy combined with irinotecan has also shown good results, including no dose-limiting toxicity (van Hazel et al. 2009). Although 60 % of patients had failed oxaliplatin-based regimens and over a third had failed 2 or 3 previous lines of chemotherapy, the combination of RE with irinotecan was associated with an ORR of 48 % and a disease control rate of 87 %. The median PFS was 6.0 months at any site and 9.2 months in the liver, and median OS was 12.2 months (range 2.8–48 + months) (van Hazel et al. 2009).
As salvage therapy in patients with chemotherapy-refractory mCRC, efficacy and safety data from several other prospective studies have demonstrated the value of RE alone or combined with a radiosensitizing chemotherapy regimen.(Cosimelli et al. 2008; Van den Eynde et al. 2009; Mulcahy et al. 2009; Ricke et al. 2009; Jakobs et al. 2008; Kennedy et al. 2006). A multicenter randomized controlled phase III trial assessed the addition of 90Y resin microspheres to 5FU given by continuous IV infusion in 46 patients with mCRC limited to the liver who had failed available standard-of-care chemotherapy(Van den Eynde et al. 2009). Patients were randomized to receive 5FU alone or 90Y resin microspheres with a modified regimen of 5FU. Median time to liver progression, the primary endpoint of the trial, was significantly longer in patients receiving RE compared to 5FU alone (5.5 vs. 2.1 months, respectively; P = 0.003). Median TTP of disease anywhere in the body was also significantly longer (4.6 vs. 2.1 months; P = 0.03) and significantly more patients receiving 90Y resin microspheres achieved disease control (85 vs. 35 %; P = 0.01). Following disease progression, 90Y resin microspheres was administered as salvage therapy in ten patients (43.5 %) in the 5FU-only arm. Targeted treatment of liver tumors extended survival in both treatment arms. Median survival was 7.4 months in the 5FU-only arm and 9.9 months in patients receiving 5FU plus 90Y resin microspheres (P = 0.80). RE was well tolerated, with significantly more patients experiencing a serious adverse event in the 5FU-only control arm (4 vs. 35 %, respectively; P = 0.02) (Van den Eynde et al. 2009).
RE significantly extended both OS and PFS in a prospective phase II trial that compared 29 patients with a higher tumor burden (20–50 %) from chemorefractory mCRC who were treated with 90Y resin microspheres, with 29 patients previously receiving contemporary chemotherapy who were given supportive care (Ricke et al. 2009). Patients in both arms had received a median of three regimens of prior chemotherapy (range 2–6), with no significant difference in their response to chemotherapy and biologic agents. Median PFS was increased from 2.1 months with supportive care to 5.5 months following 90Y therapy (P < 0.001), and median survival was also prolonged, from 5.5 to 8.3 months, respectively (P < 0.001) (Ricke et al. 2009). At three months, greater survival was clearly evident (59 vs. 97 %) and was sustained through 12-month follow-up (0 vs. 24 %). Furthermore, using multivariate analysis, RE was the most significant predictor of survival (P < 0.001). RE was also well tolerated; adverse events included thrombocytopenia and sepsis (3 %), and abdominal pain (3 %). Three possible cases of radiation-induced liver disease were managed medically and were not considered life-threatening (Ricke et al. 2009).
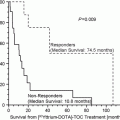
A prospective phase II multi-center collaborative-group trial was recently completed by the Società Italiana di Terapie Integrate Locoregionali in Oncologia (SITILO) collaborative group. In 50 highly chemorefractory patients with metastases solely or predominantly in the liver, all had failed prior oxaliplatin- and irinotecan-based chemotherapy regimens; more than 75 % had received four or more lines of chemotherapy (Cosimelli et al. 2008). Approximately 60 % of patients had >4 mCRC that involved 25–50 % of liver tissue. Following a single administration of 90Y resin microspheres, the ORR was 24 % (range 12.2–35.8 %), and stable disease (SD) was reported in a further 24 % of patients. Of particular note, two patients were sufficiently downsized to enable radical resection of more than three segments. The Kaplan-Meyer median OS was 13 months (range 7–18) with a 2-year survival of 19.6 %. The treatment response with 90Y resin microspheres was highly predictive of prolonged survival; the median 16-month survival among responders (range 13–19) was compared against the 8-month survival (range 4–12) among non-responders (P = 0.0006) (Cosimelli et al. 2008).
Similar data were reported in the US in a retrospective multicenter review of experience using 90Y resin microspheres (Kennedy et al. 2006). In 208 chemotherapy-refractory patients with measurable unresectable disease predominately involving the liver, 87 % of patients had previously received at least 3 lines of chemotherapy and 46 % had failed local–regional therapy (either resection; radiofrequency ablation [RFA]; hepatic artery infusion of chemotherapy; TAE; or TACE). At day 90 follow-up assessment after RE, computed tomography (CT)-measured tumor response was demonstrated in 35.5 % of patients and disease stabilization was shown in 55 % additional patients. Response by positron emission tomography (PET) was observed in 85 % of patients. These responses were again highly predictive of prolonged survival. Median survival was 10.5 months among responders versus 4.5 months for non-responders or historical controls (P = 0.0001) (Kennedy et al. 2006).
A second retrospective study of 41 patients with chemotherapy-refractory mCRC reported similar outcomes. The ORR was 17 % using response criteria in solid tumors (RECIST) with a median OS of 10.5 months following treatment with 90Y resin microspheres (Jakobs et al. 2008). Patients who developed a partial response (PR) or SD (29.3 and 10.9 months, respectively) experienced a significant survival advantage (4.3 months; P = 0.0001) over those with progressive disease.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree